
Quality education regarding best practices for managing the health and disease of older adults (OA) is needed. Interprofessional simulation education (Sim-IPE) is an active learning strategy that enables students from multiple professions to learn from, with and about each other to improve patient care. Student involvement in interprofessional educational events enhances valuable peer learning and engagement. This approach supports decision-making regarding a future geriatric care specialty and current challenges in care providers for OAs workforce. Escape rooms are an effective but resource-intensive Sim-IPE strategy. This essay describes the development and delivery of a workshop designed to support an interprofessional peer-to-peer educational project focused on the creation and delivery of an escape room educational experience concentrated on the 5Ms Framework (what Matters, Medication, Mentation, Mobility, Multicomplexity) of age-friendly care (AFC). The workshop promoted collaborative problem-solving and deeper engagement with OA care principles through peer-to-peer education.
What this essay adds
•Effective education on established frameworks for care of older adults (OAs), which is increasingly important as the population ages.
•Involving students in the development and delivery of educational initiatives focused on care of OAs engages them with the geriatrics specialty and may improve workforce challenges.
•Proof of concept for a novel escape room workshop designed to enable students to effectively create a peer-learning event.
•Peer-to-peer education and learning through student-developed escape room activities can benefit both student educators and interprofessional students.
•An escape room focused on an Age-Friendly Health System (AFHS) and Age-Friendly Care (AFC) for OAs, specifically the 5Ms framework of care, to support learning for interprofessional students.
The older adult (OA) population in America had its largest and fastest growth between 2010 and 2020. In 2020, individuals 65 and older comprised 16.8% of the US population [1]. Significant impact on healthcare systems is expected as the OA population is projected to increase by 44% by 2040, with those aged 85 and older increasing by 115%, and 100 years and above increasing by 100%. These changes in societal demographics are a challenge to healthcare providers and the healthcare system in general, especially in Arkansas (AR), where, in 2020, the OA population was 17.6%, higher than the US average [1].
Providing quality care in the context of this longevity is challenging [2]. Discontinuity of care amongst OAs can lead to errors and puts patient safety at risk [3]. Age-Friendly Healthcare (AFHC) and Age-Friendly Healthcare Systems (AFHS) are crucial to a person-centred approach to care of OAs [4]. Providing frameworks to healthcare professionals working within these systems can reduce cognitive load, ensure common language, support priority setting and provide evidence-based AFHC [3]. One such framework is the 5Ms (what Matters, Medication, Mentation, Mobility, Multicomplexity); centring this framework on ‘what matters’ enables prioritization of each OA’s choices, preferences and goals, embedding these within whichever care setting they are treated. Selection of age-friendly medications is important in the care of OAs. This includes adjusting medication dosing if needed and not prescribing high-risk medications that may negatively impact other Ms Mentation may also be referred to as mood and memory and focuses on the ‘prevention, identification, treatment, and management of dementia, depression, and delirium’ [3, page 469]. Mobility ensures an approach to assisting or encouraging OAs to move safely every day to maintain functional ability and do ‘what matters’. Lastly, multicomplexity recognizes the challenges presented in managing overlapping chronic disease processes and social and environmental factors through a more holistic approach to care. The 5Ms were selected as the subject matter for the escape room educational event given the importance and relevance to all healthcare learners. Integrating the 5M framework into care has been shown to improve health outcomes for OAs, optimize quality of clinical services, maximize cost-efficacy [4] and improve Merit-based Incentive Payment Systems (MIPS) when integrated into electronic medical records (EMR) [5,6].
As the population ages, the demand for high-quality education on evidence-based practices for managing health and disease in OAs [1]. The Arkansas Geriatric Education Collaborative (AGEC) is a Health Resources and Services Administration (HRSA) Geriatric Workforce Enhancement Grant (GWEP) designed to promote geriatrics-focused training and encourage health professions students to pursue careers caring for OAs. The AGEC provides free community and health professional programmes focused on healthy ageing and geriatric training and education. The AGEC’s Student Scholar Programme was developed to increase exposure and foster interest regarding care of OAs through interprofessional education (IPE). The Collaborative competitively recruits five interprofessional learners each year to become ‘scholars’. These AGEC scholars are second- to fourth-year students from the Colleges of Medicine, Pharmacy, Nursing, Health Professions and Public Health. This programme was established in 2020. The AGEC scholar programme includes participation in community-based experiences, structured didactic sessions, and the completion and presentation of a collaborative project wherein the scholars work together as an interprofessional team to create an educational event geared towards interprofessional providers and students.
IPE emulates healthcare professionals’ delivery of care. In 2000, the Institute of Medicine highlighted the importance of IPE in ensuring patient safety and the role of IPE in developing and achieving fundamental competencies for healthcare professionals [7]. The Interprofessional Education Collaborative (IPEC) was formed in 2009 and uses a strategic framework to advance the mission to ensure health professionals are proficient in competencies for ‘patient-centered, community- and population-oriented, interprofessional collaborative practice’ [8]. The four IPEC competency domains (values and ethics, roles and responsibilities, teams and teamwork and communication) provide the framework for IPE initiatives to work towards achieving competency [9]. A scoping review demonstrated a positive impact of IPE on multiple key quality health measures (length of stay, medical errors, patient satisfaction, patient or caregiver education and mortality) [10]. Of the 20 studies that assessed mortality, ten demonstrated reduced mortality with IPE interventions, and no studies identified worsened mortality.
