
The ability to gain access to the peritoneal cavity and perform dependable fascial and skin closure is foundational in surgical training. We developed and evaluated a realistic, low-cost synthetic abdominal wall simulator incorporating a biomechanically similar fascial layer.
We iteratively engineered a layered abdominal wall model in an 18 × 18 cm frame using pigmented silicone elastomers and a nylon/spandex power mesh to emulate fascia, muscle, adipose tissue and skin. Ten practising surgeons at a US academic military hospital performed a midline laparotomy and closure on the device and then rated realism (palpation, incision, grasping, suturing, stapling) and the model’s acceptability for training. Cost and build time (including cure intervals) were recorded.
Tooling cost for the reusable mould and rectus frame was approximately $125, with $34.38 in materials per additional unit. Using two frames, manufacture time was ~21 hours, driven by cure times across layers. After use, nine out of ten surgeons rated palpation, incision and suturing as somewhat similar or similar to living tissue; six out of ten rated grasping as somewhat similar or similar; eight out of ten rated skin stapling as somewhat similar or similar; ten out of ten judged the simulator acceptable for teaching midline laparotomy; and nine out of ten judged it acceptable for teaching fascial closure.
Our construct provides a reproducible, inexpensive simulator for teaching laparotomy creation and closure using widely available materials. Surgeon ratings support acceptable face realism and broad training utility, with grasping fidelity identified as a target for refinement. Future work should incorporate trainee perspectives, multi-institutional testing and iterative material adjustments to optimize handling characteristics.
The ability to surgically gain access to the peritoneal cavity and to perform a proper closure are fundamental general surgery skills. Failure to perform adequate fascial closure results in incisional hernia, a significant cause of neuromuscular disability for which an estimated 350,000 patients require surgical intervention in the United States annually [1–3]. With graduating United States general surgery residents on average spending less than 15% of their total work hours over a 5-year residency as chief surgeon in the operating room, and simulation demonstrating clear benefits for skills-based training, surgical simulators have risen to the forefront as critical adjuncts in the technical education of the general surgery resident [4–8].
Laparotomy creation and closure can be taught using animal models or using high-end commercially available synthetic models, but perceptions among both trainees and the public of animal-based approaches are mixed, and currently available synthetic models are associated with significant, often prohibitive cost [9–12]. Cadaveric simulation remains another option but currently lacks evidence demonstrating skill retention or transfer of skills into the operating theatre [13].
As traditional surgical training continues to evolve in response to the challenges of patient safety, financial considerations and concerns over decreased autonomy, the role for simulation in surgical education is expected to grow [4,14]. We sought to develop a realistic simulated abdominal wall that could be easily manufactured using simple materials and at a cost that would allow mass production at any programme interested in making copies for the purpose of teaching laparotomy creation and abdominal closure. We based our model on our group’s previously developed synthetic fascia.
The Construct for Laparotomy Opening and Suturing (CLOS-IT) was built on the foundation of our group’s previously developed biomechanically realistic synthetic fascia [15]. Above this layer, we added different formulations of dyed Ecoflex silicone compounds to simulate the skeletal muscle, adipose tissue and skin moulded in an 18 × 18 cm frame. This construct was presented to an attending colorectal surgeon and a general surgery resident for simulated laparotomy, and feedback on the device’s realism and areas for improvement was obtained. In a process analogous to the Interservice Procedures for Instructional Systems Development (IPISD) model, successive cycles of surgeon and resident feedback and model revision were used to gradually hone and refine each tissue layer over multiple iterations to achieve the final product that is presented here [16].
