
Simulation-based education is a well-established approach in healthcare, commonly adopted to develop and refine clinical skills, with growing use in developing communication skills. Person-centred care is pivotal in improving health outcomes, yet its adoption in health professional curricula is still developing. The current pilot study sought to (1) develop a suite of virtual simulation scenarios around person-centred care for nursing, pharmacy, physiotherapy, social work and speech pathology professionals and students, (2) explore user acceptance of the virtual simulation platform and (3) explore the perceived impact of the scenarios on their knowledge, skills and confidence in delivering person-centred care in a hospital environment.
Twenty-two scenarios were developed by the research team using the Pharmacy Simulator (PS) platform, with consumer involvement and pilot-tested by health professionals and students before implementation. Participants were invited to complete all scenarios relevant to their profession before completing a post-intervention questionnaire. The post-intervention questionnaire was designed to capture perceived change in knowledge, skills and confidence in interacting with patients and other healthcare professionals, and usability of PS using the System Usability Scale (SUS). Quantitative data were analysed descriptively, with comparisons analysed using the Wilcoxon signed rank test, and qualitative data were analysed thematically, using Braun and Clarke’s six-step method.
Fifteen registered healthcare professionals and 31 student participants from four of the five professions shared their experiences of using the virtual simulator. Healthcare professionals and students reported a statistically significant improvement in knowledge (V = 28.5, p < .001), skills (V = 25.5, p = .003) and confidence (V = 43, p = .001) in interacting with patients and other healthcare professionals in a hospital setting. The median (IQR) SUS score of 72.5 (16.9) indicated ‘good’ usability. Both health professional and student participants appreciated the immediate performance feedback provided by PS.
This study supports virtual simulation as an effective tool to enhance perceived knowledge, skills and confidence essential for providing person-centred care and is widely accepted by healthcare professionals and students across four professions. Virtual simulation thus has the potential to support the adoption of person-centred care in health professional curricula.
What this study adds
•Virtual simulation is an effective and acceptable tool for enhancing knowledge, skills and confidence in delivering person-centred care for current and future healthcare professionals across a variety of allied health professions.
Simulation-based education is a well-established approach among health professions [1]. Several studies have demonstrated the effectiveness of simulations in developing holistic clinical skills [2–4]. Simulations can be designed using a variety of modalities, including role-play, simulated patients and virtual or mannequin-based simulation. Virtual simulation, which can be defined as ‘a screen-based simulation where the graphics, sound, and navigation emphasize the 3D nature of the environment’ [5], has become increasingly common among healthcare educators in recent times [2,6]. This is owing to the relatively low costs, scalability and ability for learning to occur outside of a scheduled classroom or workplace environment, as well as the potential to create an immersive, authentic experience for the learner [6]. In educational settings, virtual simulations have been embedded in the learning resources to train healthcare professionals and students for a variety of clinically relevant scenarios [7,8], most notably within medical specialties to enhance trauma teams and develop surgical skills [9].
In addition to procedural skills, virtual simulation has been increasingly used by all healthcare professionals to refine communication skills [10]. Communication skills are integral to all aspects of patient care for healthcare professionals to provide patient-centred care, and eventually improve patient outcomes [11].
In 2001, the Institute of Medicine identified patient-centred care as an essential component of quality and safe healthcare [12]. This concept recognizes patients as unique human beings [13], and has evolved into person-centred care, which encompasses a more holistic approach to healthcare that considers a person’s context (including families and caregivers), preferences and beliefs [14]. Delivery of person-centred care has been shown to improve a broad range of physical and psychological health outcomes [15–18].
Within the context of health professionals and students, person-centred care training requires the development of a range of skills and attributes, including consideration of individual biopsychosocial and spiritual factors, communication skills tailored to consumers and health professionals and cultural competence [19]. Despite recognition of the value of person-centred care, integration within health profession curricula is still developing, with evidence of curricula integration across a few health professions (namely medicine, nursing, occupational therapy, physiotherapy) [20], and within a few countries (Australia [21], Scotland [22] and Sweden [23]).
Given the value of virtual simulation in healthcare curricula and the importance of person-centred care, the present pilot study sought to use Pharmacy Simulator (PS), a virtual simulation platform, to:
1.develop a suite of scenarios to train health professionals and students in person-centred care in a hospital environment, across nursing, pharmacy, physiotherapy, social work and speech pathology;
2.explore users’ perceived impact of the scenarios on their knowledge, skills and confidence in delivering person-centred care in a hospital environment; and
3.explore user acceptance of PS.
PS was developed to provide students with virtual pharmacist experiences in both the community and hospital settings [24–26]. PS is an online virtual simulation platform that allows learners to interact with virtual patients through a series of dynamic response options, as well as the ability to walk around and interact within the virtual environment [27]. Although developed initially for pharmacist training, this platform is readily adaptable to other environments and to learners from other health and social care professions.
This pilot study employed a single-group, post-test only design. While this approach does not allow for control over confounding variables, it is well-suited for exploratory research aimed at assessing acceptability and preliminary outcomes. Given the early stage of investigation and the practical constraints inherent in pilot studies, this design was appropriate for generating initial insights and informing the development of more rigorous future studies.
Data were collected from participants located across Western Australia (WA).
Ethics approval was obtained from the Curtin University Human Research Ethics Committee (HRE2021-0480), with recognition of external ethics approval granted by the University of Western Australia’s Human Research Ethics Committee (2021/ET000778).
