
The terms ‘co-production’, ‘co-design’ and ‘co-creation’ are often used interchangeably, and are now more commonly used in healthcare. These terms describe an exchange relationship between stakeholders (including those with lived experience) and the project leader to capture different perspectives and have an outcome that is more accepted. However, in simulation, not many studies label the exchange relationship as such and therefore evidence cannot be easily gathered.
This scoping review aims to clarify the use of these terms within healthcare simulation by systematically identifying the studies that employ co-production with service users. By scoping and synthesizing the available literature on the involvement of people with lived experience, we will examine when such engagement constitutes ‘lived experience co-production’ versus more generic forms of service user involvement. We will carry out systematic searches with MEDLINE, CINAHL Plus with Full Text, APA PsycINFO and Scopus. PRISMA-ScR guidelines for scoping reviews will be followed. This protocol has been registered with the Open Science Framework (OSF): https://doi.org/10.17605/OSF.IO/Q6SFK.
We anticipate that this scoping review will define lived experience co-production in healthcare simulation, by distinguishing it from other forms of service user involvement and raise awareness about the value and prevalence of co-production in this field.
The terms ‘co-production’, ‘co-design’ and ‘co-creation’ are frequently used interchangeably and have become buzzwords in several fields such as social services, healthcare and citizen science [1–4]. In the widest sense, these terms imply exchange relationships, which include different forms of interaction (e.g. conversations, roleplaying or designing together with an output) and this can happen at different levels such as the individual service user level, the organizational level or in the meso-levels between. The aim of these exchange relationships is to involve a larger range of stakeholders with different knowledge domains (e.g. experience, expert insight) to improve outcomes in terms of service or product acceptance and experience, as well as quality and efficiency.
Despite this overall trend of collaboration and involvement in the planning and making [1–4], there seems to be very little evidence labelled as ‘co-production’ and reported in simulation education and practice. Brief explorative searches of the MedLine and CINAHL databases using the terms ‘co-production and health* and simulat*’ in abstracts and titles produced only a very few relevant results. However, we know that these exchange relationships between a person with lived experience and simulationists take place [5–8]. Particularly, in healthcare simulation, where people with lived experience are included to contribute partly to achieve more realistic scenarios, partly to increase empathy and authenticity, yet this is not always labelled as co-production [9,10].
To bring clarity to the use of the terms ‘co-production’, ‘co-design’ and ‘co-creation’ in the context of healthcare simulation education and practice, we are conducting a scoping review of peer-reviewed primary research studies and in-practice reports published in journals (including not-peer-reviewed ones) to understand when ‘lived experience co-production’ has been applied in contrast to service user involvement. Throughout this document we will use the term ‘person with lived experience’ when referring to the concept of any expert patient or service user involved at any stage of the simulation ideation, development and delivery process. As an interdisciplinary team based at the University of Greenwich, we bring together expertise in simulation practice, participatory and co-production research methods, design and academic scholarship, alongside lived experience. Our shared interest is in laying a robust conceptual foundation for understanding how co-production, particularly involving lived experience, is enacted within simulation education and practice. The scoping review will identify all primary research journal articles that meet the inclusion criteria, and through textual narrative synthesis [11] will explore themes that emerge within the current knowledge base and map this onto our framework as described in the following.
Simulation has been defined as ‘a technique-not a technology – to replace or amplify real experiences with guided experiences that evoke or replicate substantial aspects of the real world in a fully interactive manner’ [12]. Simulation in healthcare can be for educational purposes, or ‘to transform health & care through collective understanding, insight and learning’ – transformative simulation [13].
In order to create simulation activities, be it a defined learning experience in groups using role play or immersive experiences with or without technology or a single-person experience stepping virtually through an immersive environment where decisions need to be made, the simulationists need to ‘design’ the experience.
This designing of the simulation scenarios happens in many variations in different locations, such as simulation centres, in the lecturers’ offices or at the simulation production companies. Every design process, which at its core is a problem-solving process [14,15], has a minimum of two phases: (1) the exploration of the problem phase and (2) the development of the solution phase. Of course, design processes are frequently more elaborate and can have more phases. Two of the most well-known processes are the user-centred design (UCD) process and the UK Design Council’s double-diamond design process [15,16].