Interprofessional simulation education (Sim-IPE) is an active learning strategy by which learners from two or more professions ‘learn about, from, and with each other to enable effective collaboration and improve health outcomes’ [8,9,11,12]. Escape rooms are one method to engage learners in a Sim-IPE experience and work towards achieving IPEC competencies, as they enable rehearsal of the four pillars: communication, teams and teamwork, roles and responsibilities, and values and ethics [8,9,11]. Escape rooms are immersive, puzzle-based activities designed to elicit analytical reasoning, creativity and collaborative problem-solving under time pressure. Participants work collectively to interpret clues, integrate diverse skill sets and progress through sequential challenges that culminate in a final task required to ‘escape’. Themes or narrative structures typically organize the puzzles, providing coherence and sustaining participant engagement throughout the activity. Functionally, escape rooms operate as structured problem environments in which learners must observe, hypothesize, test solutions and adjust strategies based on emerging information. Their reliance on communication, coordination and distributed cognition makes them well suited for team-based learning contexts. Escape rooms utilizing simulation for healthcare education can be conducted in multiple formats, for example, ‘within a simulation scenario, within the simulation/simulated environment, and/or with associated equipment’, and have key differences to escape rooms utilized in non-simulation education [13, page 10]. The design and educational mechanisms of escape rooms closely parallel established principles of simulation-based education [14]. Both modalities employ experiential, scenario-driven tasks within a controlled yet immersive setting to promote active learning, psychological safety and deliberate practice. Escape rooms require participants to make decisions, manage cognitive load and collaborate in real time, which are all competencies targeted in healthcare simulation. When coupled with structured debriefing, escape-room activities can reinforce key behavioural skills such as situational awareness, teamwork and problem-solving, supporting their integration as an adjunctive method within simulation-based curricula. The key feature of escape rooms within healthcare simulation is the use of core simulation principles, including striving for a safe and realistic learning environment wherein educators provide non-judgemental and constructive feedback while modelling openness of their own thoughts and experiences to normalize the learning process, which is crucial when considering, developing and delivering these events [13]. Sim-IPE escape rooms have been shown to improve interprofessional collaborative skills of health professions students [15], reinforce teamwork and communication in interprofessional learners with different levels of experience [16], and improve interprofessional socialization [17].
Though peer-assisted learning has been described across healthcare education literature, there is inconsistency regarding specific terminology to define levels and types of peer learning [18]. Learning activities described in this report are aligned with an IPE programme that employs a curriculum framework of exposure, immersion and competence phases of learning for novice, intermediate and advanced-level students, respectively. For purposes of this project, peer-to-peer learning is defined as instructional and collaborative learning among interprofessional learners at the same stage of disciplinary education. Near-peer learning is defined as instructional and facilitated learning wherein interprofessional students at a lower level of training are instructed by more advanced-level learners. Peer-to-peer education describes this structured approach wherein one group of students takes on the active responsibility of delivering new information or skills to novice learners.
Involving students in co-creation and delivery of escape rooms through peer-to-peer education may enable deeper understanding of subject matter and inspire students to continue in a role as future healthcare educators. It may also inspire students to engage with clinical specialties related to subject matter, such as the Age-Friendly Health Systems workforce. Peer-to-peer simulation-based education has been shown to be feasible and perceived positively by students, with benefits seemingly greater for peer teachers than for peer learners [19]. Students perceive near-peer-led simulation as valuable and engaging, with learners describing a range of benefits for learning, specifically pertaining to giving and receiving peer feedback, and learners reported confidence following the simulation education [18,20].
Peer-to-peer education is an effective strategy to ensure students thoroughly understand and can apply subject matter [19]. Escape room creation is complex and has rarely been used as a peer-to-peer educational opportunity. One study describes students aiding in the creation of an escape room for human physiology in which medical students submitted materials for the escape room that were then incorporated by faculty into the learning event [20]. While students were involved in event creation to some degree, this experience was neither student-led nor interprofessional – important aspects that may enhance learning potential based on peer-assisted learning and IPE literature. Peer-to-peer creation of this escape room and near-peer delivery of the Sim-IPE [21] is resource intensive in terms of time, effort and materials and may account for the lack of description within the published literature.
This report describes the development and delivery of a workshop-based learning experience for two interprofessional groups of students interacting in peer-assisted learning, AGEC scholars and IPE learners. A team of five advanced-level interprofessional students, the AGEC scholars, was supervised in a peer-to-peer learning activity to create and deliver an escape room Sim-IPE. This team of scholars then delivered the escape room as a near-peer teaching experience to IPE learners at an intermediate level of learning. The intermediate level IPE learners also participated in peer-to-peer education within their team while completing the Sim-IPE escape room and debriefing. The escape room was focused on the 5Ms of AFHC [22]. While there are some published examples of escape rooms to teach components of the 5M framework individually, such as medication and mentation [23,24], there is currently no published literature describing escape room learning providing a holistic framework for OA care to healthcare students or providers.
Representatives from the AGEC office reached out to the OIPE to explore a collaboration to support the AGEC scholars’ requirement to create an interprofessional learning activity. A workgroup comprised of a faculty member, a programme coordinator and a programme administrator from the AGEC and two faculty educators from the OIPE was formed. Under the supervision of this workgroup, for the first two years of the partnership, the AGEC scholars created a simulated participant (SP) simulation focused on the 5Ms of age-friendly care (AFC) [22,25] as the interprofessional project. A patient case was created in year one, and the patient story and scenario evolved to an updated time point with different priority items in year two. Scholars worked as a team asynchronously with feedback from faculty via e-mail or a shared document platform. Challenges associated with this collaborative method were lack of a sense of team amongst the scholars, progression of work in the timeframe and preparedness to deliver the final educational product. To increase scholar engagement and sense of collaboration, an additional formal needs assessment was performed. This incorporated feedback from previous scholars through survey and face-to-face meetings. Targeted needs assessment also included focus group discussions with key educators and faculty stakeholders within the AGEC programme to determine their opinions of next steps. Based on the needs assessment results, transition from the creation of an SP simulation to the creation of an escape room simulation educational event occurred. An escape room was chosen for the interprofessional learning project because the interactive nature and gamification offered a chance for peer-to-peer learning and teamwork not only between the AGEC scholars charged with designing the escape room activity but also for IPE learners who participate when the escape room is delivered as a simulation learning event. The escape room was then delivered to a group of interprofessional students as a pilot to evaluate the effectiveness of the design and assess any challenges. The AGEC scholars served as co-facilitators alongside OIPE faculty to deliver and assess the escape room activity in a near-peer learning format.
Two OIPE faculty members (KJD and KKN) created and delivered a workshop in which they facilitated five AGEC scholars creating an escape room learning event focused on the 5Ms of AFHC. The OIPE facilitators guided the scholar group towards a shared goal by making processes easier and more effective, including access to support materials and the virtual platform. The AGEC scholar team was comprised of one pharmacy student (fourth year), one medical student (third year), one physician assistant student (second year), one audiology student (third year) and one physical therapy student (third year).