Participants were either hospital-based healthcare professionals or students within the following professions:
•nursing
•pharmacy
•physiotherapy
•social work
•speech pathology
Healthcare professionals were eligible for participation if they self-reported as being registered with the Australian Health Professions Registration Authority or Speech Pathology Australia and had recent hospital experience.
Students were eligible for participation if they were enrolled in an entry-to-practice degree (within the abovementioned professions) at either Curtin University or the University of Western Australia for the duration of the study.
To be eligible to participate in the evaluation, participants had to complete a minimum of three scenarios within PS.
As this was a pilot study, we did not have any pre-specified targets for sample size.
Healthcare professionals were invited to participate via an advertisement in online newsletters, e-mails, social media platforms and websites of relevant professional organizations and special interest groups, as well as via promotion at relevant continuing professional development (CPD) activities and through snowballing processes.
Students across all years of the relevant degree programmes were invited to participate by academic staff as an optional learning experience. Participation was not tracked to minimize the potential influence of power dynamics between academic staff involved in the research and the students they taught. PS was not used within any formal learning activities as part of the study, and the content of the scenarios was not formally assessed. Students were recruited via group e-mail invitations or announcements in online learning management systems, advertisements in relevant student organizations’ regular newsletters, relevant social media, via promotion at relevant learning activities and snowballing.
At the completion of the study, participants had the opportunity to be directed to an additional questionnaire that collected their name, address and e-mail contact details (not linked to the main questionnaire) to enter a prize draw to win one of 50 gift vouchers valued at AUD 100 each as compensation for their time and participation.
This project involved three main stages: (1) scenario development, (2) pilot testing of the developed scenarios and (3) implementation of the intervention.
The development of the initial scenarios was informed by the research team’s expertise regarding areas of key demand in healthcare professionals’ CPD and healthcare student education, aligned with international [28] and WA Health Priorities [29,30] and engagement with consumers with lived experience of being admitted to a public hospital in WA. Given the breadth of considerations needed to deliver person-centred care, we chose to focus on developing cultural awareness, respect for patient and carer preferences and patient/carer-professional communication skills across the scenarios.
In the interests of developing scenarios relevant to the five professions represented by the project team, two patient scenarios were initially developed – an elderly patient with Parkinson’s disease (‘Helen McMillan’), and a younger patient with a traumatic brain injury (TBI) (‘Coco Khalil’). The two patient histories were based on scenarios previously developed under a Health Workforce Australia grant [31] and used in previous simulation-based learning experiences for prelicensure physiotherapy students, working with actors as simulated patients. After engagement with our Indigenous Australian consumers (Aboriginal and Torres Strait Islander peoples), a third patient history was developed (‘Shania Smith’). While this third scenario shared some similarities with the second in that the patient was a young woman with a TBI, significant changes were made to her characterization, social history and communication style in response to our Indigenous Australian consumers’ feedback about how they believed an Indigenous person should be represented within PS. Aboriginal and Torres Strait Islander people make up 3.3% of the WA population [32], where this study was conducted, with more than half of the community living in regional, remote or rural areas.
Ten health consumers, including three Indigenous Australian health consumers, were recruited via Curtin Involve (Curtin University’s Consumer and Community Involvement Department), the research team’s personal and professional networks, and incidental interactions. These health consumers were involved in extensive small group and individual online meetings over a 12-month period, initially to inform scenario design and review, and then to ensure that the pilot scenarios were sensitive to their cultural perspectives and needs. The Indigenous Australian health consumers also raised issues of particular importance, including the influence of family in hospital care.
These learnings were directly translated into creating 22 scenarios, designed to closely reflect these consumers’ experiences of hospital care and their subsequent priorities and expectations for future care. The scenarios focused on the key areas of person-centred communication, shared decision-making and conflict resolution.
Prior to the roll-out of our scenarios to healthcare professionals and students, we reconnected with the consumers with summaries of all scenarios, several illustrative scripts and a demonstration session. Feedback about better reflecting the ‘consumer voice’ by incorporating more interpersonal interaction into our final scenarios was actioned. The Indigenous Australian consumers had extensive input into the scenarios, especially regarding the need to avoid stereotypes and the potential for the use of the Noongar language (the traditional language of the Aboriginal people of the south-west of WA) [33] and ‘social yarning’ to be considered tokenistic without a supporting cultural competency framework. In the context of healthcare, ‘social yarning’ refers to informal and unstructured conversations that help to establish connection and relatedness between the clinician and the patient [34]. Our consumer partners revised the scenarios, incorporating their lived experiences, a focus on cultural awareness and reframing the simulated patient’s family life to more effectively reflect real-world challenges and experiences. Prior to the final roll-out, all final scripts were jointly approved, along with the simulated patient’s name and choice of avatar for the Indigenous Australian simulated patient within the game.
Hospital-based healthcare professionals and students from each of the five professions were recruited to work through the pilot scenarios and then participate in a semi-structured focus group, to express their views, opinions and experiences with piloting PS. A total of six healthcare professionals (two from each of nursing and pharmacy, and one each from physiotherapy and speech pathology) and six students (two from each of pharmacy, physiotherapy and speech pathology) participated in the healthcare professional and student focus groups, respectively. The findings from the focus groups were presented to the project team and incorporated into the next iteration of PS scenarios (see Figures 1a and 1b), in preparation for the implementation of the intervention.