The UCD process places the user, i.e. a human, of the to-be-designed solution into the focus of the iterative process and whilst the designers move through the phases of ‘observation’, ‘idea generation’, ‘prototyping’ and ‘testing’ always checking with the user on the solution’s development. This makes the design process iterative, and the designed outcome is more likely to be authentic, expected and accepted by the end user. The phases of ‘observation’ and ‘idea generation’ can also be called ‘discovery phase’ i.e. the beginning where the simulation designer explores the context and situation for the scenario. The simulation designer may make use of their own experiences to inform the scenario design, yet this task is likely to be augmented by getting insights on the wider context and on specific details from patients or service users with lived experience. This is followed by the ‘definition phase’, where the idea is put on paper or a prototype is built. This is an iterative process until the outcome is workable for the simulation designer. The next step is to run the simulation and in some circumstances collect feedback from the participants, simulationists and the participating person(s) with lived experience to evaluate the experience.
As simulationists usually intend to create experiences that are authentic, meaningful and transformative, it is advisable to adopt a user-centred approach by involving service users or experts by experience to achieve exactly that. For this, we have mapped the user-centred approach onto simulation design for involving persons with the lived experience via co-production (Figure 1). We re-labelled Norman’s four phases of the UCD process to ‘Discovery’ (to replace observation & idea generation), ‘Iterative Design’ (to replace prototyping), ‘Delivery’ and ‘Evaluation’ (to replace Testing).

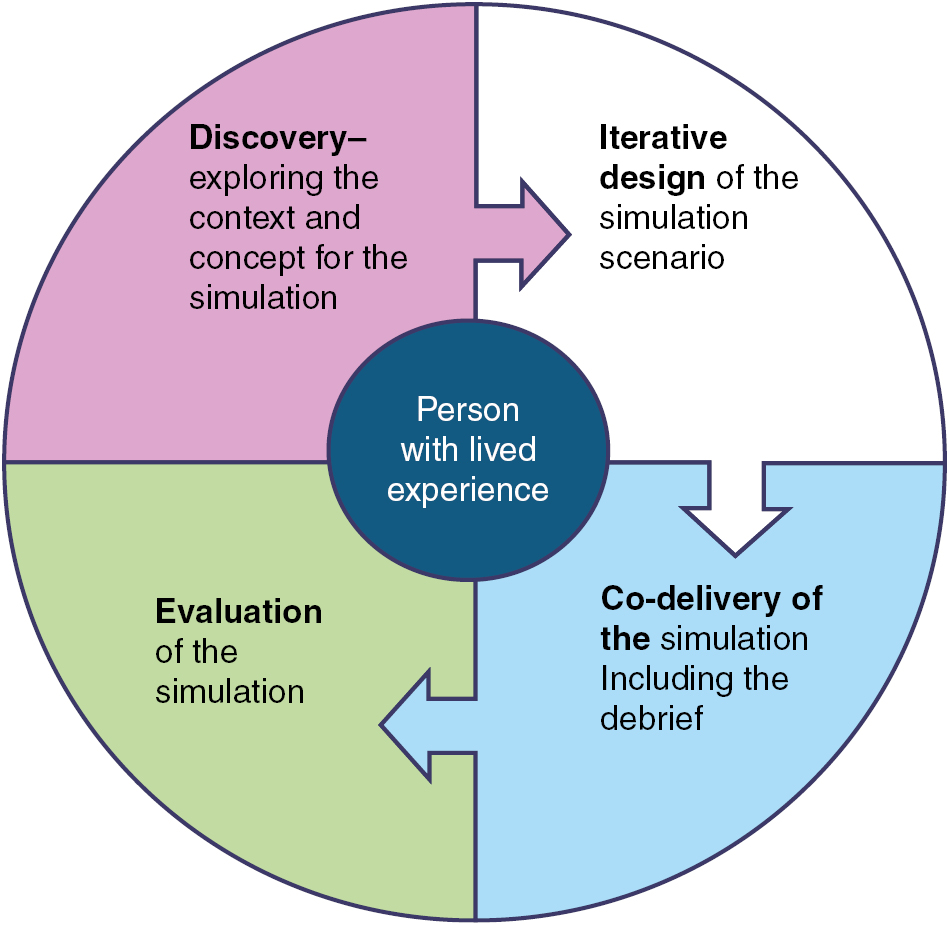
Norman’s UCD process mapped onto the simulation design and delivery cycle whilst involving the person with the lived experience (or service user) by placing them at the centre of the activities
In the current literature there is no clear definition of co-production within the context of healthcare simulation. There is no mention of terms ‘co-production’, ‘co-design’ and ‘co-creation’ nor the terms ‘lived experience’ or ‘expert by experience’ in the Healthcare Simulation Dictionary [17]. However, there are several definitions for the concept of co-production in general healthcare, and some within the context of research and practice. The Social Care Institute for Excellence (SCIE) highlights that co-production ‘describes working in partnership by sharing power between people who draw on care and support, carers, families and citizens’ [18]. They explain that there is no single formula for working in co-production, but include reciprocal and mutual working, break down the barriers between professionals and those who draw on care and support, and facilitate services by helping organizations become agents for change, rather than just being service providers.
The SCIE highlights the four stages of co-production: co-design including planning of services or protocol creation, co-decision making in the allocation of resources for prioritization, co-delivery and co-evaluation of the service or research [12].
