
Jabeen Fayyaz 1, 2
ORCID:https://orcid.org/0000-0002-2560-9926
, Asit Misra 3ORCID:https://orcid.org/0000-0002-9682-5116
[1]
[2]
[3]
faculty development (simulation educator or simulation technician),innovation,patient safety,simulation,and translational simulation
Article Type: editorial
Simulation-based education (SBE) continues to evolve beyond its traditional role of technical skills training. SBE is now increasingly used in shaping systems readiness, faculty development and as a tool for teaching socially responsible practice. The contributions within this short report on Simulation Innovations Supplement reflect this evolution clearly. While varied in subject matter and environment, all of the articles presented share a common theme of innovation in response to a need or gap, evaluation and a response to real-world constraints.
A recurring theme across the supplement is innovation driven by necessity. Vidgen et al. discuss the development of an economical cervical model for cold knife cone biopsy simulation training, in response to a reduced exposure of trainees to this high-risk procedure [1]. Similarly, Bindler et al. present an innovative large-group approach to interprofessional simulated participant encounters, demonstrating the efficiency and sustainability [2]. Together, these contributions challenge the assumption that high-quality simulations are resource-intensive and highlight the creativity and thinking outside the box in settings which are under-resourced.
Beyond individual learning, several articles underscore the expanding role of simulation in organizational readiness and patient safety. Boyle et al. describe an educational and translational approach to simulation that aims to prepare psychiatric clinicians for acute patient deterioration during the launch of a new mental health facility [3]. Their work illustrates how simulation can simultaneously build clinician confidence and uncover latent safety threats within systems and processes, reinforcing simulation’s role as a tool for organizational change and system resilience [4].
Faculty development and reflective practice emerge as another central theme in this SRSIS. Havens et al. describe a faculty development initiative that creates safe and brave spaces for simulation educators to discuss mistakes and unintended consequences in facilitation, fostering open and brave conversation in a psychologically safe manner [5]. In a related contribution, Merriman et al. detail the evolution of a Meta-Debrief Club designed to support novice debriefers through collaborative learning rather than formal assessment highlighting the role of peer coaching [6]. By simplifying structure and emphasizing peer discussion, this model broadens access to faculty development and strengthens the creation of a community of practice. Together, these articles emphasize that sustaining high-quality simulation requires a thoughtful consideration of faculty development pathways in simulation. Wood et al. also describe an idea for an interactive workshop aimed at empowering educators to embed sustainability within simulation practice [7]. By integrating carbon costing, reflective dialogue and actionable pledges, their work moves beyond awareness to practical change. This contribution is particularly timely, positioning simulation as both a contributor to and a potential mitigator of healthcare’s environmental impact, and encouraging educators to consider sustainability as a core design principle.
Across all submissions, there is a consistent emphasis on evaluation and continuous improvement. While most studies rely on Kirkpatrick’s Level 1 and 2 that is participant perceptions rather than objective performance or clinical outcomes, authors are transparent about limitations and explicit about future directions. The inclusion of ‘What’s next?’ sections across the articles reinforces simulation as an iterative practice that evolves through cycles of design, implementation, reflection and refinement, similar to PDSA cycles that could be adapted for simulation-based quality improvement cycles, where they are called instead of ‘Plan, Do, Study, Act’ (PDSA), as ‘Pan, Do, Simulate, Act’ (PDSA).
Taken together, the articles in this SRSIS portray a field that is increasingly responsive, reflective and responsible. These innovations do not force novelty for its own sake. Instead, they emerge from genuine educational gaps, system vulnerabilities, faculty needs and societal challenges. They demonstrate that impactful simulation is defined less by technology or scale and more by intentional design, alignment with learner and organizational needs and a willingness to adapt.
As SBE continues to expand globally, the insights from this SRSIS are both timely and transformative. Educators and leaders are encouraged to think creatively within the limited resources, with more focus on evaluation and offer support to their faculty. This way, simulation will become a vector for change at the broader level, with impact on the quality of care and patient safety. The work presented here advances not only simulation practice but also the values that drive it, offering a clear and hopeful direction for the future of healthcare simulation.
None declared.
None declared.
None declared.
None declared.
None declared.
1.
2.
3.
4.
5.
6.
7.
Sue Vidgen 1, Michael Blunt 1, Katherine Phillips 2, Sarah Janssens 2, 3, Gillian Gallagher 1
[1]
[2]
[3]
Cold knife cone (CKC) biopsy is the historically recommended surgical technique in suspected cases of cervical glandular disease and invasion [1] to avoid specimen artefact, difficulty interpreting margin involvement and risk of specimen fragmentation associated with loop electrosurgical excision procedures [2]. In a procedure associated with risk of short- and long-term complications [1], small-volume surgical case exposure [3] can result in a recommendation for referral to an experienced gynaecologist or gynaecology oncologist for management of this disease [2]. To contextualize this to our organization’s needs, an audit at the Mater Hospital Brisbane, revealed 12 cases performed over the 2024 surgical training year (equating to one procedure exposure per trainee).
Gynaecology trainees face barriers to developing skill mastery, due to limited exposure to gynaecology procedures, with evidence supporting simulation-based learning to supplement this deficit [4]. The Cervical CKC Biopsy Model was designed to facilitate simulation-based learning in the surgical technique required for cervical conization. This report details the development and refinement of the model, enabling other simulation facilities to replicate this affordable training model, for wider adoption into gynaecology training programmes.
Building on the success of an earlier low-fidelity LLETZ surgical simulator [4], the collaborative team of simulation coordinators, educators and specialist surgeons adapted and refined this model to facilitate CKC surgical techniques and skill acquisition. The goals were to create a model that not only portrayed physical and anatomical resemblance (structural fidelity), but more importantly, provided tactile, clinical accuracy and functional properties to support the application and transfer of theory into practice (functional task alignment) [5]. It allowed participants to perform CKC, including modified Sturmdorf suture with the model located at the end of a simulated vagina, thus providing fidelity in the surgical difficulties of the procedure (Figure 1).

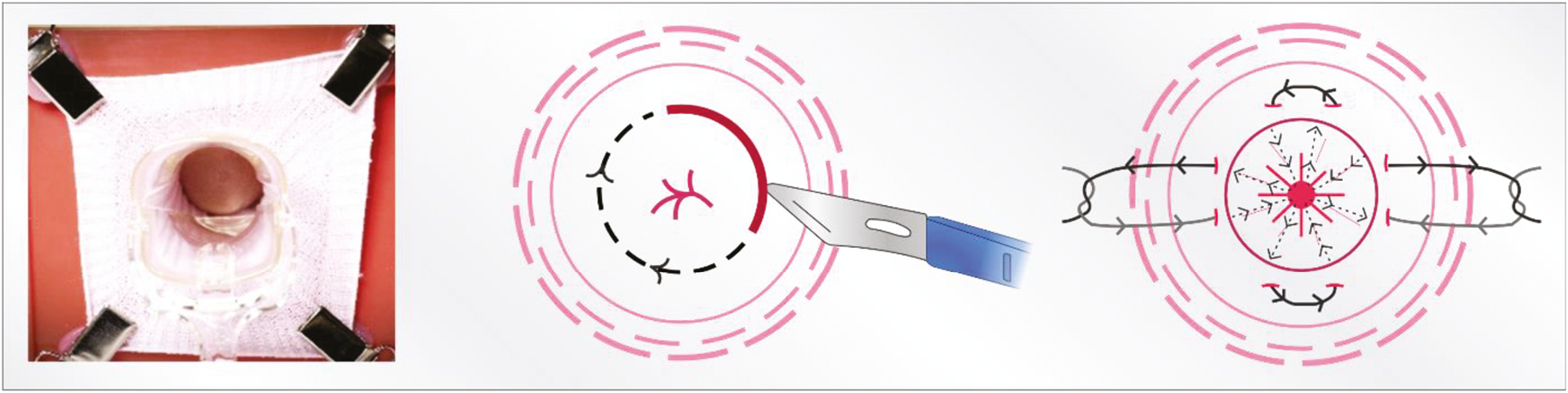
Silicone cervix model within simulated ‘sock’ vagina (left). Diagram of a CKC (middle) and a modified Sturmdorf suture (right)
A high priority was the usability and efficiency of resetting a new cervix model into the simulator after completion of each surgical attempt, allowing for multiple repetitions of deliberate practice, and rapid turnover between each learner, while limiting financial outlay associated with the single use per cervix model. We utilized readily available items from clinical areas, hardware, grocery and haberdashery stores for the creation of the body of the simulator, representing the pelvis housing the cervix model. See Figure 2.