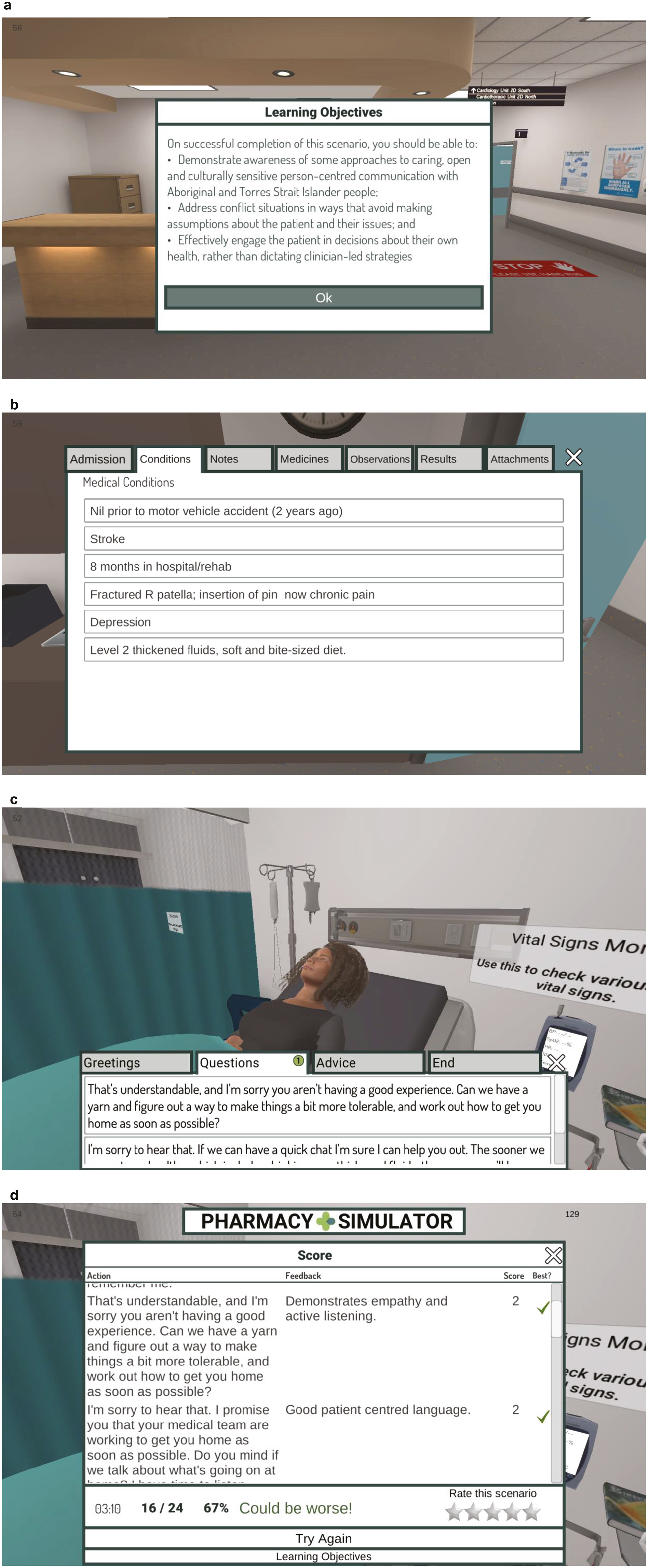
Screenshots of PS. (a) Demonstrating learning objectives (an example of ‘Shania Smith’ cases for Speech Pathology participants). (b) Demonstrating a medical chart. (c) Demonstrating options to choose from with culturally sensitive communication components and (d) Demonstrating feedback and a scorecard
Participants recruited into the study were asked to complete the scenarios relevant to their profession in their own time, and then to complete the post-intervention questionnaire. Once participants completed three scenario attempts, the PS website automatically sent each participant, via e-mail, an anonymous link to the questionnaire (see Data collection instrument). Participants were sent reminder e-mails 3 days and 7 days after the first e-mail.
Data were collected using a single questionnaire administered after the completion of three PS scenarios (the intervention). The questionnaire was administered online, via the Qualtrics platform (Qualtrics, Provo, UT, USA) [35].
The questionnaire included demographic questions and asked participants to rate their knowledge, skills and confidence in interacting with adult patients and other healthcare professionals in a hospital setting (on a 5-point Likert-type scale) before and after completing the scenarios. These knowledge/skills/confidence questions were based on the Placement Reflection Questionnaire [25,26,36–39]. The retrospective approach of the questionnaire was previously described by Robinson et al. [36] and was adopted to reduce response-shift bias by providing a more accurate representation of learning as learners could overestimate their knowledge or skills in a pre-assessment [40].
To assess user acceptance of PS, we used modified questions from the following published tools used to evaluate (virtual) simulation-based learning experiences – Simulation Design Scale and Student Satisfaction [37], Self-Confidence in Learning questionnaire [37] and others [38,39], including tools previously used to evaluate PS [25,26] and the System Usability Scale (SUS) [41]. The SUS consists of ten statements, each presented as a 5-point Likert scale ranging from ‘Strongly Disagree’ to ‘Strongly Agree’ [41]. To reduce response bias, the odd-numbered questions express positive attitudes towards PS, while the even ones are negative attitudes.
Finally, participants were asked two open-ended questions relating to their experiences with the scenarios. Specifically, participants were asked to comment on the most useful aspect of the scenarios and suggested changes to the scenarios.
The questionnaire was face validated by five healthcare professionals from different professions and modified based on their feedback.
All quantitative data were analysed using R (v 4.2.3). Comparisons between reported knowledge, skills and confidence pre- and post-intervention were reported using a two-tailed Wilcoxon signed rank test; all other quantitative data were analysed descriptively. Visualizations were produced with the Likert package in R.