A flipped classroom approach was selected to optimize scholars’ productivity and ensure a shared foundational knowledge, as it was unknown whether the scholars had previously attended or created escape rooms [26]. The workshop materials, goal, learning objectives/expectations and timetable are shown in Table 1 [27,28]. Scholars were expected to review the materials prior to the workshop. During the workshop, the scholars worked synchronously on a virtual communication platform (ZoomTM), utilizing document sharing (Google DocsTM) to produce an escape room with the goal of teaching interprofessional learners about the 5Ms of AFC [22,25]. Learning objectives and expectations for the scholars were set at the beginning of the workshop by the OIPE faculty. Workshop instructions introduced the content focus for the escape room the scholars were to create and related the alignment of this content with the institutional strategic mission to address falls and increase focus on fall prevention, one of the 5Ms – Mobility. The scholars were asked to create puzzles that focused on the 5Ms, with at least one puzzle per ‘M’ and at least two puzzles created for Mobility. OIPE faculty members (KKN and KJD) facilitated the scholars’ progress throughout the workshop, providing advice and guidance upon request.

| Flipped classroom material | Format | Created by |
|---|---|---|
| Presentation on the 5Ms of AFHC | PowerPoint presentation | AGEC Clinical Coordinator |
| Mobility/falls scenario template | Word document | AGEC Clinical Coordinator |
| Simulation Escape Room Workbook | Laerdal [27] | |
| Escape room example video | MP4 from a previous escape room run by OIPE | Office of IPE |
| Examples of escape rooms and puzzle ideas | Webpage | Healthy Simulation [28] |
| Goal: Work as a team to design an escape room for interprofessional (IP) learners, including all 5Ms of care of the OA, with particular emphasis on fall prevention/mobility. | ||
| Learning objectives: • Apply competencies for the four domains of Interprofessional Education and Collaborative Practice. • Review the four components of the Quadruple Aim. • Discuss interprofessional escape rooms as an approach to develop interprofessional skills and teamwork. • Develop an escape room appropriate for learning in an interprofessional team. |
||
| Expectations: By the end of the escape room workshop, AGEC scholars will: • Describe the process, underlying principles and components of escape room creation. • Design a themed escape room learning experience for IP learners around the 5Ms of care of the OA, including at least six puzzles (two of which focus on Mobility). • Identify and/or create: pre-course learning materials, learner instructions, escape room plan (including resources, puzzles, layout), learner assessment, event evaluation tool |
||
| Schedule and activities: | ||
| Time | Eventa | |
| 12:30–12:35 | Introduction and establishing scholars’ previous escape room experiences | |
| 12:35–12:50 | Overview of interprofessional simulation education | |
| 12:50–12:55 | Recap of the 5Ms of care of the older adult | |
| 12:55–13:10 | Introduction to escape rooms | |
| 13:10–13:30 | Overview and expectations of the workshop session, time for scholars to ask questions | |
| 13:30–15:00 | Scholars work together through workbook Chapters 2 and 3 Educator check-in at 13:50 to identify potential issues and stay on track |
|
| 15:00–15:10 | Check in with educators, recap, questions, time for break | |
| 15:10–15:45 | Scholars work together through workbook Chapters 4, 5 and 6 Educator check-in at 15:20 to identify potential issues and stay on track |
|
| 15:45–15:55 | Check in with educators, recap, questions, time for break | |
| 15:55–16:10 | Scholars work together on creating learner assessment and event evaluation. Templates provided by the educator team as examples. | |
| 16:10–16:30 | Debrief and work on next steps (scheduling the dry run and escape room session for IP learners) | |
a During scholars’ work sessions, IPE faculty (KJD and KKN) remained present in the virtual room, with cameras off and muted, but available to provide assistance if needed.
Scholars utilized an escape room workbook as a template for how they would create this learning event (Table 1). They worked through the ‘essential pillars’ of creating a simulation escape room – namely, participants (who are the learners?), objectives, theme, puzzles, equipment and evaluation. The scholars’ time within the workshop was split between the sections of the workbook to cover: planning, objective setting, outlining the escape grid (how the learners will take an escape route through the puzzles to escape the room), designing (including developing a theme and puzzle content/clue sequence), facilitating (how the facilitators will work together), debriefing (including strategies and prompt questions) and creating a resource list.
At the workshop conclusion, the scholars had worked through the escape room workbook [27] and created an outline and timetable for the escape room event, the puzzles, a map of the escape room, a list of equipment required and an event evaluation tool. A central theme of a ‘Winter Wonderland’ emerged for the room resulting from a prompt to consider a seasonal approach, and the workshop occurred in early December. Orientation and clues for the room were introduced in a poem based on the Twelve Days of Christmas. As each puzzle was solved, a piece of the Grinch’s heart needed to complete the final puzzle was also obtained. In keeping with the winter holiday theme, the Grinch’s heart (based on Dr Seuss’ holiday character) was chosen as the global puzzle so that as the learners solved puzzles successfully, the Grinch’s heart grows, signifying him realizing the importance of interpersonal connections – crucial to the What Matters part of the 5Ms (Figure 1). Assembly of the Grinch’s heart revealed a sequence of colours which cross-mapped to a numeric series that provided the code to unlock a lockbox containing the key to escape the room. Puzzles created by the scholars for the escape room included those that incorporated the following assessments: the ‘Timed Up and Go’ (TUG), a falls risk self-assessment [29] and the Berg Balance Test for Mobility; the Mini-Mental Status Examination (MMSE) and Mini-Cog clock test for mentation; medications review; and the Grinch heart with pictures symbolizing what matters most. Examples of puzzles are shown in Table 2. The AGEC scholars created learning objectives for the escape room Sim-IPE focused on the IPEC competency domains, patient- and family-centred care (PFCC) core principles and the 5Ms. Learning objectives specific to the 5Ms included: describe potential causes of falls in OAs and the systems involved (e.g. auditory, somatosensory, vestibular), describe the clinical evaluation for conducting a falls risk assessment and plan of care, and discuss and develop a future fall prevention plan including resources in/outside of the university hospital system.