The mould used included an interior cross-shaped frame designed to give shape to the recti abdominis and delineate the linea alba. The fascial layer measured 1.5 mm in thickness and consisted of three plies of Power Mesh Stretch Nylon Spandex 100GSM (Fabric Wholesale Direct, Farmingdale, NY) set in Dragon Skin 30 silicone (Smooth-On Inc., Macungie, PA). This layer was used to simulate the anterior rectus sheath, upon which we created a 10 mm thick rectus abdominis layer using Ecoflex 00-30 silicone tinted with Silc Pig blood-coloured dye (both from Smooth-On Inc., Macungie, PA) and moulded using the cross-shaped member described above (Figure 1a). The adipose tissue layer measured 15 mm and was created using a layer of Soma-foam (Smooth-On Inc., Macungie, PA), and fixed to the anterior rectus sheath using a layer of clear silicone adhesive. The skin layer measured 3 mm in thickness and was created by setting a single layer of Power Mesh in Ecoflex 00-30 silicone tinted with Silc Pig flesh-coloured dye. Of the above formulations, all retain their starting volumes during the curing process with the exception of the Soma-foam (adipose layer) which expands to about three times its initial volume. The skin layer was fixed to the simulated adipose tissue with a layer of clear silicone adhesive. A standard, 7-qt plastic hospital wash basin was fashioned into a mounting surface by cutting a roughly 12 × 15 cm rectangular hole in the bottom, and two holes on either side through which to tie down the manufactured components described above. The basin was inverted, and the silicone and simulated abdominal wall were mounted on top, fastened with two lengths of string laced through the two sets of holes.


(a) Rectus abdominis layer curing within 3D-printed mould. (b) Collection of various tissue layers prior to final assembly. (c) Unmounted, fully cured product with overlying skin
To assess the realism of the CLOS-IT and its utility for teaching laparotomy opening and closure an online survey was created. In order to obtain as granular data as possible with respect to realism, our team took a reductionist approach, creating a separate survey question to rate the realism of each discrete action performed in the course of a laparotomy, as presented in Figure 2. To capture data on the utility of the construct as a whole for its intended purpose of simulating laparotomy creation and laparotomy closure for surgical trainees, we included two questions at the end of the survey investigating