Silicone cervix model (left). Lamson box forming the body of the simulator representing the pelvis (middle). Front view of the simulator displaying the ‘sock’ vagina and ‘foam’ uterus, firmly housing the cervix model ready for CKC biopsy (right)
The materials for the construction of the cervix model were purchased from wholesalers. The silicone, sets and cures at room temperature, is soft, strong and elastic, making it ideal for excision and suturing. At time of writing, the initial financial outlay for materials was approximately AUD 650. Estimated cost per model was AUD 13. For a complete list of materials, step-by-step construction guide and video demonstration, click on this link (CKC biopsy construction guide).
The cervical model was developed within a larger simulation-based Vaginal Surgical Skills workshop customized by the Mater Health/Simulation team, held annually for 2 years, with a cumulative total of 17 participants. The workshop is targeted at Royal Australian and New Zealand College of Obstetrics and Gynaecology (RANZCOG) trainees, providing participants the opportunity to perform simulated vaginal surgery to increase skill level and procedure exposure with supervision of experienced gynaecologists. After completion of this course, participants evaluated the course inclusive of the simulation-based models utilized throughout it.
All participant evaluation questionnaire responses were positive regarding the overall simulation-based workshop, with 88% of participants ‘strongly agreeing’ that the cervical CKC biopsy model was appropriate to their learning needs. One participant specifically reported they found value in the model and when asked ‘what are two things you found valuable about this session?’, they responded with:
Tips and tricks for practicing cone knife (cone). I really like the small group size and practical focus to allow one on one teaching.
Other feedback included finding value in the practical session to consolidate skills, particularly around the use of the simulation models, with one participant commenting:
Simulation models are great.
Further research could include independent assessment of crucial procedural steps to demonstrate functional task alignment with CKC biopsy, in addition to specific participant evaluation of the utilization of this simulator in terms of fidelity and acceptability [4]. Including this data into future participant evaluations may be useful to assess the impact of this model as a surgical training tool.
Additionally, we see potential for adoption of the same anchoring device and quick exchange ability of this model to other ‘down the hole’ type simulators such as used for colorectal procedures. We welcome other facilities to utilize our construction guide to replicate or adapt to help meet needs within their organization.
We would like to thank Paul Ferguson for his contribution and co-creation of the supplementary images and production of the step-by-step demonstration video.
All authors contributed, reviewed and approved the final version of the report. SV: report concept design and lead author; MB: application, design and testing of the cervix model; Co-authored with SV, the construction guide and co-created the video demonstration included as supplements in the report; KP: Application, design, testing and evaluating model effectiveness; co-author and reviewer; Co-created and refined model; SJ: concept application, design and evaluation; senior reviewer; GG: Senior author and reviewer; collection and analysis of evaluation data; evaluating model effectiveness.
None declared.
None declared.
None declared.
None declared.
1.
2.
3.
4.
5.
Ross J. Bindler 1, Connie M. Remsberg 2, Rie Kobayashi 3, Skye McKennon 2, Dawn E. DeWitt 2, Marian Wilson 1
[1]
[2]
[3]
Interprofessional education (IPE) simulation activities involving team-based simulated participant (SP) encounters are increasingly important in health professions education [1]. Despite the benefits, institutions often encounter challenges with recruiting, training and funding the large number of SPs needed for IPE events involving hundreds of health professions students from multiple programmes and institutions [2].
In 2019, we developed a case-based IPE simulation where interprofessional teams of students interact with individual SPs using virtual breakout groups within a videoconferencing platform [3]. This resource-intensive IPE activity, made possible by external funding, trains hundreds of students from multiple universities across five sessions per year with 100+ students and 20+ SPs engaged per session. Students conduct a team interview with a SP to create a holistic treatment plan for an adult prescribed opioids after a back injury. When our team added a longitudinal patient follow-up encounter activity, we sought creative solutions to provide students with a valuable SP experience while balancing resources and expenses. The purpose of this evaluation was to determine whether student perception of quality and learning support were equivalent after reducing resource costs by engaging only one SP per IPE session.
We developed a 2-hour, high-fidelity follow-up IPE simulation for health professions students utilizing the same videoconferencing platform as used with the original activity [4]. Instead of one SP per breakout group, the follow-up activity couples one SP per session with a pre-recorded video of an experienced physician demonstrating a challenging conversation with an adult patient about escalating substance use following a back injury. During the synchronous IPE event, interprofessional teams (five to seven students per breakout group) review the written patient case and identify pertinent questions for the SP to ascertain appropriate next steps for a potential substance use disorder. Students return to the large group (approximately 100 students) to view the patient–physician video and ask follow-up questions of the single SP attending the virtual session. To streamline the question-and-answer portion, a faculty facilitator reviews student questions submitted via the ‘chat’ feature and either directs the questions to the SP or calls on students who verbally ask their question. After the live SP interview, conducted remotely using videoconferencing technology, students return to their breakout groups to create a collaborative holistic treatment plan. Faculty members are assigned to cover three to four breakout groups each to check on student progress and answer questions.
During the final minutes of both IPE activities, students are provided with a link to a voluntary, anonymous post-session survey hosted by the primary university. Students are asked to rate the overall quality of the IPE simulation activity using a Likert scale (1: Very Poor; 2: Poor; 3: Fair; 4: Good; 5: Excellent). On the post-session survey for the follow-up activity, they are also asked to rate their level of agreement with the statement, ‘The live SP interview during the large group session helped support my learning’ using a Likert scale (1: Strongly Disagree; 2: Disagree; 3: Agree; 4: Strongly Agree). Finally, students are invited to provide free-text feedback on what they found valuable and what could be improved.
Post-session survey results from the follow-up activity (completion rate: 80.3%; 245 surveys/305 student attendees) were compared to post-session results for the original IPE activity where teams interacted with individual SPs (completion rate: 59.1%; 305 surveys/516 student attendees). Results indicated students perceived both activities as valuable despite differing models for SP interaction. Students rated the overall quality of the learning activities similarly with 86.2% responding ‘excellent’ (n = 106) or ‘good’ (n = 157) for the original (multiple SP) activity and 86.9% responding ‘excellent’ (n = 86) or ‘good’ (n = 127) for the follow-up (single SP) activity. No statistical difference in mean overall quality scores was found between the two activities: original activity mean = 4.2 (SD = 0.69); follow-up activity mean = 4.18 (SD = 0.76); p = 0.79. Most learners (92.2%) completing the follow-up IPE activity post-session survey ‘strongly agreed’ (n = 85) or ‘agreed’ (n = 141) that ‘The live SP interview during the large group session helped support my learning’. Open-text feedback highlighted appreciation of the patient–physician video for modelling challenging conversations. Respondents valued listening to the questions asked to the live SP by the facilitator and other students. Students reported feeling more prepared and less distressed with the large group single SP interview used in the follow-up IPE activity than during the small group live interviews with multiple SPs.
This proof-of-concept evaluation suggests interprofessional students view the single SP methodology and large group interview simulation format to be of similar quality as the more resource-intensive approach with multiple SPs and small group interviews. Based on student feedback, further evaluation to confirm learning outcomes utilizing large group interview methods with an individual SP is warranted, particularly for under-resourced communities. At a rate of $25 per hour for SP services, we estimated saving approximately $1000 per session with the single SP encounter. Future work can explore cost/benefit analyses in greater detail. Both small and large group SP encounters appear to meet distinct IPE simulation learning needs. Of note, if patient–clinician communication skills are a primary learning outcome, large groups may not be an appropriate option. Because this was not a randomized experimental trial and identical student groups were not recruited for comparisons, limitations such as selection bias and confounding variables must be noted and controlled in future work.
All authors significantly contributed to innovation conceptualization, design and execution of the project, and data collection, analysis, and interpretation of results as well as manuscript preparation.
Support for this project was provided from grant 1H79FG000075-01 funded by the Substance Abuse and Mental Health Administration (SAMHSA). The contents of this report are solely the responsibility of the authors and do not necessarily represent the official views of, nor an endorsement, by SAMHSA, the U.S. Government, or Washington State University.
The data used in this report can be made available upon reasonable request to the corresponding author. All educational materials referenced can be accessed on the authors’ webpage: https://opioideducation.wsu.edu.
All data collected was anonymous and for quality assurance purposes. After the decision for publication, an application was submitted to the Washington State University Institutional Review Board and the project was deemed non-human subjects’ research.
None declared.
1.
2.
3.
4.
Laura Havens, Catherine Paton, Catriona Neil
There is evidence that learning from mistakes in clinical practice can be a powerful force for change [1]. Simulation-based educators support participants to develop their clinical practice through reflecting on mistakes within a facilitated debrief [2]. Following on from a Society for Simulation in Europe (SESAM) 2023 workshop, we felt there was an opportunity for faculty to explore and learn from their own and others’ mistakes made whilst facilitating simulation-based education [3]. Further exploration of mistakes can provide an opportunity for learning and development for all faculty. Therefore, we felt there was value in creating a protected space for peer discussion and support in the time-limited world of simulation-based education delivery.
Here we describe a pilot educational intervention, using group discussion, to open conversations about mistakes that occur during simulation.
We aimed to establish:
•If group discussion represents a useful learning environment for this;
•If faculty development on this topic increases openness to discussing mistakes;
•If discussion of mistakes leads to changes in simulation faculty practice.
We organised 3 × 1-hour sessions of between five and six attendees, inviting simulation-based educators of differing professional backgrounds and levels of experience to a small group discussion. We acknowledged that psychological safety would be vital to allow participants’ full engagement in discussion of their own and others’ experiences, and so we considered measures to maximize this. The session introduction outlined our aims and provided ground rules which attendees were invited to add to. The need for confidentiality and details of group discussion to remain within the session was highlighted. Prior to each session, a member of the group volunteered to prepare and share a personal experience of a mistake or unintended consequence whilst facilitating simulation. Discussion was then opened to the group, allowing a free-flowing sharing of different perspectives and experiences with the support of two facilitators. The individual sharing their experience in the pilot and further sessions was a senior member of faculty. This was felt to help flatten the hierarchy within the session. Following the first group, we also focused on maximising environmental factors such as circular seating arrangements to support open discussion and engagement [4].
Anonymized written feedback was collected directly before and after each session. We reviewed published work [5] measuring change in attitude towards mistakes to help guide the design of feedback. Statements to measure change in attitude were rated on a six-point Likert scale from ‘strongly disagree’ to ‘strongly agree’, including ‘not applicable’. Several white space questions were also included to provide qualitative data. Attendees were asked to describe any specific planned changes to their practice following the discussion. Finally, we asked attendees for any suggestions for improving the session, having made it clear from the outset that the sessions were in development.
All 16 attendees completed feedback and reported benefit from the session. This included increased awareness that all facilitators face mistakes and unintended consequences, whatever their level of experience. Ratings of whether learning occurred after hearing others’ mistakes showed the largest increase (Figure 1). Half of the respondents showed a one-point increase, mostly from agree to strongly agree, one had a two-point increase, and all others remained at agree or strongly agree. There was an increase in agreement that learning occurs following one’s own mistake, with 4 one-point increases, one reduction from agree to neither agree nor disagree, and 11 remaining on strongly agree before and after the group.