| 5Ms aspect addressed | Puzzle details |
|---|---|
| Mobility | The last line of the opening poem clue reads, ‘On the 12th day of Christmas my PT gave to me, a TUG test’. This clue leads students to identify an area in the room where a chair is placed and a line of footsteps leading to a large Nutcracker figure are located 10 feet away. Once they complete the TUG test successfully, the learners get their next clue. |
| Mobility, Multicomplexity | Upon completing the TUG test, students locate a card reading, ‘Your time was 12 seconds’. The ‘12’ is a clue to identify a stocking in the room with the number 12 on the front, from a range of stockings visible. The 12 stocking contains a Grinch heart piece, a falls risk assessment, which leads students to identify the patient, is at risk of falls, and they should remove trip hazards from the room. |
| Mobility | As the students remove the trip hazards, a string of holiday lights contains a heart piece and a QR code that leads to a website with the BERG balance test. |


The unifying puzzle of the escape room – the Grinch’s heart
At the workshop conclusion, the scholars shared an electronic link to their escape room files with educators. In January (one month post-workshop) members of the OIPE completed a run-through of the room using a tabletop layout to troubleshoot and finalize puzzles and supplies. A dry run of the escape room was completed by the OIPE team in early February during which the necessary supplies were assembled and several options for room layout were discussed and tested with a randomly recruited volunteer medical student from a nearby study area.
The Sim-IPE was delivered as an in-person pilot in late February. The schedule consisted of setup/pre-huddle (1 hour), orientation to the Sim-IPE escape room expectations (15 minutes), brief lecture on the 5Ms and several assessments used in the care of OAs (15 minutes), the escape room activity (1 hour), debrief and event evaluation for IPE learners (30 minutes) and debrief and overall IPE project evaluation for AGEC scholars (30 minutes). OIPE faculty (KJD and KKN) and AGEC scholars completed the ‘pre-huddle’, during which the event timeline, materials and presentation outlines were discussed. A walkthrough of the room was completed, and roles and responsibilities of all facilitators (OIPE faculty and AGEC scholars) for the event were discussed. The AGEC scholars were responsible for delivering education to IPE learners on the 5Ms of AFHC and participating as co-facilitators with the OIPE faculty for the IPE learners’ simulation debrief.
Four IPE learners (two medical, one nursing, one physician assistant) participated in the pilot delivery of the Sim-IPE. These four participants opted in to the event by selecting it from a sign-up schedule of IPE curriculum simulation activities for the Spring semester. Following IPE learners’ completion of the simulation and ‘escape’ from the room, a debrief was conducted, using the plus-delta debriefing model [30]. Finally, after conclusion of the Sim-IPE event, the OIPE faculty facilitated a peer-to-peer event debrief in which the AGEC scholars reflected on the totality of their IPE project to design and deliver the escape room.
Evaluation for this pilot project included two target audiences – AGEC scholars who designed and delivered the Sim-IPE escape room, and the IPE learners who completed the Sim-IPE escape room learning event. Recognizing that this is a small pilot study, it is intended that evaluated endpoints for both AGEC scholars and IPE learners are descriptive in nature only to enable lessons learned to be distilled. Evaluation time points are shown in Figure 2.

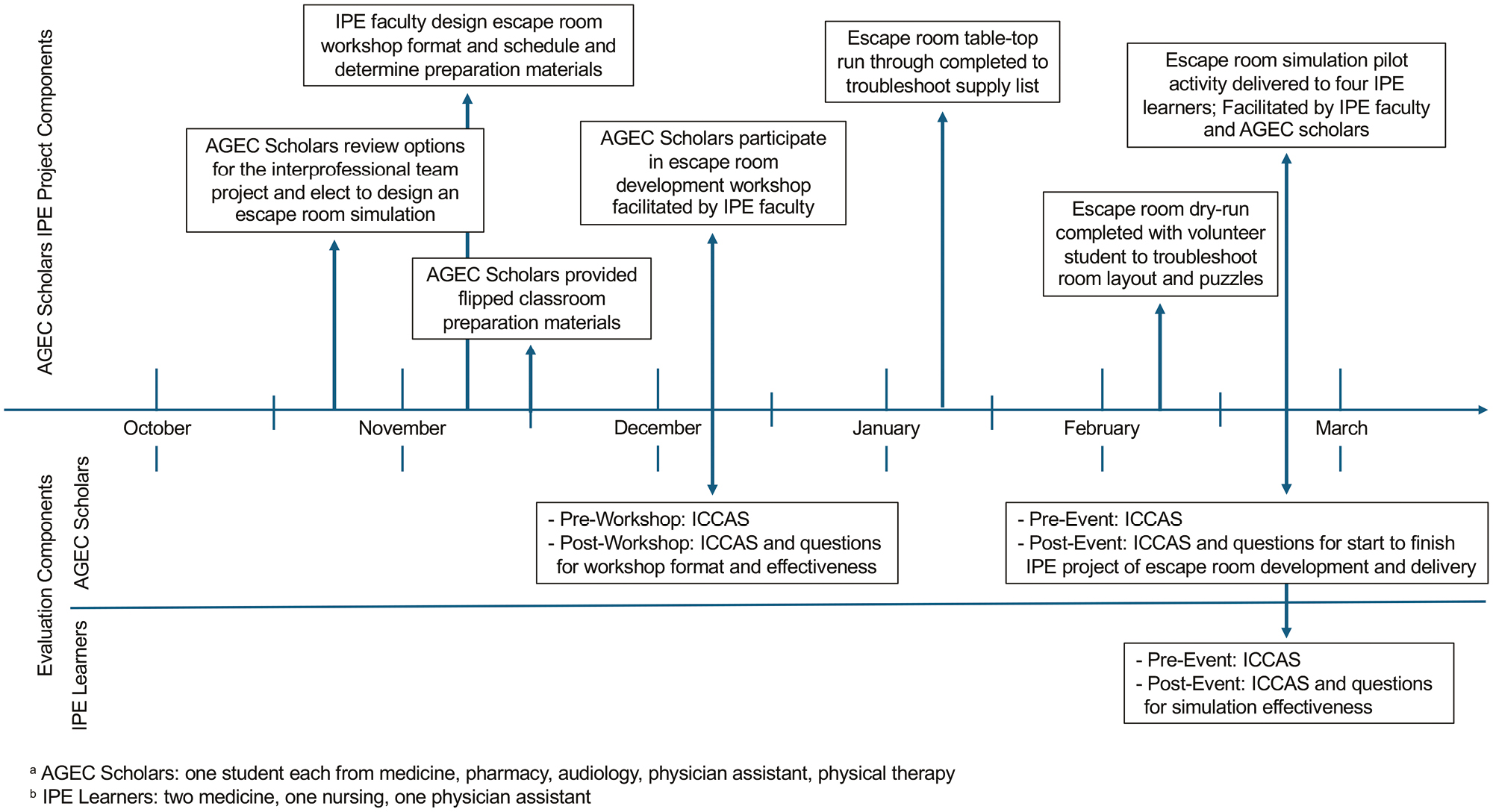
Timeline for AGEC scholars’ escape room project
To evaluate the five AGEC scholars’ impressions of their IPE project to design and deliver an escape room, quantitative and qualitative questions were employed. Evaluation focused on two components – (1) the escape room creation workshop as a single event and (2) the overarching interprofessional learning project to design and then deliver and reflect on the efficacy of the Sim-IPE escape room. Data were collected at four time points – before and after the escape room creation workshop and before and after delivery of the Sim-IPE escape room learning activity (Figure 2).