whether the construct was suitable for teaching each of these as well. Using convenience sampling, ten attending surgeons (to mean fully trained, board-certified surgeons having completed all residency and fellowship training) from a broad array of specialties (see Table 1) at a large military hospital were recruited to evaluate the construct. For this preliminary evaluation of the realism of our construct and its suitability for simulation, we restricted our assessor pool to a group of ten attending surgeons who were recruited by the study team from a large military hospital in the United States. No ethical approval was needed as the study involved no human or animal subjects.

| Specialty | Years since completing residency | Approximate number of virgin midline laparotomies completed as an attending |
|---|---|---|
| General surgery | 2 | 0–20 |
| Colorectal surgery | 6 | 21–40 |
| Minimally invasive surgery | 7 | 61–80 |
| Trauma surgery | 9 | 100+ |
| Minimally invasive surgery | 11 | 100+ |
| Surgical oncology | 12 | 100+ |
| Minimally invasive surgery | 17 | 100+ |
| Trauma surgery | 21 | 100+ |
| General surgery | 28 | 100+ |
| General surgery | 42 | 100+ |

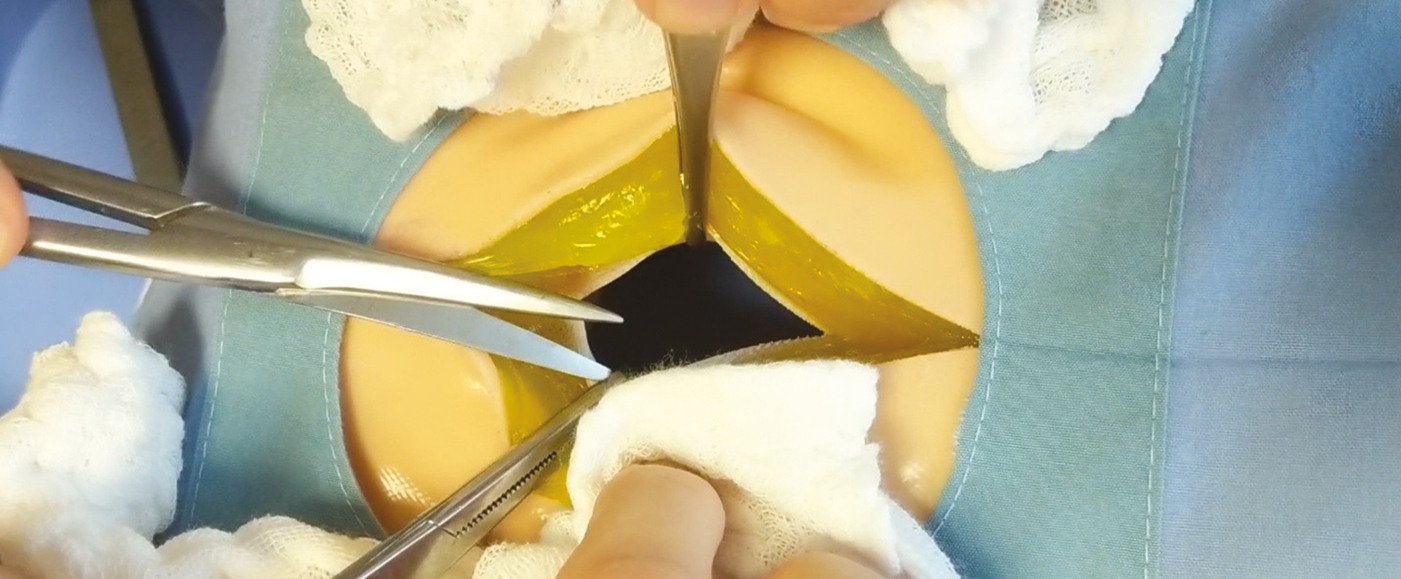
Fascia is opened during simulated laparotomy on an early prototype of the CLOS-IT
CLOS-ITs were provided to ten attending surgeons, who were asked to perform and close a standard midline laparotomy on the device (Figure 3), and then to rate it for realism and utility as a simulation tool afterwards. Among the attending group, seven had completed fellowships: three in minimally invasive surgery, two in trauma surgery and surgical critical care, one in colorectal surgery and one in surgical oncology. Raters were provided with one abdominal wall construct, one #10 blade, two army–navy retractors, two Kocher clamps, two Ferris-Smith forceps, one needle driver, two #1 PDS sutures, two #2-0 prolene sutures, two Adson forceps and one skin stapler. A general surgery resident served as a first assist.

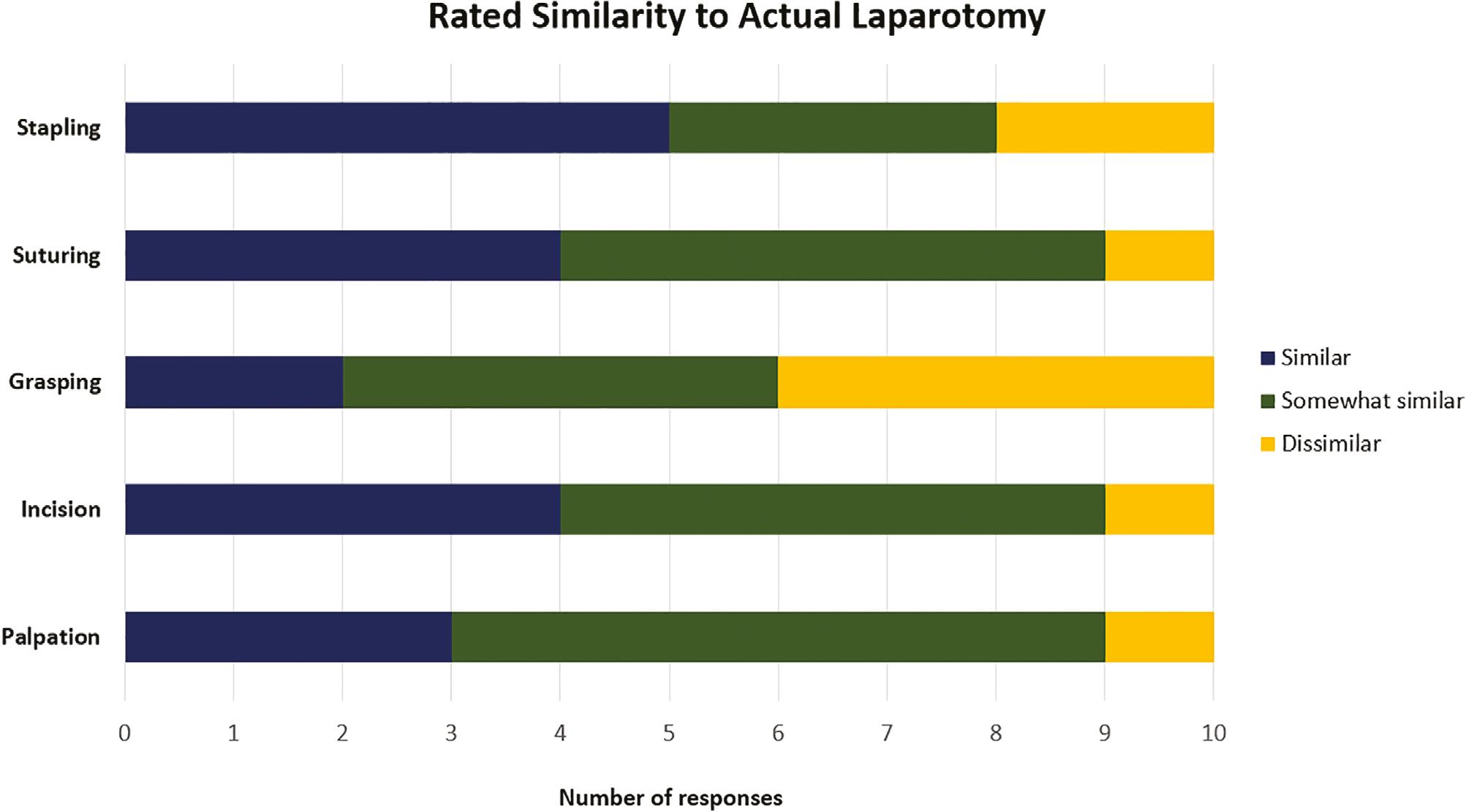
Surgeon impressions after completing a simulated laparotomy and closure on the CLOS-IT
Attending surgeons were informed they would be asked to compare the experience to an actual midline laparotomy after the exercise and were then directed to proceed with a 10 cm midline laparotomy, dissecting down to and incising fascia. They were instructed to close fascia using either 1 PDS or 2-0 prolene according to their preference and then to close the skin with staples. Attending surgeons were asked to complete an online survey regarding specialty choice, years of experience since completing residency, number of virgin midline laparotomies completed as an attending and a series of questions rating the realism of the model.