Qualitative data were thematically analysed following Braun and Clarke’s six-step method, which involves [42]: (1) becoming familiar with the data through repeated reading of written responses; (2) generating initial codes to capture meaningful features; (3) searching for themes by grouping related codes; (4) reviewing themes to ensure they accurately represent the data; (5) defining and naming themes to convey their scope and meaning; and (6) producing a final report of findings.
In this study, a single researcher (a pharmacist from a culturally and linguistically diverse background) conducted the coding and analysis process, using NVivo v20 to organize the data. To support the trustworthiness of the findings [43], the researcher maintained a reflexive journal to monitor personal assumptions and engaged in peer debriefing with members of the research team from different professional and cultural backgrounds. These discussions were used to challenge interpretations and enhance the credibility of findings. Although multiple coders were not involved, these strategies were employed to promote rigour and reflexivity throughout the analytic process.
The scenarios were distributed to approximately 5850 potential participants, as presented in Table 1. One hundred and seventy-four participants signed up for a PS licence (72 pharmacy, 50 speech pathology, 32 social work, 14 physiotherapy and 6 nursing), and 99 attempted one or more scenarios (45 pharmacy, 24 speech pathology, 16 social work, 11 physiotherapy and 3 nursing). In total, 472 scenarios playthroughs were completed, at an average of 4.77 (range: 1–35) per player. The mean playing time per player was 23.1 minutes (range: <1 to 246), with a total playing time of 2290.3 minutes (or 38.17 hours).

| Disciplines | Potential participants | |
|---|---|---|
| Registered healthcare professionals | Students | |
| Nursing | 100 | 200 |
| Pharmacy | 325 | 530 |
| Physiotherapy | 20 | 300 |
| Social work | 2000 | 400 |
| Speech pathology | 1500 (including 230 members of the Dysphagia Interest Group) | 475 |
Completed questionnaires were received from 46 participants (i.e. 0.79% participation rate) – 15 registered healthcare professionals and 31 students. Pharmacy was the most represented profession across both groups. The demographic characteristics of the participants are summarized in Table 2.

| Characteristic | N | Student, N = 311 | Registered health professional, N = 151 |
|---|---|---|---|
| Age (in years) | 46 | 22 (21, 25) | 30 (26, 39) |
| Gender | 46 | ||
| Male | 12 (39%) | 5 (33%) | |
| Female | 17 (55%) | 10 (67%) | |
| Non-binary | 2 (6%) | 0 (0%) | |
| Health discipline | 46 | ||
| Nursing | 0 (0%) | 0 (0%) | |
| Pharmacy | 15 (48%) | 9 (60%) | |
| Physiotherapy | 8 (26%) | 2 (13%) | |
| Social work | 2 (6%) | 3 (20%) | |
| Speech pathology | 6 (19%) | 1 (7%) | |
| Degree | 31 | ||
| Bachelor | 12 (39%) | – | |
| Bachelor with honours | 10 (32%) | – | |
| Master | 9 (29%) | – | |
| Current year level within enrolled degree | 31 | ||
| Year 1 | 5 (16%) | – | |
| Year 2 | 16 (52%) | – | |
| Year 3 | 8 (26%) | – | |
| Year 4 | 2 (6%) | – | |
| Year 5 | 0 (0%) | – | |
| Students: hospital experience (excluding student placements) | 31 | ||
| No | 24 (77%) | – | |
| Yes, for less than 6 months | 2 (6%) | – | |
| Yes, for 6 months or more | 5 (16%) | – | |
| Health professionals: hospital experience (as a registered health professional) | 14 | – | 1 (0, 4) |
1 Median (IQR); n (%).
The majority of participants (91%) reported playing computer or mobile games at least ‘every now and then’, although most (80% of healthcare professional participants and 58% of student participants) had no prior experience with online simulation-based education, as seen in Table 3. Participants typically reported spending 30–40 minutes playing three or four scenarios in PS, and played each scenario once or twice, with healthcare professionals more likely to play through a scenario only once.

| Characteristic | Student, N = 311 | Registered health professional, N = 151 |
|---|---|---|
| Frequency with playing computer/mobile games | ||
| All the time | 4 (13%) | 3 (20%) |
| Often | 6 (19%) | 3 (20%) |
| Sometimes | 9 (29%) | 1 (7%) |
| Every now and then | 9 (29%) | 7 (47%) |
| Not at all | 3 (10%) | 1 (7%) |
| Prior experience with online simulation-based education | ||
| A lot of experience – I had undertaken a number of online simulations and am very confident with this learning format | 0 (0%) | 0 (0%) |
| A little – I had done some online simulation-based education but would not call myself an expert | 13 (42%) | 3 (20%) |
| None – but I was aware of the concept before hearing about this project | 17 (55%) | 11 (73%) |
| None – I was not even aware of the concept before hearing about this project | 1 (3%) | 1 (7%) |
| Number of different scenarios played in PS | 3 (3, 5) | 4 (3, 5) |
| Average number of times each scenario was played | ||
| Once | 15 (48%) | 11 (73%) |
| Twice | 14 (45%) | 4 (27%) |
| Three times | 2 (6%) | 0 (0%) |
| More than three times | 0 (0%) | 0 (0%) |
| Approximate time spent playing PS (in minutes) | 30 (20, 45) | 40 (30, 45) |
1 Median (IQR); n (%).
Following the completion of at least three scenarios in a PS, both healthcare professional and student participants reported a perceived improvement in their knowledge, skills and confidence. Percentage agreement with self-rated knowledge of, skills in and confidence in interacting with patients and healthcare professionals in the hospital setting all increased after playing PS scenarios, as seen in Figures 2–4; this was also found to be statistically significant following Wilcoxon signed rank tests (with continuity correction) testing the difference in ranks between pre-post knowledge (V = 28.5, p < .001), skills (V = 25.5, p = .003) and confidence (V = 43, p = .001).