Quantitative assessment included Likert-scale questions to evaluate project development goals, instructional materials, delivery format and perceived effectiveness of the Sim-IPE and the Interprofessional Collaborative Competency Attainment Survey (ICCAS) to evaluate perception of interprofessional skills. The ICCAS is a validated instrument with 20 questions measuring perceived skill for six performance domains: communication, collaboration, roles and responsibilities, collaborative patient-and family-centred approach, conflict management/resolution and team functioning [31]. The original survey used a 7-item scale (1 = strongly disagree to 7 = strongly agree). The tool was then revised to use a 5-item scale (1 = poor to 5 = excellent) [32]. The 7-item scale was used to record AGEC scholars’ responses. Assessment points occurred pre- and post- the escape room creation workshop and pre- and post- the Sim-IPE escape room event. Qualitative evaluation was comprised of open-response questions.
The post-workshop survey reflected scholars’ perceived improvement in interprofessional competency skills from pre- to post- for all six ICCAS domains with an average increase of mean scores pre-/post-workshop of 43% (Figure 3). Response rate was 100%. Scholars’ impression of the efficacy of the workshop in addressing interprofessional collaboration and communication skills, learning objectives and general impressions were all favourable with mean scores ranging from 4.5 to 4.8 (out of five maximum) (Table 3). Scholars’ overall impressions of the value of the workshop and their knowledge and ability to create an escape room or other interprofessional learning activity also rated highly.

| Mean scoreb n = 4 | Mean scorec n = 5 | |
|---|---|---|
| Interprofessional collaboration and communication – the escape room workshopb/projectc: | ||
| increased my knowledge of another profession/s. | 4.5 | 4.6 |
| improved my teamwork skills. | 4.5 | 4.8 |
| helped me identify where I can improve my communication with other professionals. | 4.8 | 4.8 |
| helped me identify where I can improve my communication with patients/public. | 4.5 | – |
| helped me identify where I can improve my communication with student learners. | – | 4.8 |
| The escape room workshopb/projectc addressed the following learning objectives: | ||
| Apply competencies for the four domains of Interprofessional Education and Collaborative Practice. | 4.8 | 4.6 |
| Review the four components of the Quadruple Aim. | 4.8 | 4.6 |
| Discuss interprofessional escape rooms as an approach to develop interprofessional skills and teamwork. | 4.8 | 4.8 |
| Develop an escape room appropriate for learning in an interprofessional team. | 4.8 | 4.8 |
| General impressions – the escape room workshopb/projectc: | ||
| had a positive effect on my attitude towards IPE. | 4.8 | 4.8 |
| in general, I learned something important. | 4.5 | 4.8 |
| in general, was an effective use of my time. | 4.8 | 4.8 |
| was helpful to organize and develop an interprofessional escape room. | 4.5 | – |
| was helpful to understand the intersection of design vs. implementation (what you intended vs. what happened). | – | 4.8 |
| scheduled check-ins during the workshop were helpful to guide progress and complete work in the allocated timeline. | 4.8 | – |
| overall format and scheduled agenda/prompts for the escape room were helpful to guide progress and complete work in the allocated timeline. | – | 4.6 |
| Overall – the escape room workshopb/projectc: | ||
| overall, I believe was a valuable education activity. | 4.8 | 5.0 |
| demonstrated the value of participating in team-based education. | 4.8 | – |
| demonstrated the value of participating in team-based educational design. | – | 5.0 |
| demonstrated the value of providing team-based care/research. | 4.8 | 4.8 |
| increased my knowledge and appreciation for creating effective interprofessional learning activities, i.e. teacher/facilitator role in creating classes/activities. | 4.8 | 4.8 |
| I am confident that I can create escape room activities in the future. | 4.3 | 4.8 |
a Post-event surveys used repeated questions with minor modifications based on the time point in the project. Survey used a 5-point Likert scale using 1 – Strongly disagree, 2 – Disagree, 3 – Unsure, 4 – Agree, 5 – Strongly agree.
b Data collected post-escape room creation workshop, n = 4 (one student did not respond).
c Data collected post-Sim-IPE pilot event (n = 5), scholars were asked to reflect on the overall team project to design, deliver and assess the escape room Sim-IPE.