Survey questions addressed the model’s similarity to living tissue in response to the following actions: palpation, incision, grasping, suturing and stapling. In each of these domains, attending surgeons were asked to rate the model as dissimilar, somewhat similar or similar to human tissue. Lastly, raters were asked whether the construct was acceptable as a training device for simulating midline laparotomy and for simulating midline laparotomy closure.
The CLOS-IT was developed at a one-time cost of $125 for creation of the reusable mould and rectus abdominis frame, and an additional cost of $34.38 for the single-use surgical component. The string and standard hospital wash basins that were made into a reusable mounting surface for the manufactured abdominal wall layers are typically readily available, and are not included in this cost. Manufacture time consisted mostly of the required cure interval for each layer and was 21 hours per unit. Printing more than one frame allowed us to have multiple components curing in parallel within that same time.
Manufacture occurred over three phases: creation of fascia (20 minutes of composite assembly followed by 16 hours of cure time), creation of skin, adipose tissue and musculature with incorporation of fascia (30 minutes of composite assembly followed by 4 hours of cure time for muscle and skin, and 2 hours for adipose tissue), and assembly of components with a clear silicone adhesive (about 5 minutes). The full shelf life of the product is unknown, but one early prototype that was kept unused for more than 1 year appeared to retain its initial appearance and consistency.
On completing a survey after simulated laparotomy and closure, nine out of ten surgeons found the construct to be somewhat similar or similar to human tissues upon palpation, incision and suturing. Six out of ten surgeons found the construct to be somewhat similar or similar to human tissue upon grasping, and eight out of ten surgeons found the skin to be somewhat similar or similar to human skin upon stapling. Ten out of ten surgeons described the model as acceptable for simulating midline laparotomy, and nine out of ten described the model as acceptable for simulating midline laparotomy closure.