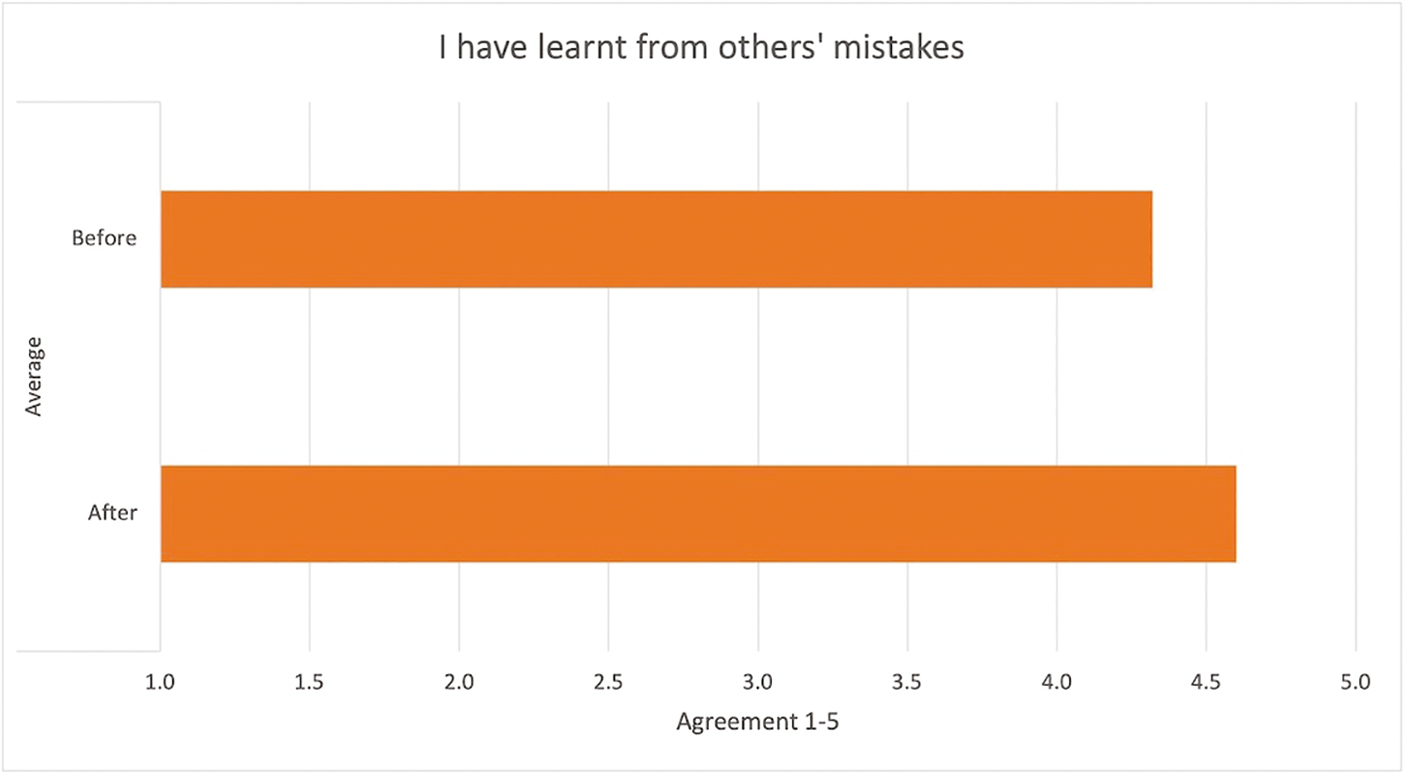
Average agreement with the statement ‘I have learnt from others’ mistakes’.
Half of participants felt more comfortable discussing mistakes following the session (Figure 2). Four respondents had no change, and four had a one-point increase, with three increasing to strongly agree. Qualitative feedback highlighted the value of a designated space for this discussion, alongside its contribution to faculty development – ‘really rich and valuable’ and ‘space to explore own experiences as well as hear from others and learn’.

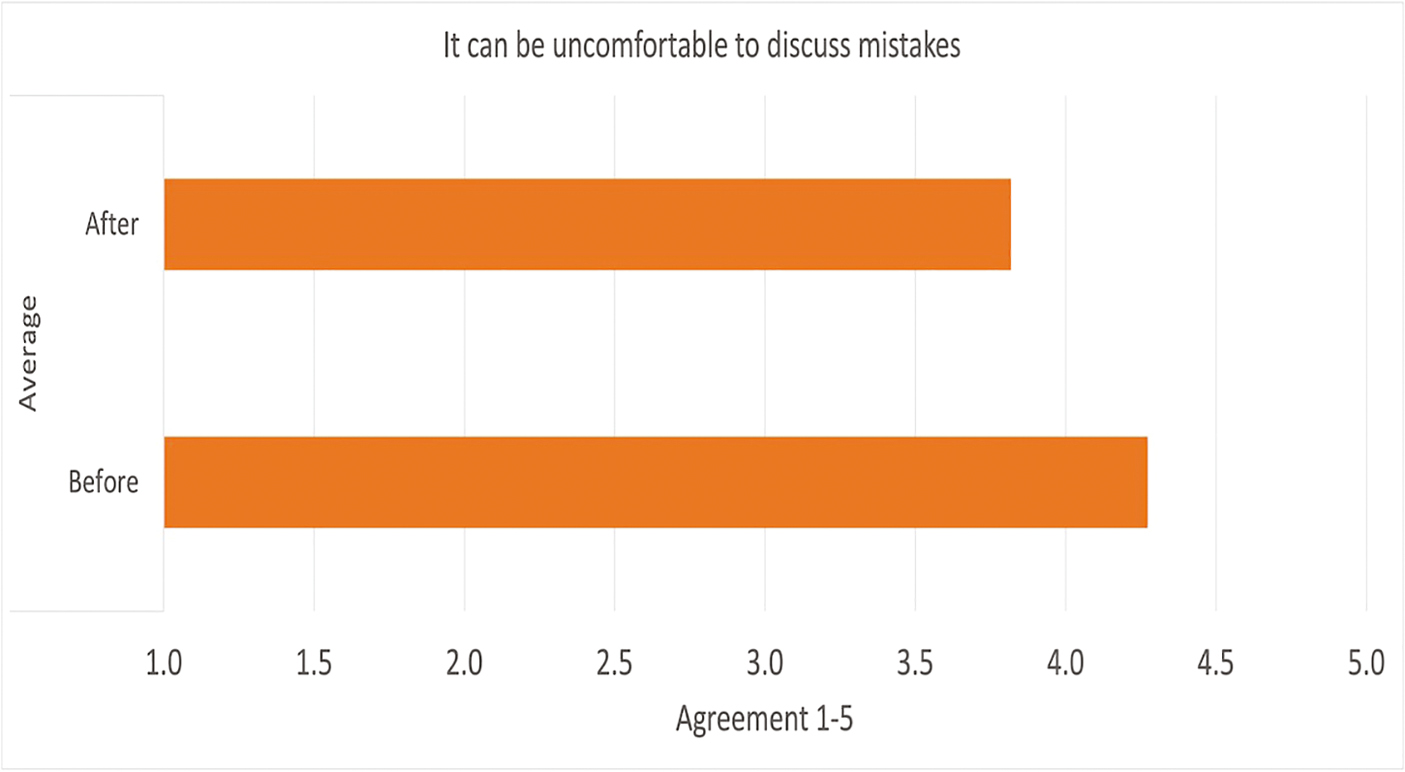
Average agreement with the statement ‘It can be uncomfortable to discuss mistakes’.
Attendees identified a range of planned changes to their simulation facilitation practice post-session, the intention to debrief more often with peers and identifying a need for greater reflection on approaches to managing unintended consequences. Others identified changes based on ideas shared within group discussion, including approaches to working with new faculty colleagues and techniques to maintain psychological safety.
We plan to establish this group discussion session as a regular element of local faculty development, aiming to share learning and create a culture of open discussion of mistakes without stigma. If this pilot was developed into a research project, this would allow ongoing evaluation of actual change to practice at designated intervals. Ongoing data collection, more directly measuring individuals’ openness to discussion of mistakes, could further support our third aim. We feel this session and its aims could benefit other workplaces, both clinical and non-clinical. The development of an online version of the session should be considered, allowing wider access and use in larger organisations.
With acknowledgement and thanks to Kirsty Freeman, James Tiernan, Bec Szabo and Susan Eller who ran the workshop ‘Don’t waste a good mistake, learn from it’ SESAM 2023, who inspired this work. The authors would like to thank all the staff in Medical Education in NHS Lanarkshire for their support throughout the project.
All authors were involved in the initial faculty development sessions, as well as the writing and review of the submitted report.
None declared.
The data that support the outcomes of this report are available from the corresponding author, LH, upon reasonable request.
No ethics approval was deemed necessary for this work.
The authors declare no conflict of interest.
1.
2.
3.
4.
5.
Vidya Samuel 1, Thomas Hogan 1, Jonathan Hurst 2, Jennifer Peterson 1, 3
ORCID:https://orcid.org/0000-0002-7248-2016
[1]
[2]
[3]
neonates,medical education,end-of-life care, bereavement,and simulation
Providing end-of-life care to infants and their families is an intensely emotive and nuanced area, which requires skilful, individualized communication and knowledge [1]. Neonatal healthcare professionals require psychologically safe education spaces to develop their skills in providing this type of care [2]. Simulation can provide hands-on, experiential learning; however, there is limited research around utilizing simulation for neonatal end-of-life care training [2,3].
Our neonatal unit has a pre-existing regular simulation programme running 2-hour multidisciplinary scenarios twice per week. Two end-of-life care simulation scenarios were developed and incorporated into this regular simulation programme (Figure 1). The sessions were facilitated by the neonatal simulation fellow and the bereavement team.