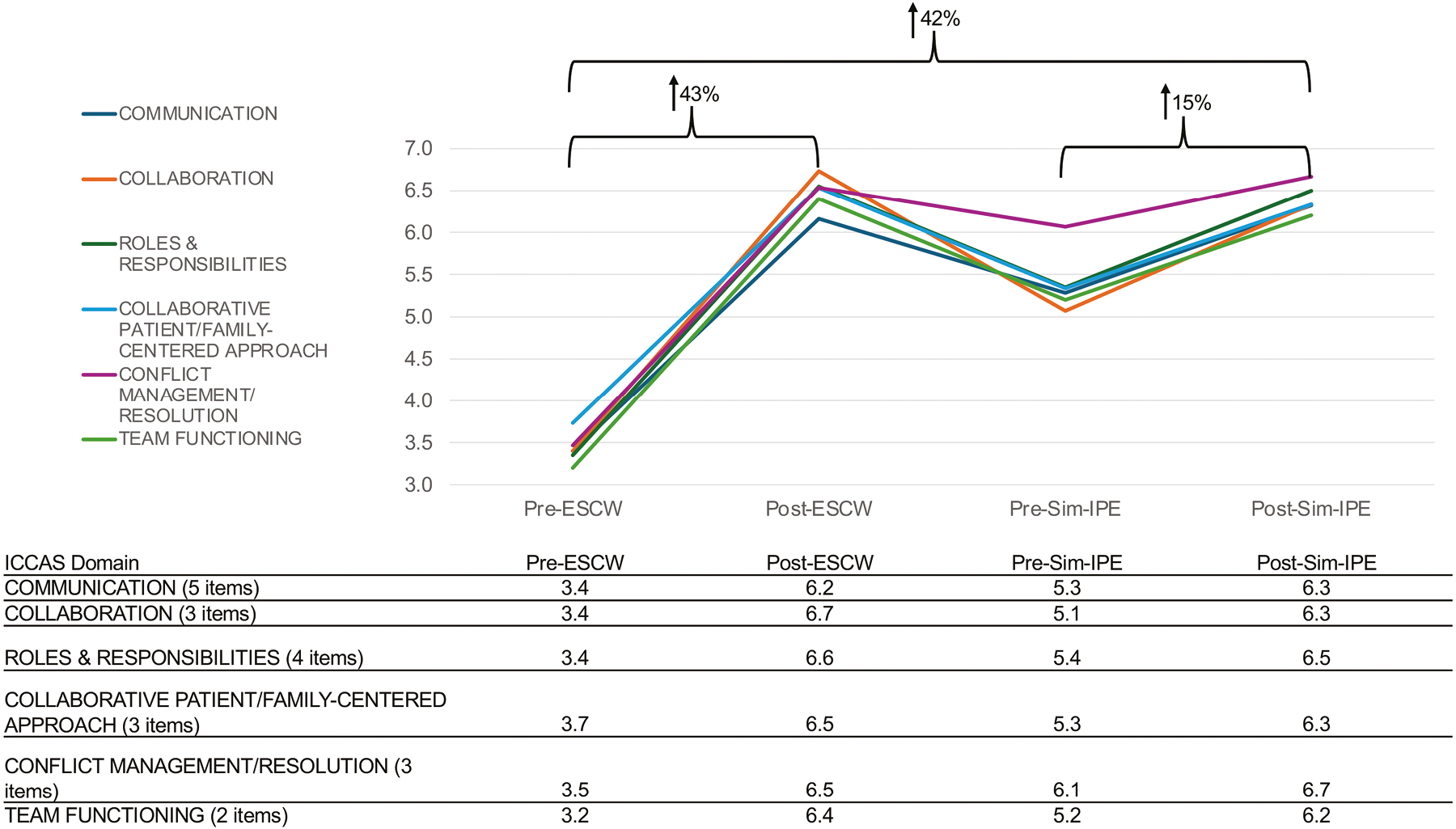
ICCAS domain scores for AGEC scholars
Qualitative feedback was solicited with three open-response questions: Please identify the most effective aspects of the Escape Room Creation Workshop and indicate why they were effective. Please identify the least effective aspects of the Escape Room Creation Workshop and indicate why they were ineffective. Please identify one thing you would have liked to have learned in the Escape Room Creation Workshop but did not. Representative comments identifying the most effective parts included ‘it was FUN. I did not mind it taking up Friday afternoon because of the content’, ‘Zoom collaboration was effective as we were all actively working on the content together’. Scholars also appreciated using the workbook to prevent being overwhelmed and to provide them with escape room and puzzle examples and structure. To improve subsequent offerings, scholars noted virtual communication was sometimes challenging with multiple speakers, and the opportunity to physically lay things/test things out (e.g. puzzles) may have been helpful.
The ICCAS was repeated proximate to the Sim-IPE escape room activity to evaluate scholars’ temporal perception of interprofessional skills. Figure 3 represents changes seen at different points of the ICCAS administration. Mean ICCAS domain scores just prior to the Sim-IPE delivery indicated scholars’ perception of their interprofessional skills remained higher than mean scores prior to the escape room creation workshop, though they had waned slightly from post-workshop values. The ICCAS was repeated proximate to the Sim-IPE escape room activity to evaluate scholars’ temporal perception of interprofessional skills. Mean ICCAS domain scores just prior to the Sim-IPE delivery indicated scholars’ perception of their interprofessional skills remained higher than mean scores prior to the escape room creation workshop, though they had waned slightly from post-workshop values.
The post-survey following the Sim-IPE event served as scholars’ final evaluation point. The group was asked to reflect on the totality of their experience in the IPE team project. In addition to repeating the ICCAS, a 5-point Likert scale evaluated scholars’ impressions of serving as an educator and the results of the Sim-IPE escape room they designed. ICCAS mean scores at this final time point were increased for all items from those obtained just prior to the Sim-IPE, indicating the process of serving as a facilitator for the educational activity and reflecting on the effectiveness of the event also contributed to perceived interprofessional skill development. The average increase of ICCAS mean scores from pre-Sim-IPE to post-Sim-IPE was 15% (Figure 3).
Scholars rated their experience in delivery of the Sim-IPE escape room highly (Table 3). They perceived the Sim-IPE escape room development project was successful in addressing the intended learning objectives and taking on the role of educator ‘was helpful to understand the intersection of design vs implementation’. All scholars provided the highest rating of ‘5 – Strongly agree’ that ‘Overall, I believe this was a valuable education activity’ and all agreed/strongly agreed they are ‘confident I can create escape room activities in the future’.
Qualitative evaluation in the post-Sim-IPE survey incorporated three open-response questions: Please identify the most effective aspects of participating as an educator for the Escape Room session and indicate why they were effective. Please identify the least effective aspects of participating as an educator for the Escape Room session and indicate why they were ineffective. Please identify one thing you would have liked to have learned participating as an educator in the Escape Room session but did not.
Scholars noted ‘implementing the assessment tools (e.g. TUG/Berg Balance) into the simulation and describing their use/how to administer them’, and using ‘the emphasis with the “what Matters” to pull all of the Ms together’ as the most effective aspects of the session. Scholars noted the following least effective aspects of their escape room: ‘multiple numbers of colors [across puzzles] that could confuse and easily get a group off track’ and ‘not using the MoCA/SLUMS into one of the pieces to describe its usage’ (i.e. using a partial test for mentation [clock drawing] assessment instead of the longer assessment [Montreal Cognitive Assessment (MoCA), Saint Louis University Mental Status Examination (SLUMS)]). For items scholars wished they had learned during the experience but did not, one indicated ‘more in depth of depression in older adults for students to better understand mental health of OAs and their caregivers’ and another said ‘it might have been good to learn more about social work’s involvement in cases like this’.