Multiple independently developed laparotomy simulators have been described recently, each designed with a different focus and oriented towards a specific set of teaching goals [17–19]. Brown et al. describe a novel model that makes use of porcine organs to produce a highly realistic result and allow for the simulation of a wide array of visceral injuries [17]. Exceptional realism is achieved by using real viscera in their simulator, but the abdominal wall of this model consists of a simple neoprene layer, and thus lacks any useful realism for practising proper fascial closure. Roche et al. describe a simulator that received favourable ratings for realism, but which lacks structural fidelity, like markers that might allow for identification of straying from the midline and a lack of fibrous dermal layer to allow for realistic manipulation and closure of skin [18]. Kukonnen et al. describe a model specifically designed to simulate intra-abdominal haemorrhage. Among this model’s strengths are the inclusion of great vessels and simulated blood pressurized by a pump to generate artificial bleeding [19]. However this model’s focus appears to be on generating realistic haemorrhage, and the described abdominal wall (a combination of leatherettes, rubber foam and food wrap) appears to be made more of convenience materials than of validated, biomechanically realistic constructs. The CLOS-IT fills these gaps, providing a simple yet realistic product that mimics both the anatomy and the biomechanical properties of the human abdominal wall.
At a per-unit cost of less than $35 (excluding the cost of the reusable base), the CLOS-IT is an exceptionally affordable simulator for basic laparotomy and abdominal closure. Besides the mounting surface, the construct itself is made up only of Powermesh, various commercially available silicone formulations and dyes for realism. While it is true that the printed 18 × 18 cm frame and crossbar used to mould the tissue layers is more expensive at a material cost of about $125, these components are indefinitely reusable and represent a one-time cost for production of the device. While many institutions will not have the benefit of access to in-house state-of-the-art three-dimensional (3D) printing, these services have become ubiquitous and make it possible to order 3D-printed objects without the admittedly significant expense of purchasing a 3D printer [20–22].
From a standpoint of realism, the CLOS-IT scored reasonably well, particularly in the domains of similarity on palpation, incision and suturing, and more importantly was broadly considered to be an acceptable construct for simulating laparotomy and closure by the attending surgeons in our study. The biggest opportunity for improvement was in the realm of grasping fidelity, where four out of ten attending surgeons found the model to be dissimilar to human tissue. Going forward, the model could be adjusted for improved realism by experimenting with different silicone formulations and additives to better approximate the experience of interacting with real tissue.
From an educational perspective, the CLOS-IT offers a trainer in which learners can hone the fundamentals of abdominal entry and closure. One unique benefit to this simple simulator is the ability to simply invert it after each exercise and to directly visualize the completed suture line from the underside. Stitch placement, bite size and bite spacing can all be easily evaluated following simulation, and this feature presents a useful opportunity for educators to provide feedback that is both targeted and objective.
Our study represents just the first step in the evaluation of this construct as a teaching tool. The sample size is small, at only ten attending surgeons, and offers no insight into trainee perspectives on the device, since we only subjected the construct to assessment by experienced surgeons. Similarly, the data presented here were obtained at the same institution where the model was developed, raising the potential for bias in attending surgeon feedback. Future directions for CLOS-IT could include further refinement for realism and testing among larger groups of surgeons that include trainees as well as surgical staff at other institutions and even comparing performance between learners who have undergone laparotomy training using different simulation tools. Additionally, evaluating the benefits of the construct as a teaching and even as an assessment tool could be the subject of future studies.
The CLOS-IT is a realistic, low-cost simulator for laparotomy creation and closure. It can be manufactured with commercially available materials, offers acceptable realism for its purpose and is at a price point that is not prohibitive. Future directions could include testing the device as a teaching and assessment tool, and further refining it for improved realism.
VM contributed to construct development, testing and writing. CD contributed to construct development and testing. SK contributed to construct development. PL contributed to mould and frame development and production. JS contributed to construct development and study design. EMR contributed to study design. BF contributed to construct development and testing. WBS contributed to study design, construct development, testing and critical review.
This work was supported by The Geneva Foundation (Transforming Technology for the Warfighters TTW HU00011820013).
None declared.
None declared.
None declared.
Supplementary data are available online at the Journal of Healthcare Simulation (Supplementary Appendix S1).
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.