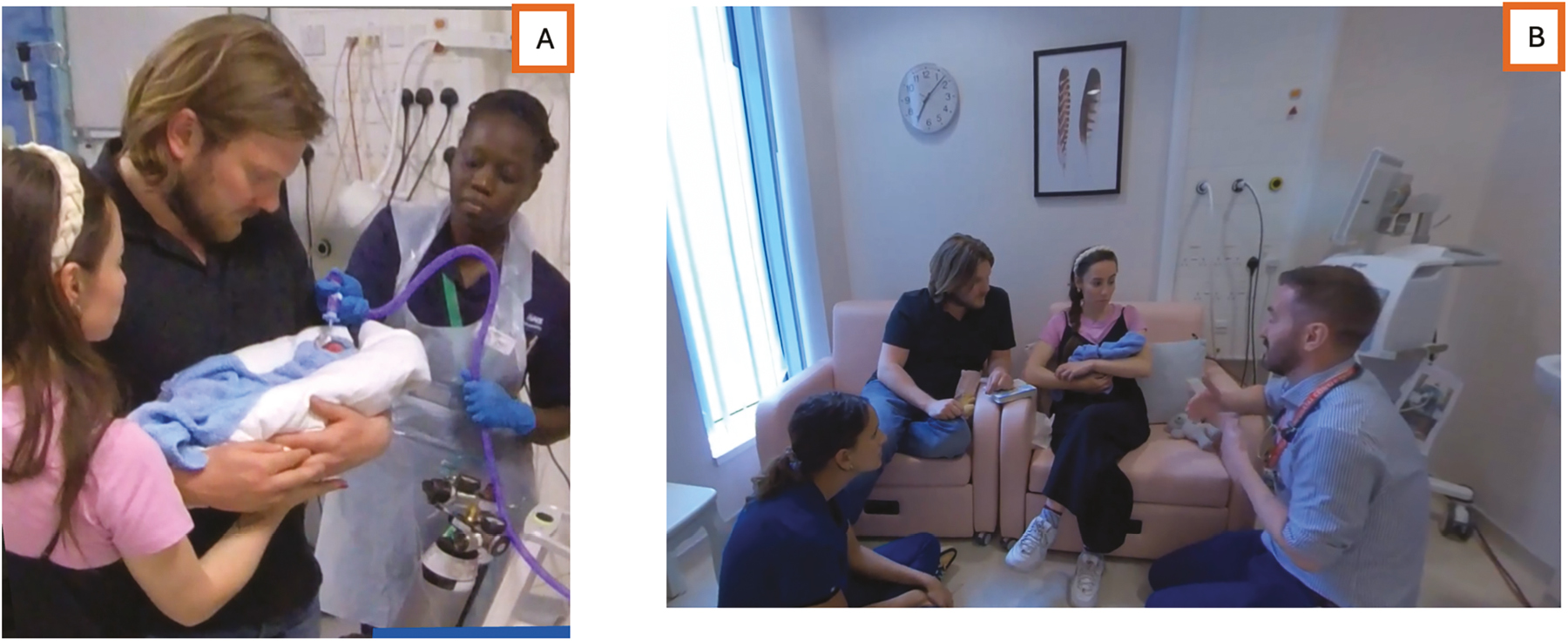
Photos from the end-of-life care simulation scenarios. One simulation (A) focused on transferring a baby from the neonatal unit to a parent room for compassionate extubation. The other scenario (B) focused on the compassionate extubation itself. Participants received an email prior to the session informing them that the simulation would focus on end-of-life care and including links to the relevant unit guidelines, along with information about emotional support available
Following the simulation session, all participants were asked to complete a paper-based feedback form. These feedback forms were completed live at the end of each session. The forms were collated and transcribed into Microsoft Excel for analysis. For quantitative data, a relative percentage was calculated as a proportion of total respondents. The qualitative data was analysed using a six-step reflexive thematic analysis approach [4].
Between November 2018 and January 2020, 26 simulations involving 78 neonatal professionals were undertaken with 53 completed feedback forms. Respondents included 23 neonatal nurses, 23 resident doctors, 4 neonatal nurse practitioners, a student nurse (observer) and two respondents who did not specify their professional role.
All respondents reported that participating in these end-of-life simulations was a worthwhile educational experience, and the majority (89%) reported their knowledge about end-of-life care had increased.
Three themes were identified from the data about which elements of learning participants had found most useful: (i) managing practicalities, (ii) managing communication and (iii) managing emotional responses as a professional (Table 1).

| Managing practicalities | Managing communication | Managing emotional responses as a professional |
|---|---|---|
| ‘Very useful to practice the practical aspects of a difficult, infrequent situation but very important to get it right.’ | ‘[don’t want to] say something that would affect them [parents] badly forever’ | ‘This simulation has helped in understanding how to deal in such a situation which is stressful, tearful and with mixed emotions.’ |
| ‘About managing lines, drugs and how to transport to Snowdrop [bereavement suite]’ | ‘[I] know how to phrase things’ | ‘Very emotional scenario’ |
| ‘What we can and can’t stop/remove eg drugs, lines etc’ | ‘… understand what people’s roles were’ | ‘I found it [the simulation] extremely useful as you often practice simulations that are quite clinical and focussed on interventions. This simulation taught me when to step back clinically and do more to make family and baby comfortable’ |
| ‘[Aware of] what options are available to give to parents …. ie offering for mother to carry baby in her arms [to the bereavement suite]’ | ‘… a clear plan between the team’ | ‘Very emotional simulation. It has helped me understand my role in what happens following a baby’s death.’ |
| ‘[I’m now] aware of options available’ | ‘Useful to practice communication with parents and medical team and terminology to use’ | ‘… understanding the condition and emotional questions of parents and then comfort in dealing with the situation’ |
| ‘[Aware of] the logistics of moving a baby, what to disconnect etc’ | ‘[Understand] … specific role of doctor in the extubation and what things need to be discussed eg what to expect after extubation …’ | ‘I previously felt scared of caring for a baby following death.’ |
| ‘Greater knowledge of options available as memory making etc’ | ‘Better understanding of what is involved in preparing parents and of what is involved after death’ | ‘less scared of being involved in transfer to [bereavement suite]’ |
Very useful to practice the practical aspects of a difficult, infrequent situation but very important to get it right [participant feedback].
Participants reported that the simulations increased their knowledge of the practical and legal processes involved with end-of-life care. These simulations allowed participants the opportunity to learn about national legal processes, including how to certify death in a neonate and coronial reporting, alongside the specifics of end-of-life options available at their local unit, such as the layout and facilities of the bereavement suite, local bereavement documentation and mortuary processes. The simulation also allowed professionals to interact with memory-making items such as hand and footprint kits and the locally available books and activity packs for supporting siblings. Additionally, participants had concerns around the legality of removing tubes and lines pre- and post-death and managing medications used for symptom management. These simulations prompted participants to explore their own knowledge on these topics and the facilitated debriefs ensured participants were able to have their questions clarified.
Useful to practice communication with parents and medical team and terminology to use [participant feedback].
Prior to the simulation, participants expressed concern about communicating with parents in end-of-life care scenarios; ‘[don’t want to] say something that would affect them [parents] badly forever’. The simulation provided a space to practise discussing difficult end-of-life topics with simulated parents. Subsequently, participants reported increased confidence with how to communicate; ‘[I] know how to phrase things’.
Additionally, several respondents appreciated being able to practise their interprofessional communication. Coordination of care and team communication is crucial to smooth and effective end-of-life care. The simulation helped participants ‘understand what people’s roles were’ and the importance of having ‘a clear plan between the team’ which aids professionals in developing a cohesive, individualized end-of-life care plan with the parents.
This simulation has helped in understanding how to deal in such a situation which is stressful, tearful and with mixed emotions [participant feedback].
Despite the sessions being a simulated environment, many respondents described participating in the simulation as emotive and engaging; ‘very emotional scenario’. They valued the opportunity to reflect on how best to provide this care and found the simulation useful for preparing them for the range of emotions experienced by professionals providing such care.
Respondents described difficulty when facing situations where medicine cannot cure or manage their patient’s condition and the professional powerlessness that this can confer (‘knowing that we couldn’t do anything’). However, the simulated scenarios allowed them to reflect on how to cope with their own emotions and how support can be provided to families: ‘This simulation taught me when to step back clinically and do more to make family and baby comfortable’.
This study utilized a written survey format to gather data from participants. Survey data may lack the depth that other qualitative formats can provide, such as interviews with participants. However, the survey format allowed data to be gathered from a large number of participants in a shorter timeframe at the end of each simulation [5].
End-of-life care simulation is a useful training modality for neonatal professionals. As identified by the respondents, there is scope to expand scenarios to cover a wider range of end-of-life care situations and to incorporate other palliative care principles.
The actors and participants featured in the figures have consented to their images being used for teaching and publication in relation to these simulations.
JP and JH devised and designed the project. Data collection and coordination were performed by JP. Data analysis was performed by VS and JP. The initial manuscript was written by VS and JP. TH and JH edited the manuscript. All authors reviewed the manuscript prior to submission.
No funding received.
None available beyond that presented in the article.
Not required.
Nil to declare.
1.
2.
3.
4.
5.
Sujatha Sharada 1
ORCID:https://orcid.org/0000-0002-1965-9038
[1]
anterior nasal pack trainer,Competency-Based Medical Education,emergency medicine,health professions education,medical education,modelling,Peyton’s four-step method,and task trainers or part-task trainers
The competency-based medical curriculum in India emphasizes skill acquisition, focusing on outcomes and competencies. Competency-Based Medical Education (CBME) prioritizes outcome-oriented learning, necessitating repeated practice of skills under supervision to achieve proficiency [1]. Anterior nasal packing, a certifiable procedural skill in Otorhinolaryngology (as outlined in the Graduate Medical Education Regulations 2019), is a critical competency for managing epistaxis, a common ENT emergency. However, inadequate training in this area compromises patient safety.
Traditional simulation-based training methods are effective, but existing nasal packing simulators are often prohibitively expensive and lack realism [2]. There is a clear need for a highly realistic, human-like nasal packing trainer that provides a cost-effective and accessible solution for medical trainees. This innovation aims to address this gap by introducing a novel anterior nasal packing trainer, designed to enhance skill acquisition and improve patient outcomes.
We aimed to design and construct a cost-effective anterior nasal packing simulator for practising packing of the nose with ribbon gauze in the treatment of epistaxis. Initial consultations were held with a group of Otorhinolaryngology faculty members. Institutional Ethics Committee scrutinized the project’s methodology, the necessity of using cadaver and the measures in place to handle the remains respectfully.
To ensure anatomical accuracy, a mid-sagittal section of a cadaveric head was used to create impressions of the nasal cavity and face. An exact replica of these impressions was crafted from clay, which served as the master model.
A moulding process was employed using silicone, followed by the creation of a mother mould from fibreglass. The work mould was then separated from the mother mould, and casting was performed using silicone and fibreglass. To enhance realism, the model was coloured to match the natural appearance of the nasal cavity.
The medial half of the model was sealed with transparent acrylic glass, allowing for visibility and replaceability. This design feature enables users to monitor packing placement in real-time. The simulator was mounted on a rotatable stand, permitting 360-degree rotation (Figures 1 and 2).