The National Institute for Health Research (NIHR) provides a definition titled INVOLVE, which relates solely to research. It reflects their belief that members of the public have skills and knowledge that are of equal value to the researchers and defines this as ‘an approach in which researchers, practitioners and the public work together, sharing power and responsibility from the start to the end of the project’ [19].
The most expansive definition of co-production is that of the People Hub [20], a collective working to empower people with lived experience to use their voice in decisions, rather than speaking on behalf of them. The People Hub developed a ‘Spectrum of Participation’, which highlights the different ways that people can be invited to work together and share ideas and perspectives with organizations. It shows how co-production is distinct from other forms of participation, with the spectrum ranging from informing (‘doing to’), through education, consultation, engagement, co-design and finally to co-production (‘doing with’). Their definition outlines that while co-design is an effective way to involve people with lived experience, the intended objective has already been set, whereas co-production involves collaboration with people with lived experience from the outset, allowing partnership in the exploration, priority setting and objectives for change. This means that work must be in-depth and long-term, with a select group of consistent people.
Whilst this is an ideal definition with regards to reciprocity, equity and power sharing, we as the authors are pragmatists and understand that this level of involvement might not be possible in the real world due to time constraints, financial considerations and the level of involvement people with lived experience can reasonably contribute to research and educational projects. Therefore, as authors, we define co-production within healthcare simulation as: ‘a way of working that involves people who use health and care services and who have lived experience of a particular condition, or have protected characteristics or are from a specific socio-demographic background and/or their respective carers’. We stipulate that service users and carers need to engage in at least two of the four phases of the simulation cycle (discovery, iterative design, delivery and evaluation) for it to qualify as ‘lived experience co-production’, which otherwise would be considered as only involvement of service users in one of the simulation activities.
Building on our definition, we therefore aim to review the evidence in the academic literature for studies that utilized co-production within healthcare simulation in practice and education.
Our research question, therefore is: How has lived experience co-production been applied in health & care simulation?
•To scope the evidence for co-production within healthcare simulation in practice and education by searching the literature.
•To map the resulting studies, which report on co-production activities, onto our framework to understand the level of co-production.
•To develop literature-derived recommendations on best practices for co-production within healthcare simulation.