Scholars’ ICCAS evaluation items indicated the peer-to-peer group project among the five-member scholars’ team was successful in increasing their perceived interprofessional competency (Figure 3). From an overarching start-to-finish IPE team project perspective (pre-workshop to post-Sim-IPE), scholars’ perception of interprofessional competency as reflected by ICCAS domain scores increased an average 42%. Additionally, scholars’ high level of confidence that they can create escape room learning activities in the future supports employing the IPE project format for future iterations in the AGEC Scholar programme to support interprofessional skill development within the scholar team.
To assess the effectiveness of the Sim-IPE escape room pilot session, a mixed-methods approach to data collection was employed. IPE learners completed a pre-survey before the escape room consisting of demographics (school, programme) and the ICCAS version using a 5-item scale [31,32]. A post-survey immediately after the Sim-IPE escape room repeated the ICCAS and incorporated a 5-point Likert scale to evaluate IPE learners’ perception of the effectiveness of the Sim-IPE to develop their knowledge and skills and overall satisfaction with the simulated environment. Qualitative evaluation employed two open-response questions: What aspects of the learning experience did you find most valuable? Please share any other comments about this learning activity.
IPE learners’ perception of their interprofessional competency increased from pre- to post- in all ICCAS domains (Table 4). Learners believed the escape room was effective in increasing their comfort and confidence to use the 5Ms framework. They agreed the escape room made them ‘more comfortable in my ability to address the 5M’s in my clinical practice’. All four learners provided the highest rating of ‘5-Excellent’ that the activity ‘demonstrated the value of providing a team-based fall prevention assessment by targeting the 5M’s of health care in an older adult’s life’. Responses to open-response questions included ‘I found the active participation and thinking on our feet more helpful and with other healthcare workers than just discussion’, ‘the escape room in general helped make the content stick’ and ‘working together as a team to figure out the puzzles… helped to develop our communication skills’.

| ICCAS competency developmenta | Pre | Post | % diff | Simulation and debriefing | Mean scoreb |
|---|---|---|---|---|---|
| Communication | Experience was valuable. Helped me apply my knowledge. Helped me gain confidence. Developed my communication skills. Developed my reasoning skills. Developed my decision-making ability. Facilitator(s) made me feel at ease during the debriefing. Reflection on my performance helped me to learn. Learners were actively engaged in the debriefing. I learned strategies for improving performance. Important steps to apply to future practice were summarized. Debriefing was helpful in my development as a professional. |
4.8 4.8 4.8 4.5 4.5 4.3 4.8 5.0 5.0 4.8 4.8 5.0 |
|||
| Promote effective communication among members of an IP teamc Actively listen to IP team members’ ideas and concerns Express my ideas and concerns without being judgemental Provide constructive feedback to IP team members Express my ideas and concerns in a clear, concise manner |
4.0 4.3 4.5 3.5 4.0 |
4.5 5.0 5.0 4.3 4.8 |
10 15 10 15 15 |
||
| Collaboration | |||||
| Seek out IP team members to address issues Work effectively with IP team members to enhance care/research Learn with, from and about IP team members to enhance care/research |
3.3 3.8 3.8 |
4.5 4.5 4.8 |
25 15 20 |
||
| Roles and responsibilities | |||||
| Identify and describe my abilities and contributions to the IP team Be accountable for my contributions to the IP team Understand the abilities and contributions of IP team members Recognize how others’ skills and knowledge complement and overlap with my own |
4.0 4.3 3.5 3.8 |
4.8 4.8 4.5 5.0 |
15 10 20 25 |
Escape room learning objectives | |
| I feel more comfortable in my ability to address the 4Ms in my clinical practice more than I did prior to this activity. I feel more comfortable in my ability to identify the needs of older adults regarding mobility, medications, mind and what matters most. This activity demonstrated the value of providing team-based fall prevention assessment by targeting the 4Ms of healthcare in an older adult’s life. |
4.8 4.8 5.0 |
||||
| Collaborative patient/family-centred approach | |||||
| Use an IP team approach with the patientd to assess the health situation Use an IP team approach with the patient to provide whole person care Include the patient/family in decision-making |
3.0 3.5 3.5 |
5.0 5.0 4.5 |
40 30 20 |
||
| Conflict management/resolution | SE-simulated environment | ||||
| Actively listen to the perspectives of IP team members Take into account the ideas of IP team members Address team conflict in a respectful manner |
4.0 4.3 4.0 |
4.8 5.0 4.8 |
15 15 15 |
Portrayed the simulation well. Gave clear instructions regarding background information. Contributed to a safe learning environment. Provided an effective mechanism to learn using the 4M framework. |
4.5 4.8 5.0 4.8 |
| Team functioning | |||||
| Develop an effective care/researche plan with IP team members Negotiate responsibilities within overlapping scopes of practice |
3.5 3.3 |
4.3 4.5 |
15 25 |
||
| Overall | |||||
| Overall, I believe this was a valuable education activity. | 4.8 | ||||
a ICCAS using a 5-item scale (1 = poor; 2 = fair; 3 = good; 4 = very good; 5 = excellent) [25,26].
b Based on a 5-point Likert scale using 1 – Poor, 2 – Fair, 3 – Good, 4 – Very Good, 5 – Excellent.
c The patient’s family or significant other, when appropriate, is part of the IP team.
d The word ‘patient’ has been employed to represent client, resident and service users.
e The term ‘care’ includes intervention, treatment, therapy, evaluation, etc.