The image shows ANTPACK simulation model used for anterior nasal packing training


Learner performing anterior nasal packing on the ANTPACK simulation model. The figure demonstrates the insertion and placement of ribbon gauze within the anatomically detailed nasal cavity of the task trainer
A comprehensive evaluation of the anterior nasal packing trainer was conducted, involving four batches (Third Professional Phase 1 MBBS) of 20 students each (n = 80). All of them were coming for the first time to this department for learning, showing that they have no prior knowledge or skills in management of epistaxis. Small group discussion was conducted for each batch on causes of epistaxis, investigations and management protocols. After that, a lecture class of 10 minutes duration was taken on the methods of anterior nasal packing. Each student was trained in anterior nasal packing by ‘Peyton’s four-step method’ of teaching anterior nasal packing in the given model. Formative assessment was undertaken using Objective Structured Clinical Examination (OSCE) as an observation station using an in-house validated checklist, 14 days after this training class. Additionally, feedback was solicited from learners to gauge the effectiveness of the trainer using a validated Likert scale questionnaire. The responses are given in Table 1, which shows students’ perceptions of the anterior nasal packing task trainer across six learning domains. Overall, majority of students agreed or strongly agreed that the task trainer was effective in learning nasal packing, promoted active engagement, improved their skills and enhanced retention of the procedure skill. A smaller proportion reported neutral responses, while no one expressed disagreement or strong disagreement. Confidence and satisfaction also showed predominantly positive responses, though these domains displayed slightly higher neutral opinions compared to the others. This indicates that students generally found the task trainer to be a valuable and effective educational tool for learning anterior nasal packing.

| Statement | Strongly Disagree (%) | Disagree (%) | Neutral (%) | Agree (%) | Strongly Agree (%) |
|---|---|---|---|---|---|
| Helped in retention of knowledge | 0.0 | 0.0 | 0.0 | 50.0 | 50.0 |
| I feel satisfied on doing nasal packing by myself | 0.0 | 0.0 | 12.5 | 37.5 | 50.0 |
| Improved my skill in anterior nasal packing | 0.0 | 0.0 | 0.0 | 0.0 | 100.0 |
| Confident about doing on a real patient | 0.0 | 0.0 | 6.25 | 56.25 | 37.5 |
| Active engagement in learning | 0.0 | 0.0 | 0.0 | 0.0 | 100.0 |
| Effective in learning nasal packing than lecture alone | 0.0 | 0.0 | 0.0 | 0.0 | 100.0 |
The table presents learner responses to six statements about Retention of knowledge, Satisfaction, Skill acquisition, Confidence, Active engagement and Effectiveness compared to lecture alone, after practising anterior nasal packing on a task trainer. Values are expressed as percentages of total participants (n = 80). Response categories include Strongly Disagree, Disagree, Neutral, Agree and Strongly Agree. Majority of students reported Agree or Strongly Agree across all domains, indicating overall positive perceptions of the task trainer as a learning tool. Neutral and negative responses were minimal, with slightly higher neutrality observed in the domains of confidence and satisfaction. Overall, this table demonstrates that the task trainer was well-received and perceived as beneficial for procedural learning.
The evaluation yielded overwhelmingly positive results. Learners provided feedback that the trainer was highly effective in enhancing their skills and confidence in managing epistaxis.
Key outcomes included:
•Improved skills: learners demonstrated significant improvement in their ability to perform anterior nasal packing.
•Increased confidence: the trainer instilled confidence in learners to manage epistaxis effectively.
•High learner satisfaction: learners expressed satisfaction with the trainer, citing its effectiveness in enhancing their learning experience.
These outcomes underscore the efficacy of the anterior nasal packing trainer in promoting skill acquisition, confidence and learner satisfaction.
Validation of this training model is needed. Model is stationary and does not actually ‘bleed’. Iterative improvements to the trainer’s design and functionality can be made after gathering feedback from users. Research can be directed to investigate how well learners retain and transfer their skills to real world clinical settings. This trainer can also be used to teach emergency medicine residents and practitioners how to manage epistaxis in urgent care settings.
The author wishes to acknowledge all faculties of Department of Otorhinolaryngology and Head and Neck Surgery, Government Medical College, Thiruvananthapuram, for the development of the trainer for anterior nasal packing and for the ongoing help in improving the user interface for medical training. Expressing special thanks to Mr. Shanoj PC, modeller in Department of Anatomy, Government Medical College, Thiruvananthapuram, for his imagination and competency in making this model a reality.
Single author contributed to manuscript preparation.
No sources of funding support.
Available on request.
None declared.
None declared.
1.
2.
Andrew Toby Merriman
ORCID:https://orcid.org/0009-0006-5034-5228
, Jan Engel-Morton, Stephen WaiteMeta-debriefing, or debriefing the debriefer, is established as an effective method of faculty development for simulation practitioners [1]. In NHS Lothian, a novel ‘Meta-Debrief Club’ (MDC) was formed in 2016 [2]. Novice simulation debriefers met weekly to critically appraise a whole debriefing brought by a participant. Using a combination of structured debriefing assessments and conversational tools, the discussion generated a list of actionable changes that the debriefer could incorporate into their practice [2].
Since then, the conversation on meta-debriefing has progressed. Kumar et al. advocated for formalized meta-debriefing training activities, reporting the view that meta-debriefing is more challenging than conventional simulation debriefing and requires specific expertise [1]. The NHS Lothian MDC has diverged from this interpretation. We frequently do not have access to expert meta-debriefers, and many of our faculty have less than a year of experience as simulation educators. For our faculty to benefit maximally from meta-debriefing, we have continued to adapt the initial MDC concept to improve the ease and effectiveness of novice facilitation, while maintaining psychological safety for participants. We outline how the MDC has evolved to meet our needs locally, and how this might be relevant to others.
The MDC is a community of practice of simulation educators [3]. As we often do not have access to expert meta-debriefers, we have made changes to the original concept that aim to advance the collaborative learning potential of the community and ensure it can continue to be led by novice faculty members.
Our first change has been to stop using debriefing assessments. We therefore clearly distinguish between meta-debriefing for learning as opposed to meta-debriefing for assessment of performance. Instead, we generate discussion using solely the Scottish centre debrief model [4]. This model is typically used to structure simulation debriefings in NHS Lothian, is well understood by our participants, and can therefore be used by even novice meta-debriefers.
Additionally, we have moved away from showing videos of full debriefings. Participants identify clips of up to 10 minutes that highlight areas of challenge or raise specific learning points. In line with experiential learning theory [5], this clip provides the substrate for a group reflection, where participants share similar experiences, and collectively develop ‘take-back-to-practice’ messages – strategies for developing our practice as debriefers. For the participant, this promotes comfort by allowing them to choose which clip is shown. For the novice meta-debriefer, we have found that facilitating discussion around shorter clips is often more straightforward. This approach also addresses previous concerns about the time it takes to review a full debriefing [2].
We enhance our novice community of practice by including our simulation technicians in the MDC. Our technicians have more years of experience as simulation educators than many of our debriefers and are well placed to discuss debriefing strategies that work well. Involving simulation technicians also allows the MDC to address issues of scenario design and delivery.
There is no one way of meta-debriefing [1], and we are keen to ensure that our current MDC works for our faculty. At the end of each MDC, we give participants an opportunity to discuss our current approach and to suggest changes that could be made. Additionally, after four meetings using the current format, 15 recent participants were sent questions via email evaluating the recent changes to the MDC in terms of educational value and psychological safety. We performed a pragmatic, inductive analysis of the free-text answers to identify key themes within the data.
Seven recent participants provided detailed qualitative feedback. Participants supported the use of the Scottish centre debrief model. They did not feel that using structured assessment tools would add to their learning.
I prefer the less structured format as this allows more free discussion and interaction within the group. (Participant A)
Comments were positive regarding the move to reviewing clips as participants felt this saves time that is better used for group discussion and learning. Feedback at the end of sessions aligned with these views, expressing a clear desire to continue reviewing shorter clips.
I feel you can get the discussion point across in 1-2 minutes and by showing shorter clips it allows much more time for discussion. (Participant B)
The changes to the MDC were designed to support facilitation by novice faculty and collaborative learning while maintaining the psychological safety of the group. Although we have not performed a systematic evaluation of psychological safety, all respondents agreed that the MDC is a psychologically safe space. This suggests that participants are prepared to take interpersonal risks by showing challenging debriefing moments in the service of group learning. In our experience, participants do contribute clips of vulnerable moments. Nonetheless, a possible limitation of this approach is that participants self-select clips with which they are most comfortable, rather than the clips that result in the richest learning conversations.
More research is required to determine the role of an expert meta-debriefer as an enabler of learning. Nonetheless, implementation of specific faculty development for meta-debriefers is challenging [1]. Our interpretation of the MDC has yielded positive results and may be transferable to other contexts where expert meta-debriefers are not available. We hope that our insights can empower other novice debriefers to benefit from the shared learning that meta-debriefing promotes.
Siobhan Connolly, Ed Mellanby and Nathan Oliver
None declared.
None declared.
None declared.
None declared.
None declared.
1.
2.
3.
4.
5.
Jennifer Louise Wood 1, Katherine Mitchell 1, Robyn Canham 1, Katie Hughes 1, Victoria R. Tallentire 1, 2
[1]
[2]
Healthcare educators increasingly acknowledge the critical need for sustainable practices but frequently experience feelings of helplessness or uncertainty when addressing the complexity of the planetary crisis. The global healthcare sector significantly contributes to environmental impacts, exacerbating the triple planetary crisis of climate change, biodiversity loss and pollution, which in turn exacerbate social and health inequalities. Simulation is a valuable pedagogical tool, but often relies on energy-intensive technologies and single-use consumables, which contribute to environmental degradation [1]. Despite strong motivation, often driven by personal concern for the future health of families and communities, educators struggle to initiate tangible sustainability actions within their practice. Simulation faculty and participants in NHS Lothian highlighted this challenge, emphasizing the need for practical and actionable guidance to bridge the gap between awareness and action.
In response to this identified gap, we developed a 90-minute interactive workshop titled ‘Introducing Environmental Sustainability to your Simulation Practice’ aimed at empowering educators through practical, evidence-based sustainability strategies. The workshop was advertised through the Medical Education Directorate and attended by a range of staff involved in the delivery of clinical education in Scotland. The innovation leveraged the creative and interactive methodology of Lego® Serious Play® (LSP), a technique recognized for its effectiveness in fostering innovative problem-solving, collaboration and deeper reflective thinking [2]. Participants were encouraged to share ideas and reflections by constructing individual Lego models that represented previous and possible future sustainability changes.
As shown in Figure 1, the workshop was divided into four sections: an introduction to the role of healthcare and simulation-based education in relation to the triple planetary crisis; an introduction to ‘carbon costing’ and a guide to calculating the carbon footprint of a simulation session; LSP tasks; and final thoughts, reflections and future pledges. Facilitators were doctors undertaking medical education fellowships, who had been trained at the Edinburgh Summer School in Clinical Education. The workshop was not directly funded but was developed as part of their fellowship roles. At least one facilitator worked as part of NHS Lothian’s Sustainability Working Group.