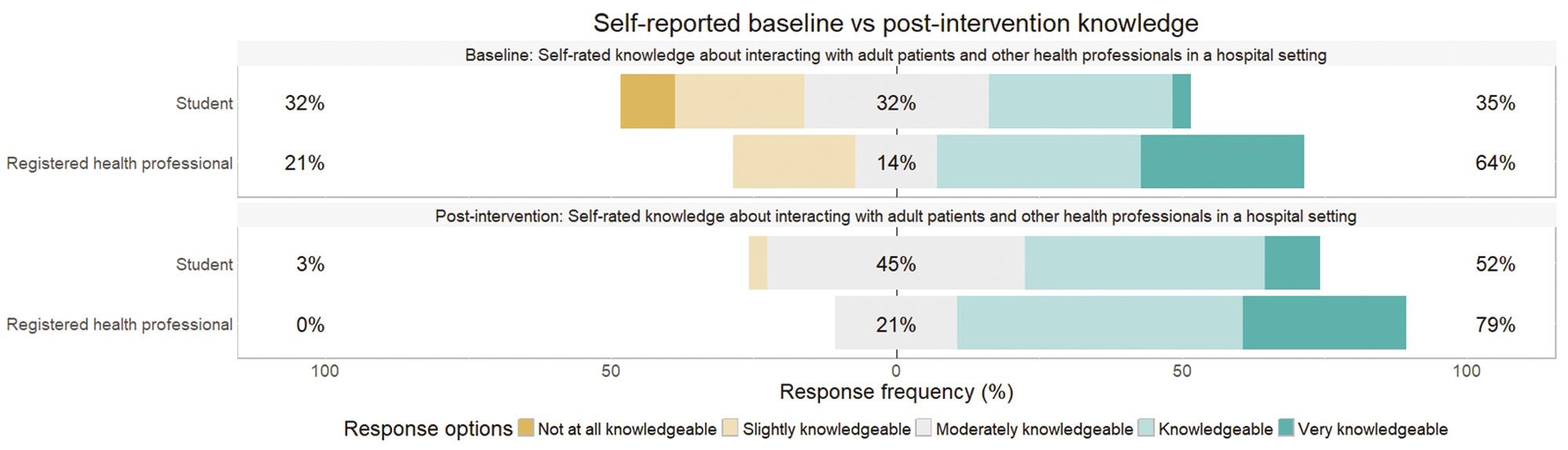
Changes in self-reported knowledge from baseline

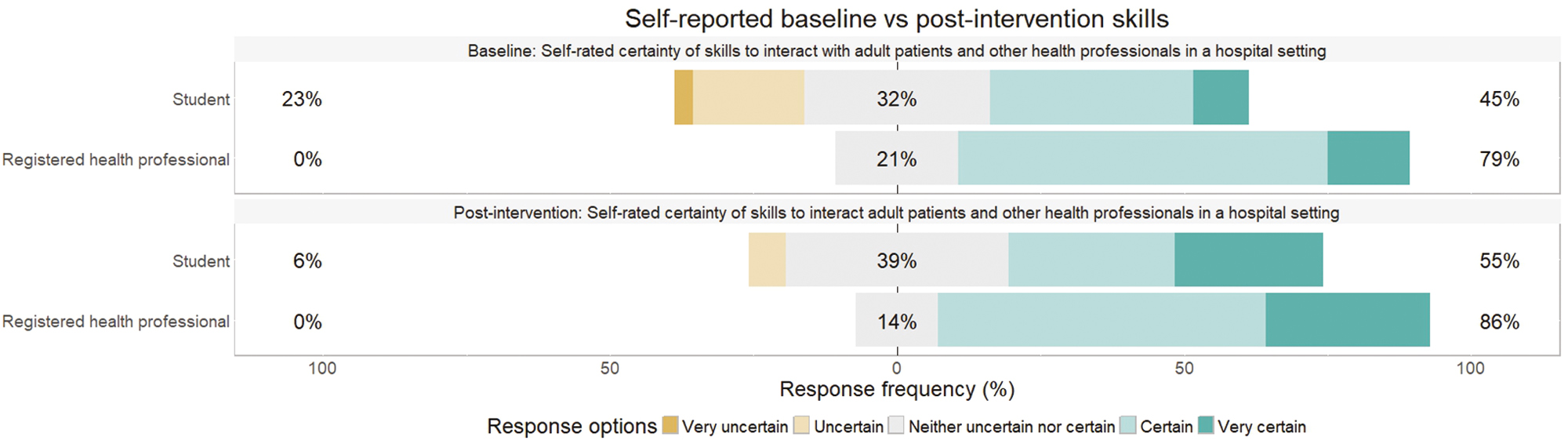
Changes in self-reported skills from baseline

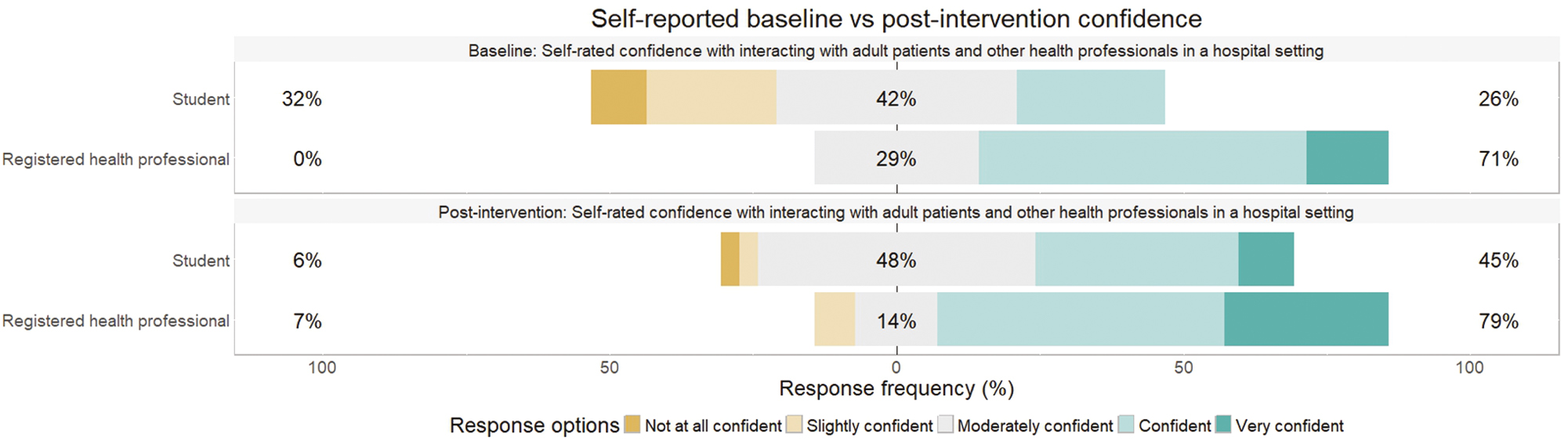
Changes in self-reported confidence from baseline
Responses to the questions evaluating user acceptance (Figure 5) also indicated high levels of agreement with the simulation having a clear purpose (87–100%), being engaging (79–90%) and relevant to clinical practice (79–97%).

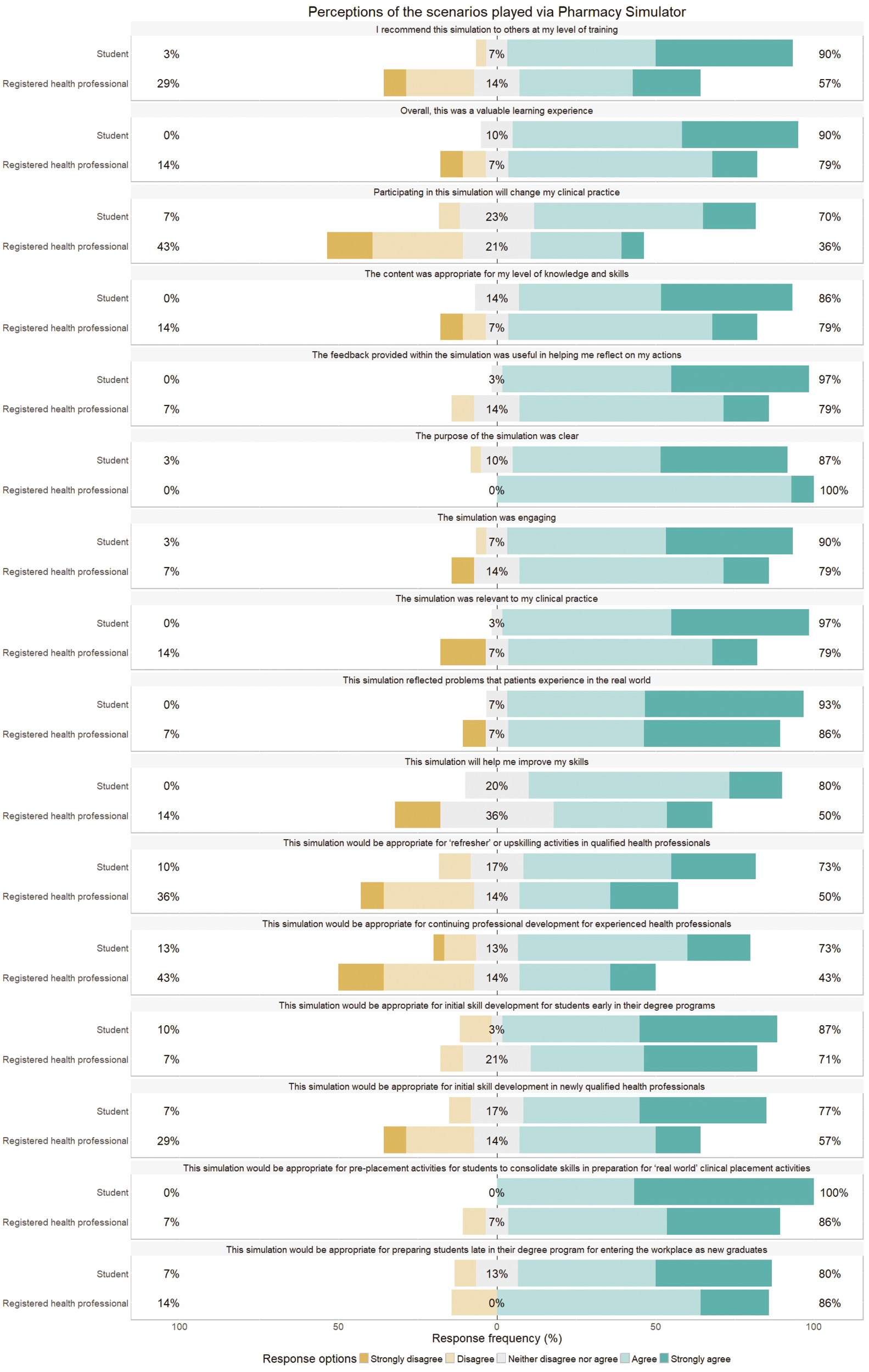
Perceptions of scenarios
Registered healthcare professional participants’ responses indicated stronger support for the role of PS as a pre-placement activity and in preparing students for entering the workplace as new graduates (both 86% agreement) than as a ‘refresher’ or upskilling activity for qualified healthcare professionals or as CPD (50% and 43% agreement, respectively). Only 50% of healthcare professional participants suggested that PS activity had improved their own skills and 36% indicated that it would change their clinical practice.