The scoping review employs a systematic search to scan the literature and to provide a synthesis with the aim ‘to map the literature on a particular topic or research area and provide an opportunity to identify key concepts; gaps in the research; and types and sources of evidence to inform practice, policymaking, and research’ [21]. Building on the original framework [22], this involves the following steps: (1) identification of area of interest, (2) literature search to identify relevant studies, (3) study selection, (4) data charting by extracting data in tabular (or graphical) format for the purpose of data synthesis and (5) data summary and write-up [21,22]. This review follows a data-based convergent synthesis design employing the textual narrative synthesis approach and by mapping it onto our co-production framework. The convergent design implies qualitative, quantitative and mixed-methods studies are identified in a single search and integrated throughout analysis, synthesis and presentation [11,23]. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR guidelines [24]) are followed. The Population Concept Context (PCC) framework [25] guided the articulation of the research question and the development of the research strategy and keywords.
This protocol has been registered with the Open Science Framework (OSF): https://doi.org/10.17605/OSF.IO/Q6SFK.
The following criteria, derived from the PCC framework (Table 1) [25], will be applied to identify relevant literature for this scoping review.
We will search for articles that include service users, patients or persons with specific characteristics such as homelessness, or with a disability and/or their carers at any stage of the healthcare simulation. This population group tends to inform the simulation scenario with their ‘lived experience’, to give more realistic details and authenticity to the simulation experience. This population is also ‘expert by experience’ as they live with it.
Involvement of proxies for those service users, who can consent, will not be considered as presenting direct ‘lived experience’ and therefore the study would be excluded. Involvement of stakeholders or other professionals who may have expert knowledge on a condition will also not be considered as the ‘lived experience’ and thus excluded.
All articles that present the involvement of service users, patients and/or persons with lived experience (e.g. a health condition or homelessness) in healthcare simulation education and practice will be included.
All studies must have taken place in the context of healthcare simulation education and practice. Studies that address other fields (e.g. space travel simulation or mathematical modelling) will be excluded.
1.All studies that use the term(s) ‘co-production’ or ‘co-design’ or ‘co-creation’ and/or ‘lived experience’.
2.Is focused on simulation in healthcare.
3.Includes people with lived experience of a particular condition, or who have protected characteristics, or are from specific socio-economic backgrounds and/or their respective carers.
4.People with lived experience must have been involved in any of the four phases of simulation activities, which are: discovery, iterative design, delivery and evaluation.
5.All primary peer-reviewed literature (qualitative, quantitative and mixed-method research) or in-practice reports published in journals or conference proceedings (including those that are not peer-reviewed).
1.Commentary, expert opinion, dissertations, essays, practice guidelines, systematic or narrative review articles.
2.Studies not related to healthcare.
3.Studies that are not peer-reviewed, except in-practice reports.
To identify relevant literature, we will systematically search the following databases: MEDLINE, CINAHL Plus with Full Text, APA PsycINFO (via EBSCOhost Health Science Research Database) and Scopus. In addition, we will hand-search the reference list of the eligible articles to identify any additional evidence for ‘lived experience’ co-production.
Our search strategy is framed by the data-based convergent design, for which we have formulated one search string based on the keywords below. For the latter, we consulted with a subject librarian to ensure our search string works well in the EBSCO databases as well as Elsevier’s Scopus.

| Population | ‘expert patient’ OR ‘expert by experience’ OR ‘service user’ OR ‘lived experience’ |
| OR | |
| Concept | co-prod* OR co-creat* OR co-design* OR coprod* OR cocreat* OR codesign* |
| AND | |
| Context | simulat* OR ‘part-task trainer’ OR ‘scenario-based learning’ OR virtual OR ‘augmented reality’ OR ‘role play’ OR mannikin* OR mannequin OR ‘clinical skills’ OR ‘skills-based learning’ OR ‘simulated patient’ OR mock* OR ‘standardi* patient’ OR actor* OR ‘patient educator*’ OR ‘immers*’ OR gaming OR gamification OR ‘problem-based learning’ OR ‘experiential learn*’ OR ‘in-situ’ OR ‘insitu’ OR ‘in situ’ OR ‘simulation-based education’ OR ‘simulation-based training’ OR ‘interprofessional educat*’ OR ‘distributed simulat*’ OR ‘sequential simulat*’ |
| AND | |
| health* OR medic* OR nurs* OR clinic* OR physician* OR pharmac* OR midwi* OR dieti* OR occupational therap* OR paramed* OR dent* OR radiograph* OR hospital OR surg* OR ‘operating department practitioner*’ OR anaesthe* OR physiotherap* OR psycholog* OR ‘emergency respon*’ OR ‘public health’ OR community |
We excluded the term ‘patient’ as it is expected to produce an unmanageable number of results.