Overview of our 90-minute workshop (A) ‘Introducing Environmental Sustainability to your Simulation Practice’. (B) Photograph of a participant’s Lego® Serious Play® model in response to the question ‘Build a model that represents a sustainable change you would like to make in your education practice’. When describing the model, the participants detailed the lower bricks representing Quality Improvement (QI), the window representing a sustainable lens and the vegetation representing growth of the environmental sustainability QI projects, thus bridging the way to concerted action in their workplace.
Following an introduction to the role of healthcare in climate breakdown and carbon footprint calculations, participants were introduced to LSP tasks. During the third part of the session, educators engaged actively by building Lego® models that symbolized abstract sustainability challenges, thereby stimulating meaningful discussions and facilitating the generation of innovative, practical solutions. Whilst Lego® is made from petrochemicals, the blocks used in the workshop were already owned by participants or were second-hand. This hands-on activity also promoted non-hierarchical, collaborative interactions consistent with the educational principles for sustainable healthcare [3]. Examples of the LSP models constructed are shown in Figure 1. Throughout the workshop, participants shared their experiences, identified personal and institutional barriers, and worked collectively to propose realistic, implementable actions tailored to their simulation contexts. The development of context-specific ideas and personal pledges ensured that the workshop moved beyond theoretical discussions to practical action [4].
The immediate impact of our innovation was assessed through a structured feedback process following each workshop session. Both qualitative and quantitative data were collected, measuring participants’ perceptions of the session’s educational value, the practicality of the actions proposed and their willingness to recommend the workshop to colleagues. Additionally, participants were asked to formulate specific pledges to implement sustainable practices within their simulation activities. These pledges served dual purposes: reinforcing individual commitment to sustainability and fostering accountability within the group setting.
Initial evaluation involving 13 participants yielded strongly positive feedback. Quantitatively, 84% reported acquiring new insights into the environmental impacts of simulation-based healthcare education, and 100% indicated they would recommend the workshop to colleagues. Qualitative responses revealed deeper impacts, demonstrating that participants felt genuinely empowered to translate sustainability principles into actionable changes. Participants frequently described the workshop as informative, engaging and inspirational, with comments specifically highlighting the practical utility of the session. These testimonies underscored the effectiveness of the interactive, collaborative format in cultivating actionable commitment to sustainability. Table 1 summarizes the different areas of behavioural change planned by participants following the workshop.

| Behaviour changes planned by participants following workshop | |||
|---|---|---|---|
| Changes within own practice | Changes using sphere of influence | ||
| Reduce emails/attachments/printing | 5 | Include sustainability when reviewing, delivering and planning programmes | 6 |
| Recognize importance of small changes | 5 | Include sustainability in teaching and training | 6 |
| Equipment | 2 | Advocate for sustainability within clinical education | 12 |
| Consumables | 2 | Total | 24 |
| Sustainable travel | 2 | ||
| Appropriate waste segregation | 7 | ||
| Total | 23 | ||
These were categorized into areas of direct control and areas of influence, along with behaviour subcategories that participants decided to make changes in.
Building upon the promising initial outcomes, subsequent steps should involve evaluating the workshop’s long-term effectiveness through follow-up surveys several months post-intervention. Such an evaluation would determine the sustainability and actual implementation of pledged actions, offering richer insights into the lasting impact of the workshop. Additionally, expanding this innovation’s reach is essential. Further research and development could explore adapting the workshop format for wider applicability, including virtual delivery options, ensuring broader accessibility and greater potential impact across diverse healthcare educational settings. Current pilot sessions of the workshop are being run with clinicians and administrative teams. The adaptable nature of the methodology suggests significant scalability, allowing its integration into a variety of educational contexts, thereby advancing the global movement towards environmentally sustainable healthcare practices.
Ultimately, our innovation contributes to bridging the critical gap between theoretical awareness of sustainability challenges and the practical, incremental actions needed within simulation-based healthcare education. By empowering educators with knowledge, practical tools and a collaborative support network, we aim to foster sustained changes that cumulatively contribute towards achieving broader environmental and healthcare sustainability goals.
None declared.
None declared.
None declared.
None declared.
None declared.
1.
2.
3.
4.
Yasmeen Hayat 1, Maria Mahmood 1, David Wright 1, Eirini Kasfiki 1
[1]
acute care,augmented reality,simulated patients or standardized patients,simulation,and technology
Virtual (VR), augmented (AR) and mixed reality (MR) have gradually become integrated into a myriad of fields, including aviation and the transportation industry. The technology has now developed sufficiently for potential use in medical education. MR, the form used in this programme, projects digital information onto real-world objects.
There is growing evidence that these modalities can provide educational value to doctors in training [1]. However, most applications of this nascent technology in medical education have been in the realm of surgical technique and anatomy teaching [2–5], with little evidence of teaching the inductive reasoning and clinical assessment critical in internal medical environments.
The COVID-19 pandemic disrupted face-to-face teaching nationally, pushing educators to rely on technology to teach remotely. Resident doctors in the United Kingdom sometimes commute long distances to attend face-to-face teaching. There has been a documented reduction in attendance of teaching sessions in the local deanery, especially on non-clinical days. Simulation training, which allows for exploration of mental models and application of knowledge, is hard to run virtually. Could MR be a potential solution to this?
We conducted three pilot sessions at a tertiary hospital utilizing HoloLensTM, a Microsoft technology that projects interactive, three-dimensional content onto the real world (Figure 1). GigXR, a medical education company that developed educational MR software, provided the software for the sessions. The pilot sessions were chosen to reflect different educational settings (e.g. virtual and in-person) with small and larger groups of learners. The purpose of these pilots was to assess the feasibility of using this technology for interactive, simulation-based teaching in healthcare.
In Pilot 1, a remote teaching session was conducted with four resident doctors who were given a pre-determined scenario on anaphylaxis, showing a patient with the condition and their vital signs evolving in three different stages. The course facilitator used the headset while the candidates joined remotely through the mobile app and communicated with one another and the facilitator using Microsoft Teams.
In Pilot 2, a small face-to-face group session took place with five trainees given a scenario on heart failure. Each delegate was given a headset showing a simulated patient with the condition while interactive teaching on heart failure took place.
In Pilot 3, 34 resident doctors observed a volunteer take part in an MR-based simulation of an evolving asthma exacerbation requiring intervention. The scenario was projected onto a screen for all to watch.


How HoloLens runs in-person (picture of two candidates being shown how to use it, to include in the innovation part of the paper)
The trainees were asked for verbal feedback immediately after the session to glean their reactions to the technology and those in the third pilot also received a standardized teaching questionnaire where they rated different dimensions on a Likert scale of 1–5 to obtain quantitative data to support any conclusions drawn (Figure 2).
The technology proved difficult to use. Compared with traditional simulation with mannequins and actors, trainees reported glitches when using MR virtually, at times no longer seeing the patient. This issue even occurred in the face-to-face sessions. A technician had to be available to address issues in real-time.
Trainees did not feel that MR was the best way to be taught the material. They found it interesting and novel but asserted that interacting with real patients and partaking in real-world simulation is the most helpful. Trainers voiced similar concerns, citing the lack of escape routes and how the pre-recorded nature of the software prevented assessment of mental models. For example, in Pilot 1, the trainees watched the patient deteriorate, which added context but did not challenge mental models in the way simulation often can. Most MR software presents cases this way with technical difficulties making more interactive simulations challenging as compared to traditional methods.
Trainers repeatedly highlighted that using MR is labour-intensive and expensive. The two pieces of software we purchased cost a total of £20,000, while each headset cost £3000. Traditional simulation can be run much more cheaply with mannequins costing approximately £200.
Also, these cases could be found easily on any acute medical ward, so it is challenging to identify the benefits of MR for the average trainee who has access to bedside teaching.

Student feedback summary for pilot session 3 (rated one to five), graph showing feedback to be included in the outcomes section
MR showed promise but is distracting in its current form and struggled to assess mental models. Technical glitches remain distracting for students and prevent MR from facilitating learning to the same extent as traditional teaching. Although MR shows benefit for anatomy teaching [2–5], teaching for internal medicine benefits from more interactive simulation that the technology currently struggles to support.
This paper would fit into an assessment of Kirkpatrick’s hierarchy level 1, determining engagement of learners. As MR is a novel method, further study is required to assess the higher levels of Kirkpatrick’s hierarchy and its suitability as an independent teaching method. This requires ongoing evaluation as the technology improves and becomes more ‘life-like’, facilitating better interactivity.
None declared.
No sources of funding support.
None declared.
None declared.
None declared.
1.
2.
3.
4.
5.
Mohammed Abuzitoon
ORCID:https://orcid.org/0009-0006-9059-2645
, Ibrahim Tahacost effective,innovation,reviews,simulation,technology,and technology platforms
Reliable vascular access is essential in emergency and trauma care [1]. In simulation-based education, intraosseous (IO) access is taught as a rapid alternative when intravenous (IV) access fails particularly in cardiac arrest, shock or trauma scenarios [2].
Evidence demonstrates faster medication delivery and higher first-attempt success rates with IO compared to IV access, especially in prehospital and critical care settings, making IO training a core component of life support and trauma simulation curricula [3,4].
However, frequent use of battery-powered IO drills creates operational and financial strain, as the device must be fully replaced once its sealed battery is depleted, at a cost of 610–660 USD per unit [5].
This report describes a cost-effective modification converting a battery-powered IO drill into a wired device to improve reliability and reduce costs.
The original IO driver contains a sealed, non-replaceable lithium battery designed for up to 500 insertions. As the battery is neither rechargeable nor replaceable and provides limited warning before depletion, the entire unit must be discarded, prompting the transition to an external power source.
We modified the IO drill by replacing its internal battery with a reliable external DC power supply. The motor wires connected to a Newstar NSC-30-regulated power supply (AC 100–240 V; DC 12–30 V) (Figure 1). Compatibility testing confirmed 15 V (4100 mA) as optimal, powering the drill effectively without overheating or torque loss.