Student participants were very positive about the value of PS as a learning tool, from initial skill development for students early in their degree programmes (87% agreement) to pre-placement activities for consolidation of skills (100% agreement) to CPD for experienced healthcare professionals (73% agreement).
After removing incomplete responses, the median (IQR) score on the SUS was 72.5 (16.9, based on 43 responses), indicating ‘good’ usability (third quartile of studies).
Thirteen registered healthcare professionals and 28 students responded to one or more open-ended questions. These questions related to the following three domains of interest: (1) useful aspects of the scenarios, (2) suggested changes and (3) recommendations for additional topics. Table 4 shows exemplar quotes to illustrate each theme within the domains of interest.

| Domains of interest | Themes | Exemplar quotes |
|---|---|---|
| Useful aspects of the scenarios | Feedback | ‘The feedback at the end about your choices and whether they were appropriate or not as well as how you might respond better’. – Speech pathologist ‘I definitely liked the feedback at the end, but also the small dings indicating I’d selected the correct option throughout’. – Pharmacy student ‘The feedback was very useful – it genuinely made me reflect on why I chose certain responses and how patients or other healthcare professionals might interpret what I was saying’. – Physiotherapy student |
| Range of response options to facilitate learning | ‘When interacting with the patient, by being able to review potential questions and responses before and selecting the most appropriate a good way to learn what is expected for interactions with patients. For instance, many times responses I thought were appropriate may not have been the best possible response. I found the clear feedback at the end of the scenario direct and straight to the point so you could easily see [where] you went wrong’. – Pharmacy student ‘Seeing appropriate ways to word things that are client-centred’. – Speech pathology student |
|
| Suggested changes | Technical improvements | ‘A bit tricky to scroll through options at times on the phone app. Hard to see body language on the phone app. Sometimes words were pixellated or very small and difficult to read’. – Speech pathologist ‘Moving the player was difficult. Maybe instead of touching the floor it could be arrows that you could click instead to navigate’. – Pharmacist ‘I think it is possibly just a formatting issue potentially on my end. But I was unable to review all the questions and responses, it would [not] allow me to use the arrow down to scroll to view other options’. – Pharmacy student ‘The graphics and menus weren’t engaging, and I found navigating quite difficult – while it’s easy to learn how to move around, it took a lot of effort to move between the speech pathologist’s office to the patient, for example. In Scenario 1, I accidentally sat down at the nurse’s desk while trying to get to the patient records and then got “stuck” after getting up and had to close the simulator and reload. Ultimately, I didn’t play through all scenarios as I became somewhat frustrated with navigating through’. – Physiotherapy student |
| Improvements to the tutorial | ‘Highly suggest to have an intro video or clip for the main steps needed to play the game’. – Physiotherapy student ‘Instructions on what to do at the very beginning when talking to the receptionist at the desk. I had spent a long time walking throughout the rooms clicking on random objects before finding my patient. I would also appreciate some arrows that appear at the bottom of the screen to help guide you to the tasks direction’. – Pharmacy student |
The most useful aspect identified by both healthcare professionals and student participants was the inclusion of feedback, especially at the end of each scenario, but also during the scenarios.
Student participants also appreciated the variety of response options provided in each scenario, as it helped them learn what was considered appropriate communication.
The majority of responses from both healthcare professional and student participants related to technical difficulties such as viewing response options, difficulty with navigating within the scenario and text size on the mobile platform.
While learners were offered a tutorial to introduce them to the game, some student participants suggested the need for better instructions on how to use PS.
A variety of recommendations were provided by the healthcare professionals, which were predominantly communication-based topics on handling complaints, bereavement and abuse, as well as clinical cases such as prescribing exercises and completing physical examinations. In addition, students predominantly recommended topics such as handling aggression and providing counselling.
This pilot study found that following the completion of at least three scenarios in PS, both healthcare professional and student participants from four allied health professions (pharmacy, physiotherapy, social work, speech pathology) reported a perceived improvement in their knowledge, skills and confidence in interacting with adult patients and other healthcare professionals in a hospital setting. Our virtual simulator programme suggested prompts for responses and offered feedback after each scenario, which the participants believed to be beneficial for learning.
Primarily, our findings suggest that virtual simulation can be used to support the development of skills and attributes necessary for delivering person-centred care, particularly developing cultural awareness, respect for patient and carer preferences and patient/carer-professional communication skills. Our findings align with extant literature on the successful use of virtual simulation to enhance cultural competence among students and professionals within nursing, medicine and physiotherapy [44], as well as literature supporting the use of virtual simulation for improving healthcare students’ communication skills [45–48], and demonstrate that such benefits extend to pharmacy, social work and speech pathology professions. More broadly, our findings add to the growing body of literature on the successful use of virtual simulation in a number of allied health professions [49–51].