In addition, we plan to search the reference lists of the retrieved articles for further evidence, as well as hand-searching the Journal of Healthcare Simulation, Advances in Simulation, Simulation in Healthcare and Clinical Simulation in Nursing, for any literature that may have been missed with the database search. We plan to complement this with Google Scholar searches (up to the first ten pages) to ensure that we have not missed any results which are not captured by the database and hand search activities.
All articles that meet all inclusion criteria and undergo full-text screening (by two assessors) are included in this review (tracked using PRISMA guidelines). We plan to use Rayyan.ai to support us with the de-duplication of results, the screening and support commentary. In the article identification phase, two reviewers will independently read the full articles and score them against the inclusion and exclusion criteria. If there are differences between the reviewers’ opinions, a third reviewer will be sought to resolve the matter by having a deciding vote.
Two authors will extract the following data from the selected articles: author, year of publication, country of publication, title, aims/purpose, healthcare discipline, simulation modality, findings, outcome measured (if applicable). Furthermore, the level of involvement by the service users/person with the lived experience will be mapped onto the four phases (discovery, iterative design, delivery and evaluation) of the simulation. Benefits of this involvement will also be extracted, given these have been reported.
We will employ the textual narrative synthesis approach [11] to create this overview of studies in healthcare simulation that involves services users/persons with lived experience. They do this by going into the detail of the studies and by mapping the studies onto the simulation design cycle. As soon as the involvement covers more than two phases, this will show succinctly the evidence for lived experience co-production.
We have decided against carrying out a critical appraisal of the resulting studies as we aim to show the breadth and types of co-production. Once co-production is integrated and labelled as such in simulation education and practice, then we will consider appraising the evidence critically with any future scoping and literature reviews.
We aim to capture relevant studies in one database convergent search query, yet there is the possibility that we may miss some literature which involves services users or persons with lived experience but not covered by our keywords. We have offered different definitions of co-production and developed our own framework to situate ‘lived experience co-production’ into the simulation cycle. At the same time, we acknowledge that other definitions of co-production may lead to a different way of conceptualizing the activity and therefore some evidence in academic, practice or grey literature may be missed. Although we thrive to be reflexive and inclusive our author team consists of three White women, which will bring their own biases. As such, during the scoping review process, the authors will extend the project and include more collaborators from a variety of backgrounds and perspectives.
Our scoping review aims to present an overview of the ways in which co-production alongside people with lived experience has been applied within simulation education and practice in healthcare. We will highlight those studies which can serve as a benchmark for good practice and provide recommendations for future lived experience co-production activities within healthcare simulation.
We anticipate the review findings to have the following impacts. Firstly, to provide a formal definition of lived experience co-production within healthcare simulation and to differentiate this from other forms of service user ‘involvement’. Secondly, to disseminate simulation practitioners’ findings around the best practice for lived experience co-production. Thirdly, to create awareness with service users and persons with lived experience that co-production in healthcare simulation education and practice is common and needed.
The Association for Simulated Practice in Healthcare (ASPiH) have supported the publication of this work through their fee waiver member benefit.
Conception and drafting of the manuscript: LP, drafting and reviewing the manuscript: MM, reviewing and contribution to the manuscript: SMW.
None declared.
The protocol will not generate any new data.
This study will not involve human or animal participants; hence, ethical approval was not sought.
The authors declare no conflicts of interest.
This systematic scoping review protocol was registered on the Open Science Framework (OSF): https://doi.org/10.17605/OSF.IO/Q6SFK.
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.