Modification of a battery-powered IO drill to an externally powered DC system.
The drill was opened, the battery disconnected and the motor leads soldered to insulated wires connected to the DC output. A small casing opening enabled wall socket connection, eliminating charging requirements and ensuring uninterrupted use (Figure 1).
The modified IO drill was initially evaluated during a defined pilot period from October 2019 to January 2020 across ten simulation sessions. These sessions were overseen by a Certified Healthcare Simulation Operations Specialist (CHSOS), who monitored performance and user feedback. The modified drill was used alongside the original battery-operated version to allow real-time comparison under typical training conditions.
Informal feedback from educators and operations staff highlighted reliable motor function, absence of mid-session power loss, and rapid user adaptation to the wired configuration. Since the pilot, the modified drill has remained in active use from 2019 to the present in various high-volume programmes, demonstrating long-term reliability and durability.
Over three years (2020–2023), the modified IO drill was consistently used in vascular access stations across diverse simulation-based training programmes. It supported over 12 ATLS courses (192 learners) and 50 PALS courses (600 learners).
The device demonstrated stable performance with no reported motor failure, activation delays or torque loss. Faculty value the improved reliability, reduce setup time and elimination of battery-related disruptions.
The modification process required less than one hour using basic tools, with a total cost of approximately 25 USD. In contrast, replacement IO drills cost 610–660 USD per unit. This resulted in substantial cost savings and dependable performance in high-frequency training environments (Table 1).

| Item | Description | Cost (USD) |
|---|---|---|
| Existing IO drill | Already available, battery depleted | 0 |
| Heat shrink tubing | For electrical insulation (small length) | 1 |
| Newstar NSC-30 power supply | Switching adapter, 15 V / 4100 mA | 23 |
| Insulated copper wires | Short segments for internal wiring | 1 |
| Total estimated cost | 25 | |
This small-scale innovation demonstrates how simulation centres can address operational gaps through low-cost, practical modification. Given the increasing emphasis on sustainability in simulation-based education, especially in low-resource and high-volume programmes, such approaches may guide others facing similar constraints.
We are currently exploring the integration of a portable rechargeable power bank to enable mobile simulation without wall-socket dependency, expanding use beyond fixed settings.
Future work should involve formal usability testing and direct comparison between battery- and DC-powered drills to assess user satisfaction, performance and session flow. A cost-benefit analysis could also quantify operational savings and reliability gains.
This project highlights a broader issue in simulation: operational sustainability is often overlooked despite its impact on reliability and cost effectiveness. Simulation operations specialists play a critical role in developing practical, sustainable solutions without compromising training quality.
Instead of limiting simulation growth due to financial constraints, institutions should invest in skilled operations teams of sustainable innovation. This project demonstrates how empowered people, not technology alone, drive resilient simulation programmes.
None declared.
No sources of funding support.
None declared.
None declared.
None declared.
1.
2.
3.
4.
5.
Charlotte S.M. Boyle 1, Melissa L. Watts 1, 2, Rory A.H. Trawber 1, 3, Leah R. Proctor 1
[1]
[2]
[3]
Health professions education,In situ simulations,Scenario development,Simulation,and Simulation modality
In March 2024, the Western Australian government announced the reopening of a 75-bed standalone private mental health facility, Cockburn Health, as part of the public Fiona Stanley Fremantle Hospitals Group (FSFHG). The site, opening August 2024, would include the state’s first specialist eating disorder facility and beds for medically supervised drug and alcohol withdrawal. During the commissioning period, staff expressed concern regarding acute patient deterioration, as psychiatric clinicians would be the initial responders without onsite critical care support services.
In May 2024, FSFHG’s interprofessional consultative simulation service, Simulation To Enhance Patient Safety (STEPS), was engaged by the Cockburn Transition Team to assist with facility and staff readiness for responding to acute patient deterioration. Established in 2018, STEPS is built on strong relationships with key individuals in clinical and non-clinical services to enable translational simulation activities across departments in the hospital network [1]. The framework for planning and delivery of simulation activities, used by STEPS, is well established, following the input–process–output framework described by Nickson et al. [2], summarized in Figure 1.

![STEPS translational simulation consultative service framework [1]. Facilitators begin with a needs analysis, followed by a tabletop exercise and walkthrough of the space with interest holders (if conducting systems and space testing activities). The main scenario is designed and delivered, followed by a systems debrief using the modified PEARLS framework [3]. Identified latent safety threats are allocated a risk rating (from low to extreme) in keeping with standard risk reporting within Western Australian Health. These are then reported to pre-identified interest holders (including hospital executives) to be addressed. From this point, a decision is made to either re-test or endorse the system or space.](/dataresources/articles/content-1774925406025-a27d2946-1d63-4700-a493-9b4767c253d7/assets/cnsm4560_f0001.jpg)
STEPS translational simulation consultative service framework [1]. Facilitators begin with a needs analysis, followed by a tabletop exercise and walkthrough of the space with interest holders (if conducting systems and space testing activities). The main scenario is designed and delivered, followed by a systems debrief using the modified PEARLS framework [3]. Identified latent safety threats are allocated a risk rating (from low to extreme) in keeping with standard risk reporting within Western Australian Health. These are then reported to pre-identified interest holders (including hospital executives) to be addressed. From this point, a decision is made to either re-test or endorse the system or space.
STEPS partnered with mental health clinicians, the Cockburn Transition Team and emergency response coordinators. We believed combining two simulation-based interventions would best address staff needs:
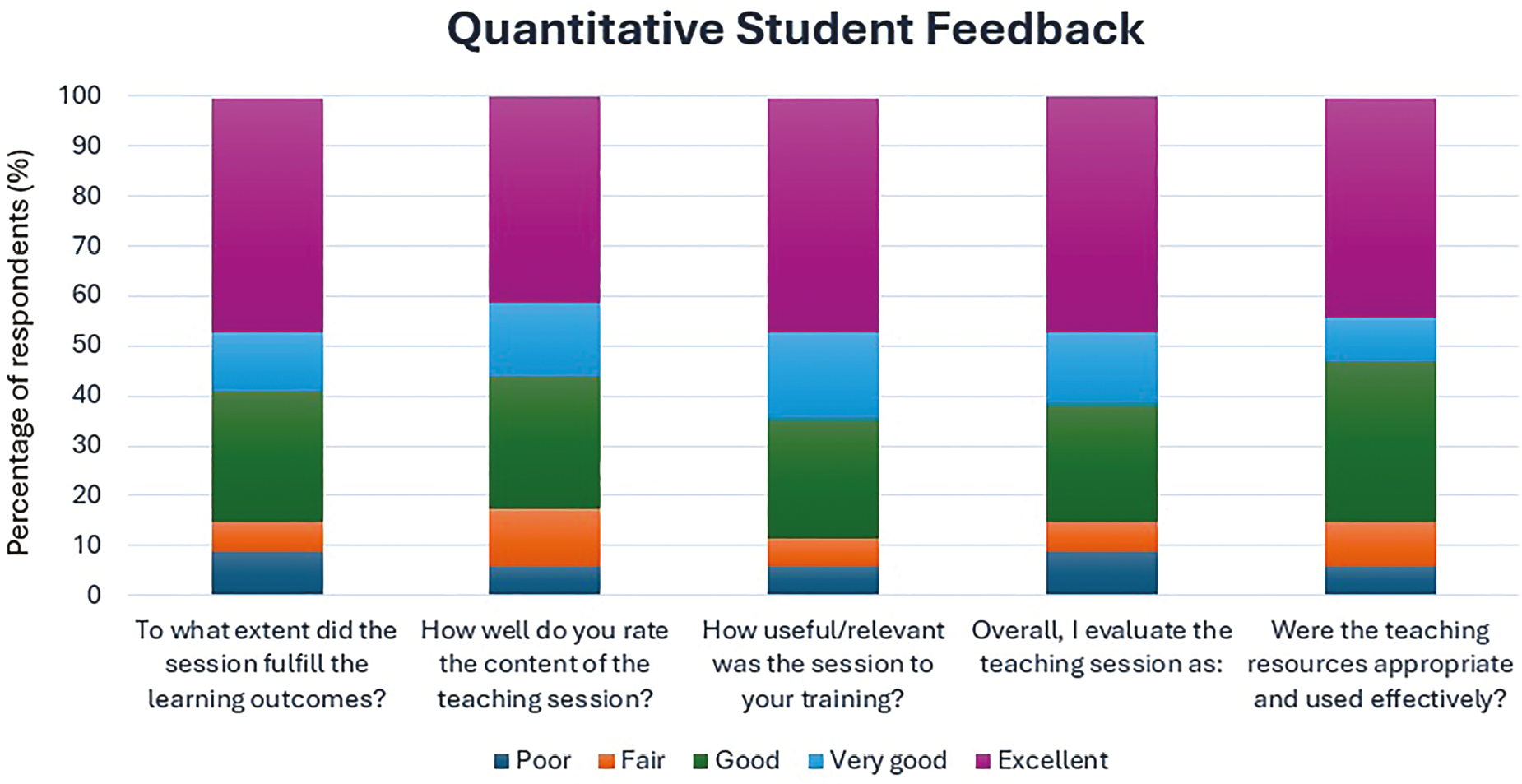
1.Educational simulation: We designed and delivered half-day workshops, covering core medical emergency response skills. Content included site-specific escalation pathways, structured patient assessment, airway management and life support based on pre-existing FSFHG hospital life support checklists. Participants applied learned skills in three in situ simulation scenarios (based on recent FSFHG mental health emergency response calls).
2.Translational simulation: Using the STEPS framework, the three in situ scenarios were developed to identify latent safety threats in processes surrounding medical emergency and threat of physical harm calls.
Pre- and post-workshop surveys measured participants’ confidence in new site escalation pathways, and perceived structure and confidence in managing acute patient deterioration. A Likert scale was used for rating from 1 to 5. For systems testing, we followed the STEPS framework (Figure 1).
Twenty-two clinicians attended the workshops, including psychiatrists, doctors undergoing postgraduate training and nursing staff. We obtained 15 paired samples of questionnaire data that were analysed using the Wilcoxon signed-rank test, which demonstrated statistically significant improvements across all areas (P < 0.05) except confidence managing tachyarrhythmias and hypotension (P = 0.095 and P = 0.31, respectively). Overall confidence in managing patient deterioration and a structured approach to assessment had a statistically significant (P < 0.001) modest improvement (median score 3–4 for each), and confidence in escalation pathways improved greatly (median score 1–4) with high statistical significance (P = 0.00061 × 10−1) (Figure 2).