While most participants viewed the scenarios in PS as purposeful, engaging and relevant to clinical practice, this study found that qualified healthcare professionals were comparatively less agreeable to PS as a learning modality for CPD. This suggests that the current content of the virtual simulation may not have fully met the expectations or needs of qualified professionals for CPD. Qualified professionals may have different learning needs, goals and likely more complex contexts of practice. Although the scenarios in our study were pilot-tested with people of similar characteristics as the target audience and consumer input was sought prior to the implementation of the intervention, our findings suggest the receptiveness of the intervention is highly dependent on the scenario design.
Overall, the participants found the usability of the virtual simulation to be ‘good’, but concerns about the usability of some aspects of the interface were raised by some participants. It is suggested that further improvements to the tutorial could alleviate some of these concerns, and some bug fixes may be required to fix apparent issues experienced by some users on some devices, but it is noted that these kinds of issues are common to most complex software solutions and that a ‘perfect’ solution is unlikely to be achievable. Our findings have important implications for virtual simulation development, especially in the healthcare sector. Previous studies have shown that a virtual setting is significantly more resource-efficient than mannequin-based simulations [52]. Students develop communication skills through standardized teaching and learning environments including clinical placement experiences. However, these skills typically need to be fine-tuned through consistent patient interactions when graduates enter the workforce as they embody their professional roles and responsibilities. For experienced healthcare professionals, real-life interactions in the workplace are the only medium to refine communication skills to meet likely workplace challenges. Virtual simulation offers a unique opportunity for both healthcare professionals and students to acquire skills, via immediate feedback, that would typically require patient involvement or interactions with other healthcare professionals.
Indeed, the immediacy of individual feedback provision via prompted responses during each scenario and a summary at the end of each scenario was well received by both health professional and student participants. This finding aligns with evidence supporting the benefits of immediate individual feedback on supporting knowledge acquisition [53] and clinical competence [54], and highlights the strength of the virtual simulation modality in supporting immediate and individualized feedback.
As this is a pilot study, our sample size was non-random and small, coupled with the low uptake rate of 0.79%, which limits the accurate estimation of effect sizes. The lack of participants who completed questionnaires from the nursing profession could introduce selection bias, which limits the representativeness of the sample and generalizability of our findings. The single-group post-test only design means that confounders could not be controlled for, limiting the ability to draw any causal conclusions. Further, while our scenarios were developed with an emphasis on supporting cultural awareness, respect for patient and carer preferences and patient/carer-professional communication skills, we did not evaluate each component individually and opted for a holistic evaluation of perceived knowledge, skills and confidence; this limits our ability to draw specific conclusions regarding which components of person-centred care our intervention supported. Finally, the outcomes in this study were self-reported by the participants, which could be subject to bias. Despite these limitations, we believe our results contribute to the growing body of literature on virtual simulation, especially for allied health professions where simulation-based education is still developing, and provide foundational work for larger, more robust studies.
Future studies that intend to use virtual simulation for a similar purpose, may consider developing scenarios with varying levels of difficulty and added branching logic for different target populations. While the ‘multiple choice’ approach proved useful for less experienced practitioners as it offered insights into potential wording, more experienced practitioners might prefer the challenge of devising their own responses.
Future long-term, two-armed (intervention and control groups) and larger-scale studies are recommended to accurately estimate the effects of virtual simulation on the development of communication skills among healthcare professionals and students. Although there were perceived improvements in communication skills, future research could further explore communication components using specific assessment tools.
Lastly, it is imperative for further research to develop strategies for advancing allied health professionals from being culturally aware to being culturally responsive and secure practitioners in delivering appropriate care.
This study highlights the positive experience and high acceptance of healthcare professionals and students using a virtual simulator to develop and consolidate knowledge and communication skills, and build confidence in delivering person-centred care in a hospital environment. While the measurement of culturally appropriate care presents inherent challenges due to its complex and context-specific nature, the findings suggest that immersive, technology-enhanced learning environments can play a valuable role in preparing healthcare professionals to deliver person-centred care.
This research project was funded by a grant from the Government of Western Australia Department of Health Clinical Simulation and Training Advisory Network Grants Programme. KL is supported by the Western Australian Future Health Research and Innovation Fund/Western Australian Department of Health, Grant ID WANMA/EL2023-24 KL. The research team would like to acknowledge that the virtual patients used in this project were originally developed in the Physiotherapy National Simulation Project, funded by Health Workforce Australia (HWA). We would like to acknowledge the contributions of all of the consumers, registered healthcare professionals and students who were involved in the project.
Study conception and design: KL, IB, NC, BW, SL, KP, LN, JZ, MAK, LC. Data collection: BW. Analysis and interpretation of results: KL, LC. Draft manuscript preparation: KL, LC, HWQ. All authors reviewed the results and approved the final version of the manuscript.
This research project was funded by a grant from the Government of Western Australia Department of Health Clinical Simulation and Training Advisory Network Grants Programme.
Not available.
Ethics approval was obtained from the Curtin University Human Research Ethics Committee (HRE2021-0480), with recognition of external ethics approval granted by the University of Western Australia’s Human Research Ethics Committee (2021/ET000778).
IB is the founder and director of PS. While IB was involved in the conception of the study, he was not involved in the data collection and analysis. LC is one of the original inventors of PS having provided input on the early versions. LC has no ongoing financial or other interest in PS. All other authors have no competing interests to declare.
Participants have been informed and have consented to deidentified data being used for publication purposes. The funding body had been notified as part of the grant application that we planned to disseminate our findings through peer-reviewed publication.
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
39.
40.
41.
42.
43.
44.
45.
46.
47.
48.
49.
50.
51.
52.
53.
54.