At a time when the world population is ageing, it has never been more important to effectively educate healthcare students about issues surrounding delivery of AFC. Engaging students in the creation of Sim-IPE events provides an opportunity for progression through the levels of Bloom’s taxonomy [33,34], development of IPEC core competencies and engagement with varied clinical specialties, depending on the focus of the Sim-IPE. This can be particularly helpful in specialties where workforce issues have been identified or can be anticipated. Both AGEC scholars and IPE learners appreciated the active learning component of the escape room format and felt that creating (scholars) and solving (IPE learners) the puzzles would help them retain subject matter. Perceived interprofessional skill development began early in the scholars’ project, as indicated by the comparative increase in ICCAS scores pre-/post- the escape room creation workshop. Creation of the escape room by the AGEC scholars gave them an opportunity to build upon not only knowledge for assessing OAs but also to grow further in their interprofessional relations and competencies. Though mean ICCAS scores waned slightly between the escape room creation workshop and the Sim-IPE delivery, scores rebounded following the Sim-IPE, yielding an overall 42% increase considering the AGEC scholars’ total project experience of creating and delivering the escape room. There was an increase in mean ICCAS scores pre-/post- the escape room Sim-IPE for IPE learners. The difference in ICCAS mean scores for the different learner groups may be influenced by several factors, including scholars’ depth of experience with the learning content related to OAs and longer duration of partnerships in the collaborative team during the longitudinal project. Additionally, a potential confounder is students recruited to the scholar positions were more advanced compared to the IPE learners who were considered intermediate level in programme progression.
Despite challenges, when appropriately supervised, we demonstrate that using a synchronous workshop approach for escape room creation can be a positive and not overwhelming experience for students. A virtual platform can facilitate these creation workshops, enabling connection of students from different sites, as well as connection to preceptors to guide the process. It also provides students with the ability to share documents electronically and create the escape room in real time during the workshop. However, as noted in the AGEC scholars’ evaluations, if students are geographically close, an in-person workshop may facilitate rehearsal of puzzle feasibility. This could enable streamlining and possible elimination of the subsequent tabletop or dry run portions of the process. It is for this reason, that is, the hands-on nature of the escape room experience and puzzles, that this education was designed to be delivered in person. It would be possible to create a virtual escape room educational experience, but this would need to be a clear goal embedded within the scholars’ workshop and objectives modified so that all puzzles were designed to be completed on the computer, as a team, ensuring the necessary software was available to all, for example, whiteboard function in Zoom, shared access to working Google Drive, etc.
Escape rooms in general have a theme, which is used as part of the context to identify clues and solve puzzles. For the current example, the Grinch’s heart symbolizes the recognition of what is really important to someone and that which brings them joy (i.e. what matters to OAs).
In recognition that all education might not resonate with all learners, we give information about each curricular event at signup, including notes to indicate the content and theme. This enables learners to select an event aligned with their preference. Those of non-Christian traditions who do not desire to complete a Winter wonderland/Christmas-themed event could then choose an alternate event. A similar event could be designed around Hanukkah, Ramadan, etc. In that respect, themes can increase exposure to other traditions as learning opportunities.
Developing and delivering an escape room stimulated critical reflection from the scholars, for example, detailing ways in which the initiative’s educational quality could be improved. Specifically, scholars suggested the inclusion of a more complete assessment for one of the puzzles rather than a portion (the MoCA/SLUMS), incorporation of a mental health assessment and the social workers’ perspectives. These suggestions demonstrate not only depth of understanding of the subject matter but also interprofessional processes and competencies.
The workshop described herein provides guidance for the creation of similar events, structured around pertinent subject matter, guided by needs assessment. The success and efficacy of these workshops are contingent upon the experience of facilitators and student engagement. It is essential that educators have an appreciation of and familiarity with the creation and delivery of escape rooms to effectively guide novice students through the process, develop appropriate goals and learning objectives, and supervise content and puzzle creation. Utilizing pre-existing tools, such as the referenced workbook, can reduce educator workload without compromising the quality of the experience for students. Existing resources can be adapted to local needs and health targets.
Implications related to this work include recognizing escape rooms are resource-heavy when considering the relatively small number of learners who can participate in each event unless the facility has the capability to run multiple simultaneous escape rooms, and they are also facilitator intensive. To help increase participant capacity, strategies to increase throughput by adding skills stations are under development. Students will alternate between the Sim-IPE escape room and practical stations where they rehearse performance of assessments for OAs. This enables students to experience the tests they will perform on their OA patients, hopefully improving their appreciation of the learning content and experience and empathy for the OAs they treat.
Effective education on best practices in age-friendly healthcare is essential as the population ages. Involvement of students in the development and delivery of educational initiatives focused on OA care is one way for them to engage with the geriatric specialty and may improve workforce challenges by increasing exposure to the field. Peer-to-peer education is also a powerful tool to consolidate knowledge of subject matter and IPEC competencies. This report describes effective development and delivery of a novel escape room workshop, with appropriate faculty preceptorship, to enable students to effectively create a peer-to-peer IP educational event. The process enhanced scholars’ appreciation of IPEC competencies and the 5Ms of AFC and was able to translate IPE to learning. This model may inform future interprofessional educational initiatives aiming to build geriatric care capacity and support workforce development in ageing populations.
We acknowledge and thank Wendy K. McCloud, Instructor and Interprofessional Education Manager, and Misty Besancon, Programme Administrator, in the University of Arkansas for Medical Sciences (UAMS) Office of Interprofessional Education for their help in implementing this activity through educational platform support, escape room refinement and delivery, and data collection. We also acknowledge the creative work of the AGEC Scholars: Melanie Beehler (Medicine), Margaret Boles (Physician Assistant), Holland Hardison (Audiology), Lizeth Martinez-Lopez (Physical Therapy) and Jasmine Wilson (Pharmacy), in the design and delivery of the described escape room.
The Association for Simulated Practice in Healthcare (ASPiH) have supported the publication of this work through their fee waiver member benefit.
KJD, KKN: conceptualization, methodology, software, data curation, writing – original draft preparation, reviewing and editing, visualization, investigation, supervision. LRTM, LS: conceptualization, writing – reviewing and editing.
The UAMS Arkansas Geriatric Education Collaborative (AGEC) is funded by the Health Resources and Services Administration’s Geriatric Workforce Enhancement Programme under grant #U1QHP28723.
Due to the nature of this work, participants did not consent to their data being shared publicly, and therefore supporting data are not available.
This project has been reviewed by the University of Arkansas for Medical Sciences Institutional Review Board and determined NOT human subject research as defined in 45 CFR 46.102 and therefore exempt.
The authors have no conflicts of interest to declare.
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.