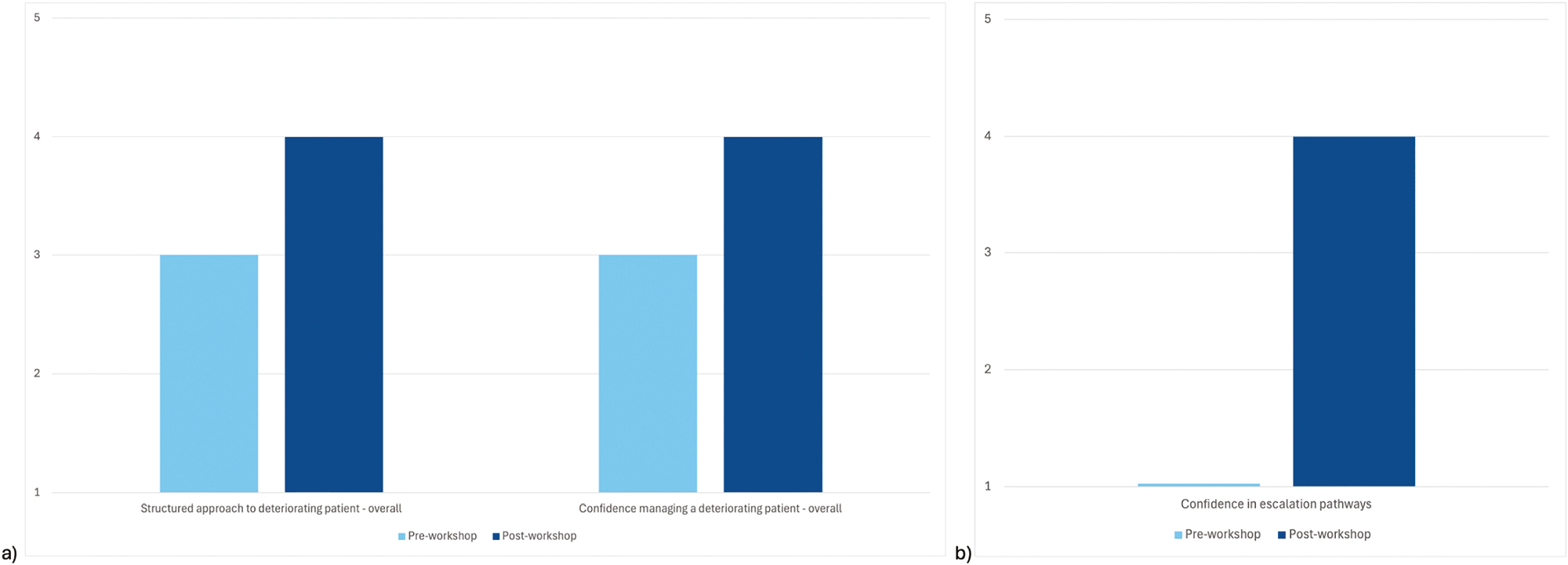
Median participant responses to pre- and post-workshop questionnaire. Likert scale from 1 to 5 for questions regarding structured approach to a deteriorating patient (1 not at all structured, 2 somewhat unstructured, 3 neutral, 4 somewhat structured, 5 very structured), and confidence managing a deteriorating patient and confidence in escalation pathways (1 not at all confident, 2 somewhat confident, 3 neutral, 4 mostly confident, 5 very confident). (a) Overall paired data of pre-workshop and post-workshop structure and confidence managing deteriorating patients. N = 90 (15 paired responses to 6 deteriorating patient situations: tachyarrhythmia, reduced GCS, seizure, cardiac arrest, hypotension, airway compromise). Overall structure Wilcoxon’s statistic = 97. Structure significantly improved, P < 0.001 (P = 0.0008336 × 10−6). Overall confidence Wilcoxon’s statistic = 114. Confidence significantly improved, P < 0.001 (P = 0.000101 × 10−3). (b) Confidence in escalation pathways. Paired data N = 15. Wilcoxon’s statistic = 0. Statistically significant improvement in confidence, P < 0.001 (P = 0.00061 × 10−1).
Medical emergency call testing identified 13 risks (6 high risk). Threat of physical harm call testing identified 12 risks (4 high risk). These were reported to hospital executives for resolution prior to opening.
Combining simulation for education with translational simulation is an innovative approach. We believe the strength of this approach lies in its capacity to comprehensively serve the needs of both the organisation and staff transitioning to the facility. This aligns with Brazil and Reedy’s recent views on the false dichotomy between ‘educational simulation’ and ‘translational simulation’ [4]. This approach is likely transferable to other settings where workplace changes alter clinical duties.
A major strength of the project is the relationships formed with hospital executives and Cockburn clinicians. We encourage healthcare simulation services to build strong relationships with key interest holders and establish a structure for translational simulation delivery, much like that of STEPS, as our pre-established framework was critical to implement an effective intervention in under 3 months. These relationships have enabled us to establish further simulation activity at Cockburn Health, including a programme of regular in situ interprofessional simulations.
Interestingly, the most significant impact of the intervention was boosting staff confidence in escalation pathways at the new site. This further highlights the benefit of adding an educational component to translational simulation. Through the in situ simulation activities, the STEPS team was able to orient clinicians to their new workplace. Though not the primary focus of data collection, free-text responses indicated that the simulations relieved anxiety about the transition and increased empowerment, supported by comments like ‘learning more information about Cockburn’, ‘info[rmation] re: escalation pathways’ and ‘confidence building’. Recent literature similarly describes positive effects of translational simulation on frontline staff during change management [5]. We believe that combining educational and translational simulation enhances this effect by enabling further information sharing and additional capacity to address staff concerns.
A limitation of this work is that the data are of participant perspectives rather than objective performance or clinical outcomes. We were also unable to collect sufficient follow-up data to assess sustained impact. We are strategizing how to effectively do this and look forward to continuing the simulation at Cockburn Health and assessing its impact on staff readiness for acute deterioration.
None declared.
None declared.
Data can be provided by the corresponding author on request.
All survey participants gave informed, written consent. Project approved by Governance Evidence Knowledge Outcomes (GEKO) quality improvement system. Quality activity number 54242.
None declared.
1.
2.
3.
4.
5.
Guy Dominic Collins 1, Louise Elizabeth Bolton 1
[1]
disaster medicine,nursing,nursing education,realism,fidelity,authenticity,and simulation
Since 2023, the University of Derby’s MSc Nursing programme has integrated high-fidelity major incident simulations. This initiative develops emergency preparedness skills and knowledge, adhering to the UK NMC Standards of Proficiency [1] and Core Competencies in Disaster Nursing V2 [2]. The NMC standards stress understanding the roles and responsibilities of nurses and other professionals in managing major incident care.
Multiple studies indicate that many nurses feel ill-equipped to handle emergency situations effectively. A systematic review found that a significant number of nurses globally reported insufficient knowledge and skills pertinent to disaster response, which applies to the UK context as well [3]. Specifically, a lack of structured disaster training programmes has been identified as a major barrier to effective response among nursing professionals, reflecting broader systemic issues within healthcare disaster preparedness and response that also affect nurses in the UK [4].
There is a critical importance of emergency and disaster preparedness among pre-registration nursing students, highlighting the need to equip future nurses with the skills and adaptability required to respond effectively to unforeseen events and evolving role expectations in the context of potential disasters [5]. While participation in a major incident may not be a routine clinical practice, no nursing discipline should assume exemption. It is essential that all nurses possess fundamental knowledge and adaptable skill sets to enable effective responses.
The programme team advocated moving beyond didactic teaching. They recognized that engaging student nurses in major incident simulation-based learning (SBL) more effectively builds familiarity with emergency scenarios, strengthens interdisciplinary role association and fosters the confidence and proficiency required to respond to high-pressure situations.
Since its inception, the team has delivered a range of scenarios, inclusive of unexplained campus-based explosions, knife and firearm assaults and major road traffic collisions. These simulations were designed and implemented in aligned with a conceptual framework for simulation-based education in emergency nursing and disaster preparedness. Developed to help guide simulations, ensuring consistency, safety and achievement of measurable learning outcomes [6].
Key innovations played a pivotal role in enhancing the depth and impact of SBL for major incident preparedness, including the use of trigger films to set the context and help ‘switch on’ students as part of their pre-brief preparations, emotionally and cognitively priming them for the scenario ahead. The integration of action outputs alongside overarching learning outcomes ensured clarity of purpose and measurable performance. Interdisciplinary involvement of the regional and voluntary ambulance services in stages of the simulation, contributed to the realism and recognition responses are typically multi-agency [7]. The involvement of many simulated patients, complete with moulage and prosthetics, added realism beyond the clean manikins’ students were more familiar with, helping to evoke authentic emotional and clinical responses.
The inclusion of unanticipated events, such as non-English-speaking simulated patients, aggressive or distraught relatives arriving at the receiving centre, planted examples of incompetent practice by other participants and persistent demands from simulated press incursions all contributed to further challenging the students’ clinical reasoning, communication and prioritization under pressure. Tools such as ‘get out of gaol’ cards and ‘stop moment’ cards were introduced to promote psychological safety, offering students the option to pause, reflect or seek support during critical moments. Live and post-simulation well-being support was accessible in the event of incident exposure distress. The get out of gaol cards provided a safety net to ask questions, although rarely used; students consistently chose to work collaboratively to resolve challenges. Reinforcing teamwork and professional resilience.
Crucially, the use of immediate hot debriefs utilizing the STOP5 framework [8] provided a structured opportunity for students to process experiences while emotions and tensions were still heightened, supporting emotional regulation and initial reflection. This was complemented by subsequent eclectic cold debriefs, conducted after a period of consolidation, enabling more objective individual and collective reflection.
Together, these innovations contributed to deeper engagement and a more immersive and professionally relevant educational experience.
The major incident simulations’ effectiveness and ongoing development were guided by student evaluations, simulated patient feedback and stakeholder contributions (including emergency response services). Concurrently, research used a bespoke proficiency framework to explore student self-efficacy levels. Repeated evaluations and key innovations have significantly enhanced the validity and authenticity of the student experience by deepening scenario realism, strengthening engagement and enriching immediate take-away learning.
Preliminary research data from pre/post-simulation participant reporting against self-efficacy statements and qualitative focus groups, demonstrated a consistent and measurable shift towards heightened levels of student self-efficacy immediately following participation in the major incident simulation, highlighting the pedagogical value of immersive experiential simulated learning in preparing students for potential real-world clinical challenges.
Further longitudinal research will examine the long-term impact of major incident SBL on graduates’ professional identity, clinical confidence and interdisciplinary collaboration. This requires understanding how SBL is consolidated post-graduation. Challenges involve tracing dispersed graduates and addressing varying engagement in follow-up.
None declared.
None declared.
None declared.
None declared.
None declared.
1.
2.
3.
4.
5.
6.
7.
8.